Printable PDF Version - Gore Medical
Printable PDF Version - Gore Medical
Printable PDF Version - Gore Medical
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
Closing Rem a rk s<br />
In This<br />
I S S U E<br />
• C A S E S T U D Y<br />
Intracardiac Echocardiography<br />
Considerations During<br />
Implantation of the<br />
GORE ® HELEX Septal Occluderr<br />
• F E A T U R E D T O P I C<br />
New, More User-Friendly <strong>Medical</strong><br />
Website Launches:<br />
goremedical.com<br />
P E R F O R M A N C E b y d e s i g n<br />
• I N T H E N E W S<br />
<strong>Gore</strong> REDUCE Clinical Study<br />
Steering Committee Responds<br />
to CLOSURE I Data<br />
• U P C O M I N G E V E N T S<br />
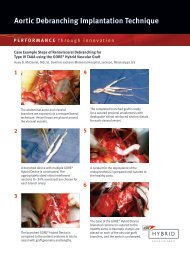
C A S E S T U D Y<br />
Intracardiac Echocardiography<br />
Considerations During Implantation<br />
of the GORE ® HELEX Septal Occluder<br />
Mark H. Hoyer, MD<br />
Professor of Clinical Pediatrics, Section of Pediatric Cardiology,<br />
Director of Cardiac Catheterization and Interventional Cardiology,<br />
Riley Hospital for Children, Indiana University School of Medicine<br />
In the previous issue of Closing Remarks, a detailed discussion of atrial<br />
septal anatomy was presented, followed by imaging techniques necessary<br />
to fully assess atrial septal defect (ASD) size and rims. Transthoracic and<br />
transesophageal echocardiography were the highlighted imaging modalities.<br />
In this issue, a recent ASD closure procedure is shared to illustrate the use of<br />
intracardiac echocardiography (ICE) for initial anatomic evaluation and for<br />
guiding closure of the defect with a GORE ® HELEX Septal Occluder.<br />
Continued on inside cover...<br />
Winter 2010 • Issue XII
Intracardiac Echocardiography Considerations During<br />
Implantation of the GORE ® HELEX Septal Occluder<br />
Continued from cover...<br />
An eight-year-old girl presented for<br />
transcatheter ASD closure at a weight<br />
of 24.6 kg. A prior transthoracic<br />
echo showed a defect diameter<br />
of approximately 10 mm, and the<br />
posterosuperior (SVC), anterosuperior<br />
(aortic), anteroinferior (tricuspid<br />
valve), posteroinferior (IVC), and<br />
posterosuperior (pulmonary<br />
vein) rims were all adequate.<br />
Using general anesthesia and<br />
heparin anticoagulation, cardiac<br />
catheterization revealed normal right<br />
heart pressures and a Q p<br />
/ Q s<br />
of 1.3.<br />
ICE imaging was performed using an<br />
8F ACUNAV Intracardiac Echo Catheter<br />
through a contralateral venous sheath.<br />
As part of the usual imaging protocol,<br />
a complete ICE evaluation was<br />
completed as follows:<br />
Note: Any control knob adjustments<br />
of the ICE catheter are best made by<br />
moving the locking ring clockwise<br />
to the locked position first and then<br />
moving the A / P or L / R control knob<br />
as needed, thereby maintaining their<br />
position.<br />
1. “Home” view (Figure 1): the ICE<br />
catheter arrow indicator at the control<br />
end corresponds to the transducer<br />
orientation at the catheter tip, and<br />
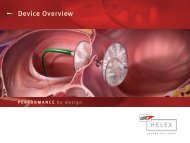
Right Atrial Disk<br />
Left Atrial Disk<br />
Figure 2 Implanted GORE ® HELEX Septal Occluder<br />
in hypothetical heart model.<br />
this should be oriented toward patient<br />
left and slightly anterior; the tricuspid<br />
valve is seen with the right atrium<br />
above and the right ventricle below;<br />
superior is screen right, and inferior is<br />
screen left; occasionally adjusting the<br />
control knob slightly to the Anterior<br />
(A) location is necessary.<br />
2. Using both hands (right hand<br />
at control knob area, left hand on<br />
catheter near introducer sheath entry),<br />
the catheter is rotated clockwise (when<br />
looking from patient’s feet to head) or<br />
away from operator; during this slow<br />
rotation, one may see a prominent<br />
Eustachian valve or Chiari network,<br />
but typically the coronary sinus starts<br />
“rounding” out, and subsequently<br />
the LV and RV outflow tracts are<br />
seen; variations in cardiac anatomy<br />
and position often require gentle<br />
