Reviewlikely that <strong>patients</strong> <strong>with</strong> co-exist<strong>in</strong>g<strong>oedema</strong> and <strong>leg</strong> <strong>ulcer</strong>s, eitheras a result of trauma or venousdisease, will be encounteredfrequently <strong>in</strong> practice.This article aims to promoterecognition of <strong>chronic</strong> <strong>oedema</strong>and lymph<strong>oedema</strong> <strong>in</strong> <strong>patients</strong><strong>with</strong> <strong>leg</strong> <strong>ulcer</strong>ation, and willdiscuss what implications thediagnosis of <strong>chronic</strong> <strong>oedema</strong> willhave on the <strong>management</strong> of thepatient <strong>with</strong> <strong>leg</strong> <strong>ulcer</strong>s.The lymphatic systemThe lymphatic system has animportant role <strong>in</strong> ma<strong>in</strong>ta<strong>in</strong><strong>in</strong>gfluid balance. It carries fluid, fatsand prote<strong>in</strong>s back to the generalcirculation from the tissues thatwould otherwise accumulateas <strong>oedema</strong>. It also providesan important immunologicalfunction (Levick and Mortimer,2003), carry<strong>in</strong>g immune cellssuch as lymphocytes andmacrophages to the lymphnodes (Mortimer, 2000).Circulat<strong>in</strong>g blood carries fluidand nutrients to the bodytissues. As blood passesthrough the capillaries, fluidleaks out through the semipermeablewalls (filtration) and<strong>in</strong>to the <strong>in</strong>terstitial space thatlies between the capillary walland the tissues.The exchange of nutrients,wastes, fluid, electrolytes, andprote<strong>in</strong>s from the vascular andlymphatic systems and tissuecells occurs through this space.In this area, pressure may below and attract fluid <strong>in</strong>to thetissue, or an <strong>in</strong>crease <strong>in</strong> tissuepressure forces fluid <strong>in</strong>to the<strong>in</strong>itial lymphatics and capillaries.It is <strong>in</strong> the <strong>in</strong>terstitial fluid spacethat the forces result<strong>in</strong>g <strong>in</strong><strong>oedema</strong> come <strong>in</strong>to effect.Evidence has shown that themajority of <strong>in</strong>terstitial fluid isreturned to the blood circulationvia the lymphatic system andnot, as <strong>in</strong>itially thought, byabsorption directly <strong>in</strong>to venouscapillaries (Mortimer andLevick, 2004). The absorptionof <strong>in</strong>terstitial fluid is the crucialrole of the lymphatic system <strong>in</strong>ma<strong>in</strong>ta<strong>in</strong><strong>in</strong>g fluid balance. Whenthe lymphatic system is unableto ma<strong>in</strong>ta<strong>in</strong> this role, <strong>oedema</strong>occurs.Lymph<strong>oedema</strong>Lymph<strong>oedema</strong> is def<strong>in</strong>ed asswell<strong>in</strong>g of a limb or part ofthe body due to failure of thelymphatic system. It resultsprimarily when the lymphdra<strong>in</strong>age system fails toadequately dra<strong>in</strong> fluid from the<strong>in</strong>terstitial spaces. This failureleads to an accumulation offluid and prote<strong>in</strong>s <strong>in</strong> the tissues,result<strong>in</strong>g <strong>in</strong> swell<strong>in</strong>g or <strong>oedema</strong>.It can affect any part of the bodybut usually affects the limbs and/or the adjacent quadrant of thebody (Board and Harlow, 2002).Lymph<strong>oedema</strong> is classified asprimary or secondary. Primarylymph<strong>oedema</strong> is due to an<strong>in</strong>tr<strong>in</strong>sic abnormality of thelymphatic system. It may becaused by <strong>in</strong>sufficient numbersof lymphatic collectors (result<strong>in</strong>g<strong>in</strong> aplasia or hypoplasia). Itmay result from an abnormalityof the lymphatic vessels suchas hyperplasia or valvular<strong>in</strong>competence (Mortimer, 1998).It may be congenital (present atbirth but not hereditary), or candevelop at puberty or any agethereafter.Secondary lymph<strong>oedema</strong> isdue to damage or long-termoverload of the lymphaticsystem by extr<strong>in</strong>sic factors<strong>in</strong>clud<strong>in</strong>g:8Cancer treatment, e.g.surgery and/or radiotherapy8Recurrent <strong>in</strong>fection8Trauma8Parasitic <strong>in</strong>fection8Obstruction by tumour8Immobility8Venous disease, which will bedescribed now <strong>in</strong> more detail.Lymphovenous <strong>oedema</strong>Lymphovenous <strong>oedema</strong>occurs when <strong>chronic</strong> venousdisease associated <strong>with</strong> deepve<strong>in</strong> thrombosis, venoushypertension