Kaiser Permanente Health Plan Northern California Region
Kaiser Permanente Health Plan Northern California Region
Kaiser Permanente Health Plan Northern California Region
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
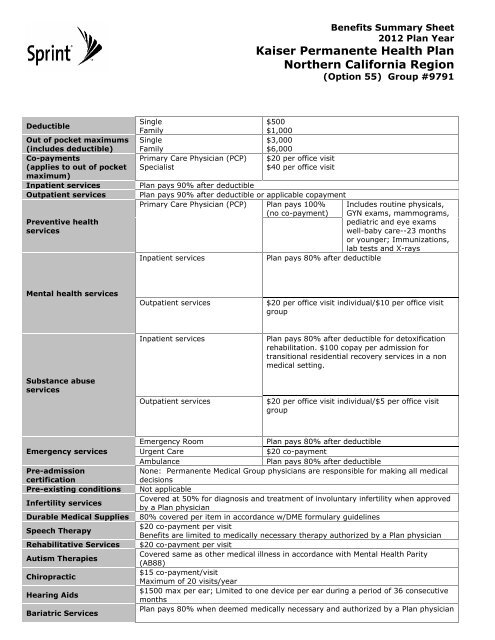
Benefits Summary Sheet<br />
2012 <strong>Plan</strong> Year<br />
<strong>Kaiser</strong> <strong>Permanente</strong> <strong>Health</strong> <strong>Plan</strong><br />
<strong>Northern</strong> <strong>California</strong> <strong>Region</strong><br />
(Option 55) Group #9791<br />
Deductible<br />
Single<br />
Family<br />
$500<br />
$1,000<br />
Out of pocket maximums Single<br />
$3,000<br />
(includes deductible) Family<br />
$6,000<br />
Co-payments<br />
Primary Care Physician (PCP) $20 per office visit<br />
(applies to out of pocket<br />
maximum)<br />
Specialist<br />
$40 per office visit<br />
Inpatient services <strong>Plan</strong> pays 90% after deductible<br />
Outpatient services <strong>Plan</strong> pays 90% after deductible or applicable copayment<br />
Primary Care Physician (PCP) <strong>Plan</strong> pays 100% Includes routine physicals,<br />
(no co-payment) GYN exams, mammograms,<br />
Preventive health<br />
pediatric and eye exams<br />
services<br />
well-baby care--23 months<br />
or younger; Immunizations,<br />
lab tests and X-rays<br />
Inpatient services<br />
<strong>Plan</strong> pays 80% after deductible<br />
Mental health services<br />
Substance abuse<br />
services<br />
Outpatient services $20 per office visit individual/$10 per office visit<br />
group<br />
Inpatient services<br />
<strong>Plan</strong> pays 80% after deductible for detoxification<br />
rehabilitation. $100 copay per admission for<br />
transitional residential recovery services in a non<br />
medical setting.<br />
Outpatient services $20 per office visit individual/$5 per office visit<br />
group<br />
Emergency Room <strong>Plan</strong> pays 80% after deductible<br />
Emergency services Urgent Care $20 co-payment<br />
Ambulance <strong>Plan</strong> pays 80% after deductible<br />
Pre-admission<br />
None: <strong>Permanente</strong> Medical Group physicians are responsible for making all medical<br />
certification<br />
decisions<br />
Pre-existing conditions Not applicable<br />
Infertility services<br />
Covered at 50% for diagnosis and treatment of involuntary infertility when approved<br />
by a <strong>Plan</strong> physician<br />
Durable Medical Supplies 80% covered per item in accordance w/DME formulary guidelines<br />
Speech Therapy<br />
$20 co-payment per visit<br />
Benefits are limited to medically necessary therapy authorized by a <strong>Plan</strong> physician<br />
Rehabilitative Services $20 co-payment per visit<br />
Autism Therapies<br />
Covered same as other medical illness in accordance with Mental <strong>Health</strong> Parity<br />
(AB88)<br />
Chiropractic<br />
$15 co-payment/visit<br />
Maximum of 20 visits/year<br />
Hearing Aids<br />
$1500 max per ear; Limited to one device per ear during a period of 36 consecutive<br />
months<br />
Bariatric Services<br />
<strong>Plan</strong> pays 80% when deemed medically necessary and authorized by a <strong>Plan</strong> physician
Choice of doctors and<br />
facilities<br />
Prescription drugs<br />
Customer service<br />
Member selects a Primary Care Physician (PCP)<br />
Generally no referrals are required. Please check with the plan regarding specialists.<br />
For provider listing, type www.kaiserpermanente.org in your web browser<br />
Retail $10 generic co-payment; $25 brand copayment/30<br />
day supply<br />
Mail $20 generic co-payment; $50 brand copayment/100<br />
day supply<br />
20% co-payment for testing supplies<br />
50% co-payment for drugs for the treatment of infertility (as part of and approved<br />
treatment) and sexual dysfunction (maximum dosage limit of 27 doses for 100-day<br />
supply)<br />
<strong>Kaiser</strong> Member Services:<br />
(800) 464-4000<br />
Life Events are events that affect or alter your life. It is important for you to<br />
understand the benefit choices that you make when you are first eligible and during<br />
subsequent annual enrollment periods, because your benefits are binding and cannot<br />
be changed unless you experience a qualified Life Event. These Qualified Life Events<br />
can be found in the Life Events Section of the Summary <strong>Plan</strong> Description, on i-<br />
Life Events<br />
Connect. To be eligible to make a Benefit Change, you must contact the Employee<br />
Help Line (EHL) to Request the Change during business hours CT, no later than the<br />
30 th calendar day after the date of the event (or 60 th calendar day after a<br />
Medicaid/CHIP-related Life Event). If you do not satisfy the enrollment<br />
requirements, coverage will not be added and no benefits for expenses incurred will<br />
be payable.<br />
Note: This represents a summary of coverage. Details in the Evidence of Coverage (EOC) govern in all cases.