Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Closing Rem a rk s<br />
In This<br />
I S S U E<br />
• C A S E S T U D Y<br />
Understanding Atrial Septal Rim<br />
Anatomy Using Echocardiography<br />
Prior to Placement of the<br />
GORE ® HELEX Septal Occluder<br />
• F E A T U R E D T O P I C<br />
Creating Products through<br />
Collaborative Innovation<br />
• I N T H E N E W S<br />
<strong>Gore</strong> Provides Update on<br />
<strong>Gore</strong> REDUCE Clinical Study<br />
for Patent Foramen Ovale (PFO)<br />
Closure<br />
• U P C O M I N G E V E N T S<br />
P E R F O R M A N C E b y d e s i g n<br />
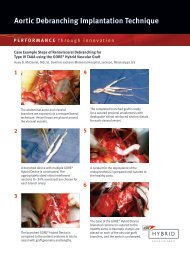
C A S E S T U D Y<br />
Understanding Atrial Septal Rim Anatomy<br />
Using Echocardiography Prior to Placement<br />
of the GORE ® HELEX Septal Occluder<br />
James W. Mathewson, MD, FACC, FASE<br />
Eller Congenital Heart Institute, St. Joseph Hospital and <strong>Medical</strong> Center, Phoenix,<br />
Arizona and the Northern Arizona Congenital Heart Center, Flagstaff, Arizona<br />
The advent of devices for ASD closure without invasive surgery has prompted a need to more<br />
fully understand the anatomy of the atrial septum. Successful closure requires the creation of<br />
a “sandwich” wherein the left and right atrial components of the device (the bread) enclose<br />
the rims (the meat) surrounding the defect. The absence of a large segment of rim can be<br />
problematic. The purpose of this article is to describe how to echocardiographically visualize<br />
atrial septal anatomy and point out those conditions wherein a surgical approach<br />
is preferred.<br />
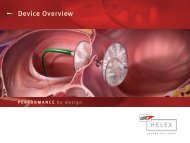
The GORE ® HELEX Septal Occluder is pictured in Figure 1. Figure 2 shows its placement across<br />
a hypothetical ideal ASD with fully deployed right and left atrial disks. The GORE ® HELEX<br />
Septal Occluder is designed for closure of small to medium sized holes usually less than<br />
2 cm in diameter. Before attempting to close such defects, one must first determine existing<br />
ASD diameter, location, and rim anatomy.<br />
Continued on inside cover...<br />
Fall 2010 • Issue XI
Understanding Atrial Septal Rim Anatomy Using Echocardiography Prior<br />
to Placement of the GORE ® HELEX Septal Occluder Continued from cover...<br />
Figure 1. The GORE ® HELEX Septal Occluder.<br />
Right Atrial Disk<br />
Left Atrial Disk<br />
Right<br />
Superior<br />
Vena Cava<br />
Right<br />
Atrium and<br />
Appendage<br />
Inferior<br />
Vena Cava<br />
Left<br />
Innominate<br />
Vein<br />
Tricuspid<br />
Valve<br />
Figure 3. Frontal view of normal right atrial 3D<br />
anatomy.<br />
immediately behind the ascending aorta.<br />
The AI, or antero-inferior rim, is located<br />
just above the septal component of the<br />
tricuspid valve. The PI, or postero-inferior<br />
rim, is located along the back wall of the<br />
atrium just superior to the entrance of the<br />
inferior vena cava into the right atrium. The<br />
PS, or postero-superior rim, is also located<br />
along the posterior wall of the atrium but<br />
superiorly and just adjacent to the entrance<br />
of the right superior pulmonary vein into<br />
the left atrium.<br />
Prior to contemplating ASD closure<br />
with any device, one must first identify<br />
S.V.C.<br />
Ao.<br />
P.T.<br />
Figure 2. Implanted GORE ® HELEX Septal Occluder<br />
in hypothetical heart model.<br />
Figures 3 and 4 show 3D computed<br />