adjustment of the L / R control knob to<br />
optimize the image.<br />
3. With further clockwise rotation,<br />
the mitral valve, left atrial appendage,<br />
and a fully round cross-section of the<br />
coronary sinus are visible (Figures 2<br />
and 3); the atrial septum is well seen;<br />
as clockwise rotation continues,<br />
the left-sided pulmonary veins are<br />
typically seen as an upside down<br />
“Y” connection, with the left superior<br />
vein to screen right and the left<br />
inferior vein to screen left; color flow<br />
is red / orange as the direction of flow<br />
is toward the transducer, which is<br />
situated in the right atrium (Figure 4).<br />
4. As one continues a clockwise<br />
rotation around the back of the heart,<br />
the descending aorta is seen next in<br />
a horizontal orientation.<br />
5. Just to patient right of the<br />
descending aorta are the right-sided<br />
pulmonary veins, again found by<br />
clockwise rotation beyond the<br />
descending aorta. Without any<br />
control knob adjustment, these most<br />
commonly appear as a foreshortened<br />
upside down “Y” connection;<br />
significantly enhanced imaging of the<br />
right-sided veins can be achieved by<br />
locking the L / R control knob toward<br />
Figure 1. Home view.<br />
Figure 3. View of the left atrial appendage<br />
and mitral valve. The atrial is also well seen.<br />
Figure 4. Left superior and inferior pulmonary<br />
veins.
Figure 5. Right middle and lower pulmonary<br />
veins.<br />
“L” (toward operator). This corresponds<br />
to left when looking up from patient’s<br />
feet to head, but counterintuitively is<br />
patient right; then rotate the entire<br />
ICE catheter slightly clockwise or<br />
counterclockwise to obtain images of<br />
the elongated right-sided pulmonary<br />
veins; this usually shows the right<br />
middle (screen right) and right lower<br />
(screen left) pulmonary veins joining<br />
(Figure 5); to image the right upper<br />
pulmonary vein, one then minimally<br />
advances the entire ICE catheter inward<br />
(superiorly) while gently rotating<br />
clockwise even more, and the vein<br />
comes into view farther right on the<br />
screen (more superior).<br />
6. After carefully assessing the<br />
underlying anatomy, attention is<br />
then turned to the atrial septum; the<br />
Figure 7. Balloon sizing with measurement<br />
marked by crosshairs.<br />
coronary sinus and posteroinferior<br />
rim has already been seen during the<br />
initial clockwise sweep, but can be<br />
viewed again.<br />
7. From “Home” view, the control<br />
knob is locked in a posterior position<br />
and the entire catheter is rotated<br />
clockwise, revealing the atrial<br />
septum and ASD; this is ideal for the<br />
anterosuperior (aortic) rim, opposite<br />
of which is the posteroinferior or<br />
posterosuperior rim (Figure 6).<br />
8. From this view, adjusting the<br />
locked control knob toward “R”<br />
(clockwise toward patient left), the<br />
ASD is often more optimally imaged,<br />
and minor adjustments of this knob<br />
clockwise or counterclockwise may<br />
be necessary; with more pronounced<br />
clockwise rotation (away from<br />
Figure 9. ICE appearance before freeing<br />
Eustachian valve.<br />
operator), a bicaval view is often<br />
seen, allowing measurements of the<br />
caval rims.<br />
9. Therefore, with ICE, measurements<br />
of the five important rims (superior,<br />
anterosuperior, anteroinferior,<br />
posteroinferior, and posterosuperior)<br />
can usually be obtained; however, it<br />
may be necessary to visualize these<br />
rims during control knob “sweeps,”<br />
with the desired images being<br />
somewhat in between.<br />
In our case illustration, the baseline<br />
measurement of the defect was 9.5 mm,<br />
while the rim measurements<br />
were as follows: superior 13 mm,<br />
anterosuperior 7 mm, anteroinferior > 20<br />
mm, posteroinferior 10 mm, and<br />
posterosuperior 10.9 mm.<br />
Figure 6. ASD with anterosuperior and<br />
posterior rims.<br />
Figure 8. Eustachian valve is caught within<br />
the GORE ® HELEX Device discs.<br />
Figure 10. ICE appearance after Eustachian<br />
valve freed from device.
