Coronary Angioplasty and Stenting - nuhcs
Coronary Angioplasty and Stenting - nuhcs
Coronary Angioplasty and Stenting - nuhcs
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
What should I do?<br />
1. Please inform your doctor of any allergy, particularly allergies to<br />
seafood, iodine, X-ray contrast medium, <strong>and</strong> pain relieving medications.<br />
2. Please inform your doctor if you have a history of peptic ulcer disease,<br />
recent strokes, bleeding tendencies or planning surgery within the<br />
year.<br />
3. If you are suffering from diabetes mellitus <strong>and</strong> are taking a medication<br />
called metformin, please inform your doctor as you may need to stop<br />
this medication before the procedure.<br />
4. Upon discharge, you will usually be given two blood clotting medications<br />
– aspirin <strong>and</strong> either ticlopidine, clopidogrel or prasugrel. The latter<br />
medicines may be discontinued after 1 month or a year depending on<br />
your situation. Your cardiologist will determine the optimal duration<br />
for you. You should however continue to take aspirin indefinitely to<br />
prevent future heart attacks, unless instructed by your doctor.<br />
What is the likelihood of a successful procedure?<br />
The likelihood of success depends on the nature of your coronary narrowing,<br />
<strong>and</strong> is usually 95%. In about 5% of cases, the procedure may be unsuccessful<br />
<strong>and</strong> the artery remains narrowed. In very few patients (less than 1%),<br />
urgent bypass surgery may be required if the procedure is complicated.<br />
Narrowing of the coronary artery may recur, usually in the 12 months<br />
following initial successful angioplasty or stenting. This usually manifests<br />
as a recurrence of chest discomfort. You should seek medical attention<br />
or inform your doctor immediately if you have a recurrence of chest pain.<br />
What are the potential risks/complications?<br />
In general, major complications which include heart attacks, abnormal<br />
heart rhythm, stroke <strong>and</strong> death, occur in less than 1% of patients undergoing<br />
PTCA. This risk depends on the complexity of coronary narrowing <strong>and</strong> the<br />
patient's underlying medical conditions. Other less serious complications<br />
occur in 1-3% <strong>and</strong> include bleeding from the puncture site, bruising <strong>and</strong><br />
swelling of the puncture site, <strong>and</strong> blood clot formation in the artery where<br />
the sheath is inserted. Overall, the procedure is very safe <strong>and</strong> well tolerated.<br />
Contact information<br />
NUH Angiography Centre<br />
Main Building 1, Level 2<br />
Opening Hours: 8.30 am - 5.30 pm (Mon - Fri)<br />
(except on Public Holidays)<br />
For appointments, please contact<br />
Tel: (65) 6772 2002<br />
Email: appointment@nuh.com.sg<br />
For International Patients And Visitors<br />
The International Patients Liaison Centre (IPLC) is a one-stop service centre to support<br />
all the medical needs of our foreign patients<br />
Tel<br />
: (65) 6779 2777 (24-Hours Helpline)<br />
Fax : (65) 6777 8065<br />
Website : www.nuh.com.sg/iplc.html<br />
National University Hospital<br />
5 Lower Kent Ridge Road, Singapore 119074<br />
Tel: 6779 5555 Fax: 6779 5678 Website: www.nuh.com.sg<br />
Location<br />
Free Shuttle Bus Service<br />
Free Shuttle Bus Service from Dover MRT Station to NUH<br />
Operation hours<br />
: 8.00 am – 8.30 pm (Mondays – Fridays)<br />
8.00 am – 2.00 pm (Saturdays)<br />
Not available on Sundays <strong>and</strong> Public Holidays<br />
Dover/NUH : 1. Dover MRT Station (opposite Singapore Polytechnic)<br />
passenger pickup/ 2. Main Building, Lobby Entrance (near roundabout)<br />
drop off point 3. Kent Ridge Wing, Level 3, South Entrance<br />
For more information on Shuttle Bus schedule, you may go to NUH internet website<br />
at www.nuh.com.sg<br />
<strong>Coronary</strong> <strong>Angioplasty</strong><br />
<strong>and</strong> <strong>Stenting</strong><br />
Information in this brochure is given as a guide only <strong>and</strong> does not replace medical advice from your<br />
doctor. Please seek the advice of your doctor if you have any questions related to the surgery, your health<br />
or medical condition.<br />
Information is correct at time of printing (Aug 2009) <strong>and</strong> subject to revision without notice.