tomography images of normal human right<br />
atrial anatomy together with the superior<br />
vena cava, left innominate and azygous<br />
veins. Figure 5 shows adjoining left atrial<br />
anatomy (violet), tricuspid and mitral valves,<br />
and the position of the interatrial septum.<br />
Figure 6 depicts intra-atrial anatomy with<br />
the anterior right atrial wall flapped open<br />
to the right. Displayed are the positions<br />
of the fossa ovalis (foramen ovale),<br />
eustachian valve (VE), and the superior<br />
and inferior vena cava. Note the position of<br />
the ascending aorta which is anterior and<br />
superior to the fossa ovalis, the location<br />
of most secundum ASDs.<br />
Atrial Septal Rim Anatomy<br />
The rims surrounding an ASD in both<br />
humans and canines can be divided<br />
arbitrarily into five zones or regions<br />
each of which is easily identified by<br />
trans-thoracic (TTE), trans-esophageal<br />
(TEE), and intracardiac echocardiographic<br />
(ICE) methods. Figure 7 is an artist’s<br />
rendering of these five rims and their<br />
anatomic locations.<br />
The locations of each rim can be<br />
conceptualized in terms of their anatomic<br />
positions relative to the anterior, posterior,<br />
Tricuspid<br />
Valve<br />
Azygous<br />
Vein<br />
Atrial<br />
Septum<br />
Figure 4. Left side view of normal right atrium.<br />
Plane<br />
of Atrial<br />
Septum<br />
Tricuspid<br />
Valve<br />
Appendage<br />
Mitral Valve<br />
Figure 5. Right and left atria together in situ.<br />
superior, and inferior orientation of the<br />
heart as it sits in the chest. The S or superior<br />
rim is located just inferior to the entrance of<br />
the superior vena cava into the right atrium<br />
and below the right pulmonary artery as<br />
it passes behind the superior vena cava.<br />
The AS, or antero-superior rim, is located<br />
P.C.B.<br />
F.O.<br />
C.S.<br />
R.V.<br />
V.E.<br />
R.C.A.<br />
Figure 6. Atrial septal anatomy with RA free wall<br />
opened to right (arrows): Ao: aorta; CS: coronary<br />
sinus; FO: fossa ovalis; PT: pulmonary trunk; RCA:<br />
right coronary artery; RV: right ventricle; SVC:<br />
superior vena cava; VE; eustachian valve.<br />
RUPV<br />
SVC<br />
PS<br />
IVC<br />
PI<br />
S<br />
AS<br />
AI<br />
AAO<br />
P<br />
Tricuspid Valve<br />
Septal Leaflet<br />
Figure 7. Artist’s rendering of the five septal rims.<br />
A: anterior; AAo: ascending aorta; AS: anterosuperior<br />
rim; AI: antero-inferior rim; I: inferior;<br />
IVC: inferior vena cava; P: posterior; PI: posteroinferior<br />
rim; PS: postero-superior rim; RUPV: right<br />
upper pulmonary vein; S: superior rim; SVC:<br />
superior vena cava.<br />
I<br />
S<br />
A
Right Upper<br />
Pulmonary<br />
Vein<br />
PS Rim<br />
AI Rim<br />
Crux<br />
S Rim<br />
PI Rim<br />
AS Rim<br />
PS Rim<br />
AI Rim<br />
Crux<br />
S Rim<br />
PI Rim<br />
AS Rim<br />
Figure 8. TTE apical four chamber view; beam cuts<br />
front to back from apex in front to the upper atria<br />
posteriorly.<br />
these five rims to be sure there is adequate<br />
rim to retain the device. Because the most<br />
common imaging modalities used at or prior<br />
to the time of device placement are TE and<br />
trans-esophageal echocardiography TEE,<br />
this report will emphasize how each rim is<br />
identified using these two technologies.<br />
Trans-Thoracic Echocardiography-TTE<br />
For TTE, the pertinent views for seeing the<br />
five rims are apical four chamber (AI and PS<br />
