<strong>AIDS</strong> in a new millennium: a grim picture <strong>with</strong> glimmers of hopeIn parts of north-east India, widespread injecting drug use provided an easy earlyentry-point <strong>for</strong> <strong>HIV</strong>. In Manipur, the prevalence of <strong>HIV</strong> infection among injecting drugusers shot up from virtually nothing in 1988 to over 70% just four years later, <strong>and</strong> ithas remained at these high levels ever since. Predictably, since almost all injectingdrug users in the state are men, <strong>HIV</strong> then spread to their wives <strong>and</strong> girlfriendsthrough unprotected sex. Around 2.2% of pregnant women in Manipur tested positive<strong>for</strong> <strong>HIV</strong> in 1999. In other states, even higher levels of <strong>HIV</strong> have been recordedamong pregnant women. Most cases of infection appear to have been acquired fromhusb<strong>and</strong>s who had been infected in turn by sex workers, themselves part of a longerchain of transmission. By the mid-1990s, a quarter or more of sex workers in citiessuch as New Delhi, Hyderabad, Madurai, Pune, Tirupati <strong>and</strong> Vellore tested positive<strong>for</strong> <strong>HIV</strong>. In Mumbai, the prevalence of <strong>HIV</strong> infection among sex workers reached 71%in 1997.The Indian Government <strong>and</strong> individual state governments have launched preventionprogrammes to reduce high-risk sex, <strong>and</strong> there is evidence that in some states theseprogrammes are resulting in safer behaviour (see Box 2 below). If current preventionef<strong>for</strong>ts can be scaled up <strong>and</strong> sustained, India may be able to bring down the ratesof <strong>HIV</strong> infection in particularly exposed groups <strong>and</strong> avert a widespread heterosexualepidemic.Box 2. A measure of success: changing behaviour in Tamil NaduIt is important to collect in<strong>for</strong>mation about the behaviour that spreads <strong>HIV</strong> as well asabout the progress of the virus itself. It is very difficult to track new infectionsbecause <strong>HIV</strong> typically causes no symptoms <strong>for</strong> many years. The proportion of thepopulation infected – the <strong>HIV</strong> prevalence rate – is not a reliable indicator of recenttrends in risky behaviour; it encompasses all <strong>people</strong> <strong>with</strong> <strong>HIV</strong>, including those whobecame infected many years previously. In<strong>for</strong>mation about behaviour can be a usefulearly warning in countries where the virus is rare or confined to particular groups<strong>and</strong> can help explain changes in <strong>HIV</strong> prevalence in populations where the virus isalready well established. Behavioural in<strong>for</strong>mation also helps to monitor progress inpromoting safe sexual behaviour <strong>and</strong> hence shows the impact of national preventionprogrammes.In countries where <strong>HIV</strong> is widespread, data on sexual behaviour are collected frommen <strong>and</strong> women in households chosen r<strong>and</strong>omly as representative of the generalpopulation. In countries where <strong>HIV</strong> infection is less prevalent, it is more common toconduct surveys among occupational groups – such as soldiers, factory workers orsex workers – that typify different levels of risk <strong>and</strong> that can be contacted regularlyover time.When surveillance systems in the Indian state of Tamil Nadu – home to some 60 million<strong>people</strong> – showed that <strong>HIV</strong> infection rates among pregnant women were rising,–––>13
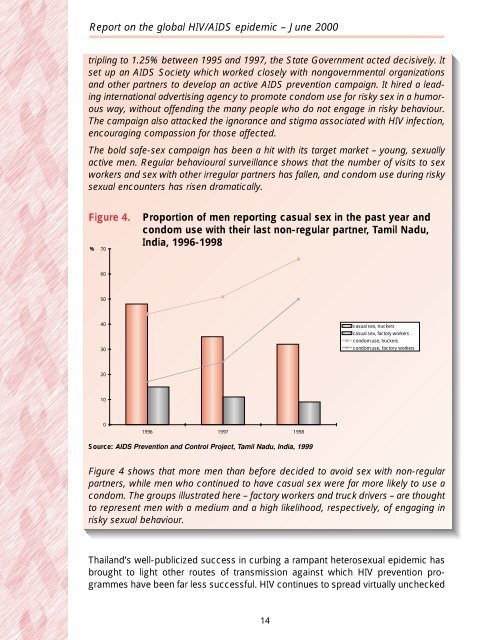
Report on the global <strong>HIV</strong>/<strong>AIDS</strong> epidemic – June 2000tripling to 1.25% between 1995 <strong>and</strong> 1997, the State Government acted decisively. Itset up an <strong>AIDS</strong> Society which worked closely <strong>with</strong> nongovernmental organizations<strong>and</strong> other partners to develop an active <strong>AIDS</strong> prevention campaign. It hired a leadinginternational advertising agency to promote condom use <strong>for</strong> risky sex in a humorousway, <strong>with</strong>out offending the many <strong>people</strong> who do not engage in risky behaviour.The campaign also attacked the ignorance <strong>and</strong> stigma associated <strong>with</strong> <strong>HIV</strong> infection,encouraging compassion <strong>for</strong> those affected.The bold safe-sex campaign has been a hit <strong>with</strong> its target market – young, sexuallyactive men. Regular behavioural surveillance shows that the number of visits to sexworkers <strong>and</strong> sex <strong>with</strong> other irregular partners has fallen, <strong>and</strong> condom use during riskysexual encounters has risen dramatically.Figure 4.%70Proportion of men reporting casual sex in the past year <strong>and</strong>condom use <strong>with</strong> their last non-regular partner, Tamil Nadu,India, 1996-199860504030casual sex, truckerscasual sex, factory workerscondom use, truckerscondom use, factory workers201001996 1997 1998Source: <strong>AIDS</strong> Prevention <strong>and</strong> Control Project, Tamil Nadu, India, 1999Figure 4 shows that more men than be<strong>for</strong>e decided to avoid sex <strong>with</strong> non-regularpartners, while men who continued to have casual sex were far more likely to use acondom. The groups illustrated here – factory workers <strong>and</strong> truck drivers – are thoughtto represent men <strong>with</strong> a medium <strong>and</strong> a high likelihood, respectively, of engaging inrisky sexual behaviour.Thail<strong>and</strong>’s well-publicized success in curbing a rampant heterosexual epidemic hasbrought to light other routes of transmission against which <strong>HIV</strong> prevention programmeshave been far less successful. <strong>HIV</strong> continues to spread virtually unchecked14