Figure 11. RA angiogram provides considerable<br />
information about device position and<br />
freedom from surrounding structures.<br />
Using a balloon sizing catheter over<br />
an extra stiff exchange wire and color<br />
stop-flow technique, the defect was<br />
sized at 13.5-14 mm (Figure 7).<br />
A 30 mm GORE ® HELEX Septal Occluder<br />
(device : defect diameter ratio = 2.2)<br />
was implanted by standard techniques,<br />
and follow-up ICE imaging showed the<br />
inferior portion of the right atrial disc<br />
to be slightly separated from the atrial<br />
septum. It actually appeared caught on<br />
the Eustachian valve (Figure 8), so a<br />
5F multipurpose catheter was used to<br />
gently push on the right atrial side of<br />
the disc, freeing up the disc from the<br />
Eustachian valve. Consequently, the<br />
device had a flatter profile (Figures 9<br />
and 10, before and after).<br />
A right atrial angiogram was performed<br />
by hand through the long delivery<br />
sheath, showing the contrast<br />
enveloping the right atrial disc, as well<br />
as reflux of contrast into the SVC and<br />
coronary sinus (Figure 11).<br />
This provided reassurance that the<br />
device does not impede important flow<br />
within the heart.<br />
Intracardiac echocardiography provides<br />
detailed images of the heart, especially<br />
the atrial septum. The ability to<br />
clearly see the posteroinferior rims<br />
of an ASD provides an advantage<br />
over transesophageal echo, which<br />
often results in suboptimal near-field<br />
imaging. In addition, the use of ICE<br />
precludes the need for endotracheal<br />
intubation in older patients or adults,<br />
thereby simplifying the procedure.<br />
Please refer to GORE ® HELEX Septal Occluder<br />
Instructions for Use at goremedical.com for<br />
a complete description of all indications,<br />
contraindications, warnings, precautions and<br />
adverse events.
F E A T U R E D T O P I C<br />
New, More User-Friendly <strong>Medical</strong> Website Launches:<br />
goremedical.com<br />
<strong>Gore</strong> Sales Associate, Alvaro De La<br />
Mora, knew just what to do when one<br />
of his customers — an interventional<br />
cardiologist — requested product<br />
animation for use at an upcoming<br />
seminar.<br />
“I referred him to goremedical.com,”<br />
Alvaro says. “I knew he’d be able to<br />
quickly and easily get what he needed,<br />
and now he can share that animation<br />
with fellow physicians.”<br />
Those physicians can also use the<br />
website to learn more about <strong>Gore</strong> medical<br />
technologies. The recently redesigned<br />
site makes it easy to find such content<br />
as newsletters, brochures, instructional<br />
videos and frequently asked questions,<br />
among additional resources.<br />
Meeting Diverse Needs<br />
The impact of goremedical.com is<br />
far reaching. And after undergoing a<br />
redesign, the site is being touted as more<br />
attractive, brand reflective and userfriendly.<br />
It contains much of the same<br />
content as the previous goremedical.<br />
com, but in a new format.<br />
“We wanted to make it easy for website<br />
visitors to access what they’re looking<br />
for,” says <strong>Medical</strong> Products Division<br />
marketing associate and project<br />
co-champion Matt Markiewicz. “Our old<br />
site generated fairly positive feedback,<br />
but it had so much information that it<br />
was starting to become cluttered. The<br />
new site is more polished. We worked to<br />
minimize the number of clicks it takes<br />
for visitors to get to the information<br />
they need.”<br />
Matt says the project team analyzed<br />
the latest web design research to create<br />
a site that would satisfy visitors. “We<br />
wanted to know — when people look at a<br />
website, what do they look at first? How<br />
do they read the information? We took all<br />
of this into account to make the site more<br />
visually appealing.”<br />
The content is accessible through four<br />
categories of links — products, conditions,<br />
specialties and resources — increasing<br />
the likelihood that visitors will find what<br />
they need. “A doctor might be more likely<br />
to click on a product name, whereas a<br />
patient might be more likely to click on a<br />
condition name,” Matt says. “Because the<br />
website has so many different types of<br />
visitors, we provided them with different<br />
ways to access information.”<br />
Once visitors find what they’re looking<br />
for, the website’s search engine provides<br />
links to related terms, making it simple<br />
for visitors to find more information<br />
relevant to their profession, diagnosis<br />
or procedure.<br />
Continued on next page...