rims), para-sternal short axis (AS rim), and<br />
sub-costal long axis (S and PI rims). Figure<br />
8 shows a typical apical four chamber view<br />
which cuts the heart from the ventricular<br />
apex in front to the posterior superior atrial<br />
base at the level of insertion of the right<br />
and left upper pulmonary veins. The AI rim<br />
is adjacent to the AV valve insertion into the<br />
crux of the heart. The PS rim is just proximal<br />
to insertion of the right upper pulmonary<br />
vein into the left atrium.<br />
The PI and S rims are identified from the<br />
sub-costal long axis view as seen in Figure<br />
9. In this view, the superior and inferior<br />
vena cava are intersected together with the<br />
long axis of the right atrium. One identifies<br />
the superior rim just beneath the right<br />
pulmonary artery as it passes behind the<br />
Figure 9. TTE sub-costal long axis cuts through<br />
IVC, SVC, and RA showing S and PI rims.<br />
superior vena cava. The postero-inferior<br />
rim is also identified as it joins the<br />
postero-inferior back wall of the left atrium.<br />
The fifth rim, the AS rim, is located just<br />
behind the ascending aorta and is identified<br />
from standard para-sternal short axis<br />
views as depicted in Figure 10. It should<br />
be remembered that roughly 45% of all<br />
secundum ASDs are located anteriorly and<br />
superiorly behind the aorta rather than<br />
centrally near the fossa ovalis (Figure 6).<br />
Trans-Esophageal<br />
Echocardiography-TEE<br />
In most children weighing 15 kg or more,<br />
a standard adult multi-plane probe may<br />
be safely inserted. For those weighing less<br />
than 15 kg, an 8 mm multi-plane pediatric<br />
probe is appropriate. The most important<br />
aspect of probe placement is pulling the<br />
lower mandible up and forward before the<br />
probe tip is inserted. The probe tip is then<br />
advanced to the level of the left atrium<br />
before proceeding. Ideally one should<br />
utilize a multi-plane probe which can rotate<br />
the beam from 0 degrees through +90<br />
degrees. Limiting rotation to 0 degrees to<br />
+90 degrees ensures constant right-left<br />
Figure 10. TTE parasternal short axis demonstrating<br />
the AS rim behind the ascending aorta.<br />
orientation. Rotating beyond 90 degrees<br />
will reverse right-left relationships. In order<br />
to see the left and right atrial disks after<br />
deployment together with the sandwiched<br />
rims in between, one must see the disks<br />
perpendicular to the delivery sheath. This<br />
requires the ability to see the sheath at<br />
roughly 40 degrees to 80 degrees, the<br />
angle at which the sheath enters the heart<br />
from the inferior vena cava. Figure 11 is an<br />
artist’s rendering of the delivery sheath and<br />
deployed left atrial disk within the heart.<br />
Note that the plane of the disk is not 90<br />
degrees to the plane of the sheath (Figure<br />
12). If a biplane probe is used, the sheath<br />
will not be visualized along its long axis<br />
obviating the ability to see the deployed<br />
disks perpendicular to the sheath and<br />
parallel to the enclosed septal rims.<br />
Step one is to identify the AI and PS rims.<br />
This is done by visualizing the heart from<br />
directly behind the left atrium at 0 degrees.<br />
A standard four chamber view is produced<br />
which orients the left heart structures to<br />
the observer’s right and the right sided<br />