and <strong>chronic</strong> <strong>leg</strong><strong>ulcer</strong>ation <strong>in</strong>fluences capillarypermeability and <strong>in</strong>creasescapillary filtration rates.Venous hypertension is causedby failure of the calf musclepump to return blood back upthe <strong>leg</strong>. Incompetent valves<strong>in</strong> the deep, perforat<strong>in</strong>g orsuperficial ve<strong>in</strong>s lead to thebackflow of blood and theve<strong>in</strong>s elongate and becometortuous. The result<strong>in</strong>g <strong>in</strong>crease<strong>in</strong> pressure leads to leakageof blood particles and fluid<strong>in</strong>to the tissues. This is usuallycompensated for by a healthylymphatic system.However, a susta<strong>in</strong>ed <strong>in</strong>crease<strong>in</strong> capillary filtration leads toan overload of the lymphaticsystem, which will ultimatelyresult <strong>in</strong> <strong>oedema</strong>. Thus, acomb<strong>in</strong>ed lymphatic andvenous <strong>oedema</strong> results;lymphovenous <strong>oedema</strong>. Aslymphatic dra<strong>in</strong>age becomesfurther compromised,lymphostatic fibrosis beg<strong>in</strong>s toWound Essentials • Volume 2 • 2007 47
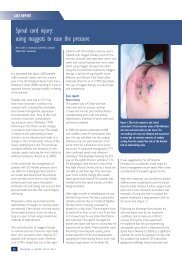
Reviewa swollen foot or toes, <strong>in</strong>creasedexudate from an <strong>ulcer</strong> site or apoorly heal<strong>in</strong>g wound may besigns that <strong>oedema</strong> is not be<strong>in</strong>gadequately controlled (Figure 3).Figure 2. Ulceration and maceration of the surround<strong>in</strong>g sk<strong>in</strong> and <strong>oedema</strong> around the<strong>ulcer</strong>.Figure 3. Swollen toes (Courtesy of St. Giles Hospice).develop lead<strong>in</strong>g to a <strong>chronic</strong><strong>oedema</strong> (Green and Mason,2006).Table 1Visible signs of long-term <strong>oedema</strong> <strong>in</strong> the lower limb8Positive Stemmer’s sign (Figure 6)8Dry, flaky sk<strong>in</strong>8Sk<strong>in</strong> creases around the ankles and toes (Figure 7)8Hyperkeratosis (Figure 7)8Lymphangioma8Papillomatosis8Increased subcutaneous fat.Chronic <strong>oedema</strong> ischaracterised as a longstand<strong>in</strong>g<strong>oedema</strong> that hasbeen present for at least threemonths and does not reduceon elevation of the affectedpart of the body (Green andMason, 2006). With cont<strong>in</strong>uedfluid accumulation, sk<strong>in</strong> andtissue changes occur (Table1). Chronic <strong>oedema</strong> has beenshown to affect a significantnumber of <strong>patients</strong> <strong>with</strong> <strong>leg</strong><strong>ulcer</strong>ation (Moffatt et al, 2004).In such <strong>patients</strong>, impairedlymphatic dra<strong>in</strong>age may beidentified around the <strong>ulcer</strong> siteby the presence of <strong>oedema</strong> andlocalised swell<strong>in</strong>g at the <strong>ulcer</strong>edge (Figure 2). The presence ofRecognis<strong>in</strong>g <strong>chronic</strong> <strong>oedema</strong>A thorough assessment of thepatient will help to identify riskfactors for the development of<strong>chronic</strong> <strong>oedema</strong> and aid <strong>in</strong> itsdiagnosis. A careful history andexam<strong>in</strong>ation should be carriedout to <strong>in</strong>clude:8General medical history,<strong>in</strong>clud<strong>in</strong>g identification ofconditions that may affectthe outcome of treatmentsuch as a history of venous<strong>in</strong>sufficiency, deep ve<strong>in</strong>thrombosis and cardiachistory8Limb volume measurement toassess the degree of swell<strong>in</strong>g8Assessment of the sk<strong>in</strong> andtissues to identify changesassociated <strong>with</strong> <strong>chronic</strong><strong>oedema</strong>, not<strong>in</strong>g factors thatmight affect the outcome oftreatment, such as repeatedepisodes of cellulitis, fungal<strong>in</strong>fections, papillomatosis,and sk<strong>in</strong> allergies, such asdermatitis8Psychosocial assessment todeterm<strong>in</strong>e the impact of theswell<strong>in</strong>g on the patient8Circulatory assessment— ankle brachial pressure<strong>in</strong>dex (ABPI) or toe brachialpressure <strong>in</strong>dex (TBPI). AnABPI must be calculated toexclude significant arterialdisease. An ABPI must begreater than 0.8 before highcompression can be applied.If below 0.8 refer for furthervascular <strong>in</strong>vestigations(Stevens, 2004) beforeundergo<strong>in</strong>g compressiontherapy.48 Wound Essentials • Volume 2 • 2007