What is <strong>Coronary</strong> <strong>Angioplasty</strong> <strong>and</strong> <strong>Stenting</strong>?<br />
The coronary arteries supply blood to the heart muscles. When they are<br />
narrowed by a process called atherosclerosis (blood vessel wall hardening),<br />
the heart’s blood supply may become insufficient, especially during periods<br />
of physical exertion or stress. This frequently causes chest discomfort (angina<br />
pectoris) but may also manifest as breathlessness, irregular heart rhythm,<br />
fatigue <strong>and</strong> even heart attack.<br />
<strong>Coronary</strong> artery narrowings may be treated using medications that reduce<br />
the heart’s dem<strong>and</strong> for blood, or by procedures aimed at restoring the<br />
heart’s blood supply. The two most common methods to increase blood<br />
supply are coronary artery bypass surgery <strong>and</strong> coronary angioplasty, sometimes<br />
abbreviated as PTCA (Percutaneous Transluminal <strong>Coronary</strong> <strong>Angioplasty</strong>). In<br />
PTCA, a balloon mounted on a thin tube (catheter) is advanced into your<br />
heart artery until it lies within the narrow area. The balloon is then inflated<br />
to dilate the narrowing. Upon balloon deflation, the arterial narrowing is<br />
often significantly reduced. This is usually followed by another procedure<br />
called stenting where a small metal coil is placed.<br />
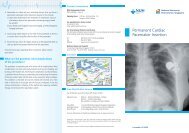
100%<br />
Blockage<br />
Balloon<br />
Wire<br />
<strong>Coronary</strong> arteriogram showing<br />
complete occlusion of the right<br />
coronary artery<br />
After insertion of a wire, a<br />
balloon is inflated at the site<br />
of the blockage<br />
A thin balloon at the end of a catheter is inflated to compress plaque.<br />
This procedure is often used instead of bypass surgery.<br />
The stent provides support to the narrowed segment of the coronary artery<br />
after angioplasty, preventing the artery from collapsing <strong>and</strong> reducing the<br />
likelihood of repeat narrowing. Modern stents are made of stainless steel<br />
or a cobalt chromium alloy <strong>and</strong> are inert to the body. Some stents also have<br />
a medication coating <strong>and</strong> these may be preferred in certain situations to<br />
further reduce the chance of repeat narrowing of the heart arteries. In some<br />
situations, stents can be placed directly over the narrowed segments (direct<br />
stenting) without prior balloon dilatation.<br />
Arterial<br />
Flow<br />
Restored<br />
Following successful stenting,<br />
normal blood flow is restored<br />
What can I expect?<br />
Undergoing PTCA (percutaneous transluminal coronary angioplasty) is very<br />
similar to having a coronary angiogram. After injection of a local anaesthetic,<br />
a plastic tube called a sheath is inserted in a large artery in the groin or<br />
wrist. Through this sheath, a long <strong>and</strong> narrow tube (catheter) is advanced<br />
to the mouth of the narrowed coronary artery. A coronary angiogram is<br />
done first to provide a “road map” for the PTCA. A fine wire is then threaded<br />
through the catheter <strong>and</strong> advanced into the coronary artery. This wire serves<br />
as a rail over which the balloon catheter is finally delivered into the artery<br />
<strong>and</strong> the balloon positioned over the area of narrowing. <strong>Stenting</strong> is similarly<br />
carried out. The procedure may take from 1 /2 to 2 hours, depending on the<br />
complexity of the diseased artery.<br />
Following successful PTCA, you will be monitored in a special monitoring<br />
ward. During this period, the sheath may be kept in your groin artery for<br />
4 to 6 hours. Alternatively, the sheath may be removed in the laboratory<br />
immediately after the procedure if the situation allows. Upon removal of<br />
the sheath, the puncture site will be compressed for about 30 minutes to<br />
ensure that there is no bleeding. You will have to remain in bed for several<br />
hours or until the following day following a groin puncture to ensure<br />
sufficient healing of the puncture site before walking. Your cardiologist<br />
will determine how long you need to be in bed before ambulation. Some<br />
blood tests <strong>and</strong> ECGs may be performed to monitor your condition. If<br />
there is no complication, most patients can be discharged on the same<br />
day or day after.