structures on the observer’s left. This view<br />
cuts the heart from the posterior superior<br />
aspect where the right and left upper
pulmonary veins enter the left atrium to the<br />
apex of the ventricles which is anterior and<br />
inferior as the heart sits in the chest (Figures<br />
13 – 16). This view is analogous (although<br />
the antero-posterior reverse) to the standard<br />
trans-thoracic four chamber view.<br />
Figure 15 shows a pathology specimen with<br />
severe left ventricular hypertrophy with the<br />
heart cut at 0 degrees exactly along the<br />
same plane subtended by the TEE probe.<br />
The cut is from the posterior superior aspect<br />
of the left atrium near the entrance of the<br />
right upper pulmonary vein to the apex of<br />
the left ventricle anteriorly and inferiorly,<br />
hence the designation of the posterosuperior<br />
and antero-inferior rims of the<br />
atrial septum. Figure 17 shows absence of<br />
the PS rim. Such defects if larger than about<br />
2 cm require surgical closure. The largest<br />
GORE ® HELEX Septal Occluder available is<br />
too small to close defects of this size, and<br />
closure with other commercially available<br />
devices may not be suitable due to the risk<br />
of erosion through the posterior atrial wall<br />
from an obligatorily oversized device.<br />
Step two is to identify the S and PI rims.<br />
Figure 18 shows that a vertically oriented<br />
plane will cut through both rims. By rotating<br />
the probe to roughly +90 degrees (Figure<br />
19), a plane will be created that will cut<br />
through the superior vena cava, right<br />
atrium, and inferior vena cava. This<br />
SVC<br />
PS<br />
IVC<br />
PI<br />
S<br />
AS<br />
AI<br />
AAO<br />
Figure 13. 0 degrees plane of the probe cuts the<br />
PS and AI rims.<br />
view is analogous to the trans-thoracic<br />
sub-coastal long axis view. Figure 19 (inset)<br />
shows the probe oriented in this fashion.<br />
By limiting rotation to +90 degrees, one will<br />
obligatorily orient the superior vena cava to<br />
the right with the inferior vena cava to the<br />
left (Figures 19, 20). This 90 degree view is<br />
the most important of all views because it is<br />
the only way to visualize the postero-inferior<br />
rim. Figure 21 demonstrates absence of<br />
the postero-inferior rim which results in an<br />
Postero-superior<br />
Atrial Septal Rim<br />
Antero-inferior<br />
Atrial Rim<br />
Figure 16. Standard four chamber view at 0<br />
degrees.<br />
LA<br />
Figure 11. Left atrial disk deployed. The angle of<br />
entrance of the sheath into the RA lies between<br />
40 degrees and 80 degrees.<br />
RA<br />
RV<br />
LV<br />
Figure 17. Absent PS rim. Blue color represents<br />
blood flow from LA to RA across ASD.<br />
70˚<br />
Figure 12. Note plane of atrial septum (yellow<br />
arrow) compared to probe angle of 70 degrees<br />
which shows the long axis of the sheath (green)<br />
with the LA disk perpendicular to the sheath.<br />
D<br />
Figure 14. At 0 degrees, a four chamber view is<br />
obtained.<br />
Entrance of Right<br />
Upper Pulmonary Vein<br />
RA<br />
Postero-superior<br />
Atrial Septal Rim<br />
LA<br />
Antero-inferior<br />
Atrial Rim<br />
Figure 15. Pathology specimen cut at 0 degrees.<br />
SVC<br />
PS<br />
IVC<br />
PI<br />
S<br />
AS<br />
AI<br />
AAO<br />
Figure 18. Vertical orientation of probe plane to<br />
intercept the superior and postero-inferior rims.
