Prof Chia Boon Lock receives the SMA Honorary ... - nuhcs
Prof Chia Boon Lock receives the SMA Honorary ... - nuhcs
Prof Chia Boon Lock receives the SMA Honorary ... - nuhcs
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
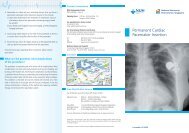
Carotid Artery Stenting<br />
Dr Teo Swee Guan, Cardiac Dept @ NUH<br />
Percutaneous transluminal angioplasty and stenting have become<br />
an established <strong>the</strong>rapeutic modality for coronary and peripheral<br />
arterial diseases, complementing surgical treatment. The<br />
application of this technique in carotid artery stenosis is an<br />
expected progression. The perceived advantages of carotid artery<br />
stenting (CAS) compared to carotid endarterectomy (CEA)<br />
include avoidance of general anes<strong>the</strong>sia and open surgical incision,<br />
shorter procedural time and hospitalization, and increased<br />
patients’ acceptance.<br />
Since FDA approval of CAS in 2004, it has been increasingly<br />
used for patients considered as high risk for surgery. In contrast to<br />
most endovascular peripheral arterial interventions, CAS<br />
represents a more challenging procedure because it requires <strong>the</strong><br />
use of smaller guidewire system (0.014-in vs 0.035-in guidewire<br />
system as in peripheral intervention), distal embolic protection<br />
device and rapid exchange system (vs. over-<strong>the</strong>-wire system). The<br />
use of long guiding sheath via common femoral artery to perform<br />
balloon angioplasty and stenting also represents new challenge for<br />
physicians with less CAS experience.<br />
CEA has long been <strong>the</strong> gold standard for <strong>the</strong> treatment of<br />
carotid artery stenosis. In North American Symptomatic Carotid<br />
Endarterectomy Trial (NASCET), symptomatic patients with<br />
carotid artery stenosis (70-99%) in CEA arm compared to medical<br />
group had higher perioperative stroke/death (5.8% vs 3.3%) but<br />
significantly lower major/fatal ipsilateral stroke at 2 years (2.5%<br />
vs 13.1%, p