New, More User-Friendly <strong>Medical</strong> Website Launches:<br />
goremedical.com<br />
Continued from previous page...<br />
Yielding Positive Feedback<br />
“When information is hard to find, your<br />
biggest concern is that people will leave<br />
the site frustrated,” Matt says. “Our<br />
metrics indicate that with the new site,<br />
people are having more success finding<br />
what they need.”<br />
Customers have also provided positive<br />
feedback. Alvaro, for example, recounts<br />
an interaction with another doctor who<br />
recently used the site: “He came to me<br />
and thanked our company for offering<br />
such a user-friendly, well thought-out<br />
site. He had a patient in his office<br />
who wanted more information about<br />
one of our products, and by visiting<br />
goremedical.com, he quickly found<br />
what he needed.”<br />
In this age of information technology,<br />
Alvaro says a growing number of<br />
doctors and patients turn to the Internet<br />
to learn more about the medical<br />
devices they’re using or receiving.<br />
“<strong>Gore</strong>medical.com allows them to get<br />
their questions answered,” he says.<br />
“And it really lays the information out<br />
for them in a nice, user-friendly format.”<br />
Creating a Consistent Brand Voice<br />
The new site does more than answer<br />
doctor and patient questions. It also<br />
leverages the power of the <strong>Gore</strong> brand.<br />
The site shares a similar look and feel<br />
with gore.com, including a banner that<br />
incorporates brand color and imagery.<br />
The banner also features animation and<br />
an area that highlights new products,<br />
events and other important information.<br />
And, like gore.com, the site features a<br />
navigation bar above the banner and<br />
four columns of links below.<br />
And the consistent branding reminds<br />
visitors that <strong>Gore</strong>’s diverse medical<br />
products come from the same company—<br />
one with a long history of innovation and<br />
integrity. “We want them to know that<br />
these products are made by <strong>Gore</strong> and<br />
backed by <strong>Gore</strong>,” Matt says. “We have<br />
set the bar really high in the medical<br />
community. It’s important that whether<br />
you’re looking for a hernia patch or an<br />
endovascular graft that you know the<br />
product is from <strong>Gore</strong>, and you can trust it<br />
because it comes from <strong>Gore</strong>.”<br />
View the new site design at:<br />
goremedical.com and<br />
goremedical.com/HELEX
I N T H E N E W S<br />
<strong>Gore</strong> REDUCE Clinical Study Steering Committee Clarify the Current Status<br />
of CLOSURE I Data<br />
The <strong>Gore</strong> REDUCE Clinical Study Principal<br />
Investigators have prepared the following<br />
statement on behalf of the <strong>Gore</strong> REDUCE<br />
Clinical Study Steering Committee in<br />
response to the recent CLOSURE I results:<br />
The <strong>Gore</strong> REDUCE Clinical Study is a<br />
prospective, randomized, multi-center,<br />
multi-national trial designed to<br />
demonstrate safety and effectiveness<br />
of the GORE ® HELEX Septal Occluder for<br />
PFO closure in patients with history of<br />
cryptogenic stroke or imaging-confirmed<br />
Transient Ischemic Attack (TIA). The<br />
unique study, which includes up to fifty<br />
investigational sites in the US and Europe,<br />
is on track. More information visit,<br />
clinical.goremedical.com/REDUCE.<br />
“On November 15, 2010 at the American<br />
Heart Association (AHA) annual meeting<br />
in Chicago, Anthony Furlan, MD presented<br />
the results of CLOSURE I, a prospective,<br />
multi-center, randomized controlled trial<br />
of PFO closure with the STARFLEX ® Device<br />
(NMT <strong>Medical</strong>, Inc) versus best medical<br />
therapy for the prevention of recurrent<br />
stroke and/or transient ischemic attack<br />
(TIA) in patients with cryptogenic stroke /<br />
TIA and PFO. The results of the study,<br />
as presented, showed no statistically<br />