A<br />
Posterior-inferior<br />
Rim<br />
Superior Rim<br />
Posterior-inferior<br />
Rim<br />
Superior LA Rim RPA<br />
LA<br />
IVC<br />
RPA<br />
SVC<br />
IVC<br />
RA<br />
SVC<br />
A<br />
RA<br />
Figure 19. Probe at roughly +90 degrees cuts the<br />
RA vertically through the SVC, RA, and IVC.<br />
Antero-superior<br />
Rim<br />
Antero-superior LA<br />
Rim<br />
RA<br />
B<br />
RA<br />
B<br />
RVOT<br />
LA<br />
AoV<br />
RVOT<br />
AoV<br />
Tricuspid<br />
Valve<br />
Aortic<br />
Valve<br />
Absent<br />
AS Rim<br />
Figure 24. Probe at 15 degrees showing absent<br />
AS rim.<br />
Tricuspid<br />
Valve<br />
Absent PI Rim<br />
S Rim<br />
Aortic<br />
Valve<br />
Superior Rim<br />
Absent<br />
RPA<br />
AS Rim<br />
Postero-inferior Rim<br />
SVC<br />
Figure 20. At 81 degrees with SVC to right, IVC to left.<br />
Figure 21. Absent PI rim with huge 3 cm diameter ASD.<br />
inferior sinus venosus ASD which cannot be<br />
closed with any device now available. Such<br />
defects often include absence of portions of<br />
the postero-superior rim near the entrance<br />
of the right upper pulmonary vein into the<br />
left atrium as well as the antero-superior<br />
rim behind the aorta. These ASDs often<br />
exceed 2.5 cm in diameter. If one looks<br />
only in the horizontal plane, the ASD may<br />
appear deceptively central in location with<br />
Figure 22. Probe at 15 degrees to see antero-superior<br />
rim AoV: aortic valve; RA: right atrium; RVOT:<br />
right ventricular Absent PI Rim outflow tract; LA; left atrium.<br />
S Rim<br />
Present<br />
AS Rim<br />
Aortic<br />
Valve<br />
Tricuspid<br />
Valve<br />
Figure 23. AS rim present.<br />
a diameter that may appear ideal for GORE ®<br />
HELEX Septal Occluder closure. But like an<br />
iceberg, the bulk of the opening is below the<br />
four chamber plane, and deployment and<br />
subsequent release of a device may lead<br />
to embolization. The last step is to identify<br />
the AS rim behind the aorta by rotating the<br />
probe to +15 degrees to 65 degrees which<br />
orients the beam parallel to the aortic valve.<br />
Figure 22 displays the probe orientation<br />
and the resultant artist’s rendering of the<br />
view obtained. One notes that this image is<br />
analogous to the trans-thoracic para-sternal<br />
short axis view. Figure 23 shows a centrally<br />
located ASD with present AS rim. Figure 24,<br />
in contrast, shows a more typical secundum<br />
ASD with complete absence of the AS rim.<br />
Is Rim Documentation Necessary?<br />
Why is it necessary to identify and measure<br />
all five rims before attempting to insert and<br />
release the GORE ® HELEX Septal Occluder?<br />
If adequate rim is present completely<br />
surrounding the ASD and provided the<br />
diameter is less than 18 mm, the opening<br />
can almost always be closed using the<br />
GORE ® HELEX Septal Occluder. Absence<br />
of the superior rim results in a high sinus<br />
venosus ASD which is commonly associated<br />
with partial anomalous pulmonary venous<br />
connection of the right upper and / or<br />
middle pulmonary veins to the superior<br />
vena cava. Obviously, such holes require a<br />
surgical approach. If the AS rim is absent,<br />
the hole can still be closed provided the<br />
other four rims are present. The device<br />
is sized and positioned such that the AS<br />
portions of the right and left atrial disks hug<br />
the posterior wall of the ascending aorta<br />
as if one is surrounding a tree trunk with<br />
one’s arms. Absence of the AI rim results in<br />
a form of endocardial cushion defect known<br />
as an ostium primum ASD. Since the hole<br />
is located immediately above the AV valves<br />
with no intervening tissue, a deployed<br />
device will obligatorily be in contact with<br />
AV valve tissue. Closure with any available<br />
device is currently not possible. Holes in the<br />
region inferiorly between the AI and PI rims<br />
are termed coronary sinus ASDs and are<br />
not closeable using interventional devices.<br />
Absence of the postero-inferior rim results in<br />
an inferior type sinus venosus atrial septal<br />
defect. As noted, such openings are often<br />
very large sometimes exceeding 3 cm in<br />
diameter and require surgery to safely close.<br />
Absence of the postero-superior rim alone<br />
is problematic. If the diameter of the hole<br />
is less than about 16 – 20 mm, the hole<br />
may be closeable. Larger diameter holes<br />
are not closeable with the GORE ® HELEX<br />
Septal Occluder. Holes that are more or less<br />
centrally located or positioned anteriorly<br />
and superiorly behind the aorta with<br />
adequate surrounding rims are best suited<br />
to be closed safely with the GORE ® HELEX<br />
Septal Occluder.
F E A T U R E D T O P I C<br />
Creating Products through Collaborative Innovation<br />
Collaboration Leads to Innovation<br />
When business strategist Dan Burrus visited<br />
<strong>Gore</strong> to speak at an innovation conference<br />
in 2008, he noticed something unique about<br />
the way the company interacts with its<br />
customers. As <strong>Gore</strong> product specialist Bob<br />
Sassa recalls, “He referred to <strong>Gore</strong> as the<br />
‘master of collaborative innovation,’ because<br />
we like to work closely with customers to<br />
develop products that meet their needs.”<br />
To do this effectively, associates often ask<br />
customers numerous questions, play an<br />
active role in problem-solving and even<br />
work alongside them in their facilities. Dan<br />
pointed out that few companies collaborate<br />
so openly, and some customers might not<br />
understand or feel comfortable with this<br />
unique approach. His feedback spurred Bob<br />
and a team of fellow associates to create<br />
videos highlighting <strong>Gore</strong>’s collaborative<br />
innovation process. “A collaborative<br />
relationship requires a lot of trust from<br />
each party,” says <strong>Gore</strong> project core team<br />
member Betty Snyder. “We wanted to<br />
create something that would help new and<br />
prospective customers understand why we<br />
work this way.” The videos, filmed by <strong>Gore</strong><br />
“<br />
Associate Curtis King highlight real life<br />
examples of <strong>Gore</strong>’s work with customers on<br />
new product innovation.<br />
Examples include:<br />
• Creation of a fiber that increases the<br />
service life of ropes in high-stress<br />
applications<br />
• Enhancement of an implantable<br />
medical material used in hernia repair<br />
• Development of a fabric and ensemble<br />
that protects against chemicals and<br />
biological agents<br />
• Creation of a material that reduces<br />
the heat generated by thin notebook<br />
computer processors<br />
• Development of a filter that captures<br />
particulate matter and destroys toxic<br />
dioxins and furans<br />
Customer Collaboration<br />
Each story features the customers’ and<br />
associates’ perspectives of their experiences<br />
working together. “These videos show that<br />
we’re way more than simply a provider of<br />
products,” Curtis says. “We work hard to<br />
understand the technical issues that are<br />
keeping our customers up at night. Our<br />
philosophy is to be the problem solver.” <strong>Gore</strong><br />
project core team member Gordon McGregor<br />
says it’s helpful to receive feedback from<br />
customers on <strong>Gore</strong>’s approach. Customers<br />
express many common viewpoints in the<br />
videos, including the level of trust they<br />
place in the company and how much they’ve<br />
benefited from their close collaboration<br />
with <strong>Gore</strong>. Comments included: “<strong>Gore</strong> is a<br />
company that will allow you to get to your<br />
goal,” and “I would [work with <strong>Gore</strong>] again in<br />
a heartbeat.” “They talked from the heart,”<br />
Gordon says of the customers. “It feels good<br />
to see that we’re delivering on the things<br />
they’re looking for, and that we’re really<br />
adding value to their products. They all said<br />
they had a great experience with us, and<br />
that’s exactly what we’re trying to deliver.”<br />
Note: Ask your local <strong>Gore</strong> Sales Associate for the<br />
full collaborative innovation DVD. Video files are<br />
available in our online version of Closing Remarks:<br />
http://www.goremedical.com/helex/library/<br />
newsletters<br />
We work hard to understand the technical issues that are keeping our customers up<br />
at night. Our philosophy is to be the problem solver. — Curtis King<br />
”<br />
The image above features the GORE ® BIO-A ® Tissue Reinforcement collaborative video. The DVD includes five-minute Collaborative Innovation video segments<br />
spotlighting examples of <strong>Gore</strong>’s work with customers on new product innovation. The segments include GORE OMNIBEND Fiber, GORE ® BIO-A ® Tissue Reinforcement,<br />
GORE ® CHEMPAK ® Fabric, GORE Thermal Interface Material and GORE ® REMEDIA ® Catalytic Filtration Systems.