significant difference between device<br />
closure and best medical therapy. In a<br />
discussant presentation, Pierre Amarenco,<br />
MD concluded that PFO closure is not<br />
needed for the majority of patients<br />
with stroke and PFO and should not be<br />
performed in routine practice. However,<br />
he noted that many patients with stroke<br />
and PFO have alternative (non-PFO)<br />
causes for their strokes, and argued<br />
that this may have diluted a true causal<br />
effect of PFO in the CLOSURE I study.<br />
Dr. Amarenco left open the possibility that<br />
PFO closure may still be considered in<br />
patients with truly cryptogenic stroke.<br />
This presentation and the recommendations<br />
discussed would appear to refute<br />
the innovative device approach to the<br />
prevention of recurrent cryptogenic stroke<br />
in patients with PFO. However, there are<br />
several key issues that we believe should<br />
limit the impact of the CLOSURE I results<br />
on the ongoing <strong>Gore</strong> REDUCE Clinical<br />
Study. These issues are mostly related to<br />
device and patient selection:<br />
• CLOSURE I included patients with<br />
clinically-defined (not imaging-confirmed)<br />
TIAs. Recent studies have shown that<br />
MRI-negative TIAs are associated with an<br />
extremely low risk of subsequent stroke.<br />
Inclusion of such patients likely resulted<br />
in an underestimation of stroke event<br />
rates in both arms of the trial as compared<br />
to a population with strokes confirmed<br />
by imaging.<br />
• The majority of the stroke endpoint<br />
events during follow-up appeared to<br />
have a determinable origin, suggesting<br />
that these patients likely had alternative<br />
explanations for their index stroke. Stroke<br />
due to atherosclerosis or small vessel<br />
disease would not be affected by PFO<br />
closure, and therefore would bias the<br />
results toward underestimating a potential<br />
treatment effect for PFO closure (i.e., bias<br />
towards the null).<br />
• Nearly half of the stroke endpoint<br />
events in the PFO closure arm appeared<br />
to be directly related to the device itself,<br />
and about a quarter of these occurred<br />
in the first 30 days after implantation.<br />
Alternative devices (like the GORE ® HELEX<br />
Septal Occluder) may offer substantial<br />
advantages and fewer complications,<br />
thereby increasing the differences<br />
between device and medical therapy.<br />
• Although device-related complications<br />
were considered insignificant, the<br />
incidence of new atrial fibrillation (5.7%)<br />
and device thrombus (four cases and two<br />
cases lead to a subsequent stroke) appear<br />
to be associated with recurrent events<br />
and more frequent when compared to the<br />
GORE ® HELEX Septal Occluder reports.<br />
• <strong>Medical</strong> therapy differed between<br />
PFO closure and control arm, thereby<br />
introducing a confounding effect on the<br />
study endpoints.<br />
We, the <strong>Gore</strong> REDUCE Clinical Study<br />
Principal Investigators, conclude that<br />
improved patient selection focused on<br />
truly cryptogenic strokes (rather than<br />
other causes of stroke or TIA) and use of<br />
a device with a low complication rate is<br />
needed to determine whether PFO closure<br />
is superior to best medical therapy.<br />
The <strong>Gore</strong> REDUCE Clinical Study addresses<br />
the CLOSURE I limitations by design:<br />
• All TIAs must be confirmed by<br />
neuroimaging studies, which will prevent<br />
the inclusion of spurious neurological<br />
events that are not vascular in origin.<br />
• Eligibility criteria are more stringent<br />
and better exclude patients with<br />
non-cryptogenic strokes, such as the<br />
exclusion of lacunar strokes and exclusion<br />
of patients with a substantial burden of<br />
vascular risk factors.<br />
• Both test and control arms for the study<br />
have the same medical therapy and sites<br />
are directed to apply a uniform medical<br />
therapy regimen for both test and control<br />