I N T H E N E W S<br />
<strong>Gore</strong> Provides Update on <strong>Gore</strong> REDUCE Clinical Study<br />
for Patent Foramen Ovale (PFO) Closure<br />
The <strong>Gore</strong> REDUCE Clinical Study* is a prospective, randomized, multi-center, multinational<br />
trial designed to demonstrate safety and effectiveness of the GORE ® HELEX Septal<br />
Occluder for Patent Foramen Ovale (PFO) closure in patients with history of cryptogenic<br />
stroke or imaging-confirmed Transient Ischemic Attack (TIA). The unique study, which<br />
includes up to 50 investigational sites in the US and in Europe, is estimated to meet its<br />
completion in 2014.<br />
“In light of the recent press release regarding the preliminary results of CLOSURE I, we<br />
felt it important to re-emphasize our confidence in the design and expected outcome<br />
of the <strong>Gore</strong> REDUCE Clinical Study,” said Stuart Broyles, PhD, Associate with the <strong>Gore</strong><br />
<strong>Medical</strong> Division Stroke Business. “Due to our European experience regarding the clinical<br />
performance of the GORE ® HELEX Septal Occluder and our unique study design, we remain<br />
very confident that the <strong>Gore</strong> REDUCE Clinical Study will ultimately achieve its intended<br />
objective. We are committed to the completion of this study and the pursuit of an FDA<br />
indication for PFO closure and the prevention of recurrent stroke.”<br />
According to Scott Kasner, MD, Professor of Neurology and Director of the Comprehensive<br />
Stroke Center at the University of Pennsylvania <strong>Medical</strong> Center, and US Neurology<br />
Principal Investigator, “The design of the <strong>Gore</strong> REDUCE Clinical Study is unique from the<br />
other PFO stroke trials in several respects. First, Magnetic Resonance Imaging (MRI) of the<br />
brain will be performed on all patients at baseline and at two years. This feature offers<br />
an additional imaging endpoint for making comparisons between the treatment arms.<br />
Second, it focuses on secondary prevention of stroke rather than TIA, which improves the<br />
reliability of the study outcomes and measurably impacts the public health. Finally, this<br />
is a multinational study, which enhances its global applicability. These efforts will likely<br />
help resolve the open debate about whether PFO closure is a viable option for treating<br />
cryptogenic stroke / TIA patients as compared to medical treatment<br />
alone, as it is used today.”<br />
The <strong>Gore</strong> REDUCE Clinical Study has several unique features: participation of Nordic<br />
investigational sites, the use of imaging-confirmed stroke / TIA for assessing its primary<br />
endpoint, a 2:1 device to medical management randomization strategy, a standardization<br />
of medical therapies across treatment arms, and the use of the GORE ® HELEX Septal<br />
Occluder. Recruitment in the Nordic countries, where patients may be more willing to<br />
be randomized, is projected to help drive study enrollment. Additionally, <strong>Gore</strong> is in the<br />
process of recruiting sites in the United Kingdom to participate in the <strong>Gore</strong> REDUCE<br />
Clinical Study. MRI will be used to evaluate all patients in the trial to more accurately<br />
confirm the presence of stroke and TIA. Additionally, the standardization of medical<br />
therapies across treatment arms will further aid the interpretation of the final results in<br />
assessing the potential benefit of device closure for the prevention of recurrent stroke.<br />
The GORE ® HELEX Septal Occluder was approved by the US Food and Drug Administration<br />
(FDA) in 2006 for treatment of Atrial Septal Defect (ASD), a congenital heart defect. The<br />
GORE ® HELEX Septal Occluder is the first device of its kind to use ePTFE, a biocompatible<br />
material that allows progressive tissue ingrowth, to help seal the defect.<br />
*REDUCE: GORE ® HELEX Septal Occluder plus Anti-platelet <strong>Medical</strong> Management for<br />
Reduction of Recurrent Stroke or Imaging-Confirmed TIA in Patients with PFO.<br />
Visit http://www.clinicaltrials.gov for more information.<br />
“<br />
We are committed to<br />
the completion of this<br />
study and the pursuit<br />
of an FDA indication for<br />
PFO closure and the<br />
prevention of recurrent<br />
stroke.<br />
”<br />
— Stuart Boyles, PhD<br />
Caution: Investigational Device. Limited by United States Law to Investigational Use For the Indication described in this article.
U P C O M I N G E V E N T S<br />
Please Join Us...<br />
SCAI Fall Fellows Program<br />
<strong>Gore</strong> Structural Heart Disease and Stroke Symposium<br />
December 5 – 6<br />
Las Vegas, Nevada<br />
2010 Scheduled GORE MEDICAL MASTERY SERIES Courses Sponsored by <strong>Gore</strong><br />
October 13 – 14 Chicago Atrial Septal Defect Closure Course with a Lab<br />
October 21 – 22* Philadelphia Atrial Septal Defect Closure Course with a Lab<br />
October 28 – 29 San Diego Introduction Atrial Septal Defect Closure<br />
December 3* Detroit Complex Atrial Septal Defect Closure<br />
<strong>Gore</strong>’s commitment to excellence continues with the GORE MEDICAL MASTERY SERIES.<br />
The Atrial Septal Defect Closure courses provide Interventional Cardiologists with the<br />
opportunity to develop their knowledge of implant techniques. Contact your local <strong>Gore</strong><br />
Sales Associate for further information regarding these various course opportunities.<br />
* enrollment full<br />
If you have a topic that you would like us to consider in a future issue of Closing Remarks,<br />
please contact your local <strong>Gore</strong> Sales Associate or e-mail ClosingRemarks@wlgore.com<br />
W. L. <strong>Gore</strong> & Associates, Inc.<br />
Flagstaff, AZ 86004<br />
+65.67332882 (Asia Pacific) 800.437.8181 (United States)<br />
00800.6334.4673 (Europe) 928.779.2771 (United States)<br />
goremedical.com<br />
INDICATIONS FOR USE IN THE US: The GORE HELEX Septal Occluder is a permanently implanted prosthesis indicated for the percutaneous, transcatheter<br />
closure of ostium secundum atrial septal defects (ASDs). INDICATIONS FOR USE UNDER CE MARK: The GORE HELEX Septal Occluder is a permanently<br />
implanted prosthesis indicated for the percutaneous, transcatheter closure of atrial septal defects (ASDs), such as ostium secundum and patent foramen<br />
ovale. Refer to Instructions for Use at goremedical.com for a complete description of all contraindications, warnings, precautions and adverse events.<br />
Products listed may not be available in all markets.<br />
GORE ® , BIO-A ® , CHEMPACK ® , HELEX, OMNIBEND, PERFORMANCE BY DESIGN, REMEDIA ® , and designs are trademarks of W. L. <strong>Gore</strong> & Associates.<br />
© 2010 W. L. <strong>Gore</strong> & Associates, Inc. AP4476-EN1 AUGUST 2010