subjects.<br />
• The clinical literature for the GORE ®<br />
HELEX Septal Occluder supports a low rate<br />
of device related atrial fibrillation and a<br />
nearly non-existent incidence of device<br />
thrombus formation.<br />
With additional PFO trials still underway,<br />
much remains to be determined regarding<br />
the best course of therapy for cryptogenic<br />
stroke patients with PFO. Taking into<br />
consideration the <strong>Gore</strong> REDUCE Clinical<br />
Study design and the noted shortcomings<br />
of the CLOSURE I study, the <strong>Gore</strong> REDUCE<br />
Clinical Study Steering Committee has<br />
concluded that the best course of action is<br />
to continue the study without significant<br />
changes. Additionally, in June, the FDA<br />
also recommended that the <strong>Gore</strong> REDUCE<br />
Clinical Study continue as original planned.<br />
At this point in time there is no compelling<br />
reason to alter the current clinical study.<br />
It remains imperative, as it has since<br />
the beginning of the trial, that we recruit<br />
patients with truly cryptogenic stroke (and<br />
PFO) to get a definitive answer to these<br />
essential questions.”<br />
Thank you for your continued commitment<br />
to this important study.<br />
Scott Kasner, MD<br />
US Neurology Principal Investigator<br />
John Rhodes, MD<br />
US Cardiology Principal Investigator<br />
Lar Søndergaard, MD<br />
Nordic Region Cardiology Principal Investigator<br />
Lars Thomassen, MD, PhD<br />
Nordic Region Neurology Principal Investigator
U P C O M I N G E V E N T S<br />
Please Join Us...<br />
February 9 – 11 Los Angeles International Stroke Conference<br />
Booth #126<br />
2011 Scheduled GORE MEDICAL MASTERY SERIES Courses Sponsored by <strong>Gore</strong><br />
February 24 – 25 Durham Atrial Septal Defect Closure Course<br />
with an Animal Lab<br />
March 3 – 4 Chicago Atrial Septal Defect Closure Course<br />
with an Animal Lab<br />
March 24 – 25 Philadelphia Atrial Septal Defect Closure Course<br />
with an Animal Lab<br />
May * Detroit Atrial Septal Defect Closure Course<br />
with an Animal Lab and the assistance<br />
of a proctor<br />
* Date to be announced. Please check with your local <strong>Gore</strong> Sales Associate for further information.<br />
<strong>Gore</strong>’s commitment to excellence continues with the GORE MEDICAL MASTERY SERIES.<br />
The Atrial Septal Defect Closure courses provide Interventional Cardiologists with the<br />
opportunity to develop their knowledge of implant techniques. Contact your local <strong>Gore</strong><br />
Sales Associate for further information regarding these various course opportunities.<br />
If you have a topic that you would like us to consider in a future issue of Closing Remarks,<br />
please contact your local <strong>Gore</strong> Sales Associate or e-mail ClosingRemarks@wlgore.com<br />
W. L. <strong>Gore</strong> & Associates, Inc.<br />
Flagstaff, AZ 86004<br />
+65.67332882 (Asia Pacific) 800.437.8181 (United States)<br />
00800.6334.4673 (Europe) 928.779.2771 (United States)<br />
goremedical.com<br />
INDICATIONS FOR USE IN THE US: The GORE HELEX Septal Occluder is a permanently implanted prosthesis indicated for the percutaneous, transcatheter<br />
closure of ostium secundum atrial septal defects (ASDs). INDICATIONS FOR USE UNDER CE MARK: The GORE HELEX Septal Occluder is a permanently<br />
implanted prosthesis indicated for the percutaneous, transcatheter closure of atrial septal defects (ASDs), such as ostium secundum and patent foramen<br />
ovale. Refer to Instructions for Use at goremedical.com for a complete description of all contraindications, warnings, precautions and adverse events.<br />
Products listed may not be available in all markets.<br />
ACUNAV is a trademark of BioSense Webster ®<br />
STARFLEX ® is a trademark of NMT <strong>Medical</strong>, Inc.<br />
GORE ® , HELEX, PERFORMANCE BY DESIGN, and designs are trademarks of W. L. <strong>Gore</strong> & Associates.<br />
© 2010 W. L. <strong>Gore</strong> & Associates, Inc. AP4553-EN1 NOVEMBER 2010