BIOSIGNALS
BIOSIGNALS
BIOSIGNALS
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
<strong>BIOSIGNALS</strong><br />
generation<br />
processing<br />
analysis
BIOLOGICAL SYSTEMS<br />
Biological system is an open dynamic system with continuous flow of matter,<br />
energy and information.<br />
Information transport in biological systems<br />
The transport and processing of information in biological systems – human<br />
organism – is facilitated by humoral or nervous mechanisms on a three levels.<br />
The processes on the first lowest level are connected to the regulation of basic<br />
biochemical reactions. The second level forms processes carried out in<br />
autonomical systems utilizing humoral and nervous mechanisms, that control<br />
functions of some organs (e.g. heart). The third, highest level covers the<br />
information processing in central nervous system.
Energy in biological systems<br />
Energy for all the vital functions of the body is obtained by either aerobic or<br />
anaerobic metabolism:<br />
- Aerobic metabolism releases energy from carbohydrates, proteins and fats by<br />
the process of oxygenation. Aerobic metabolism is used by most cells, as it<br />
produces large amounts of energy for prolonged periods of time, but requires<br />
the presence of oxygen.<br />
- Anaerobic metabolism, in contrast, does not need oxygen but is far less efficient<br />
as it produces small amounts of energy and only functions for short periods<br />
of time.<br />
Therefore the body needs oxygen to produce the large amount of energy required<br />
for most body functions, not only for moving, but also for breathing, eating,<br />
digestion, osmotic function of kidneys, generation of action potentials and nerve<br />
function. A part is consumed, transformed into heat energy.<br />
This chemical-bound form of energy is stored in special molecules. The most<br />
known is ATP (adenosine-5'-triphosphate).<br />
The energy released by cleaving either a<br />
phosphate (Pi) or pyrophosphate (PPi) unit<br />
from ATP<br />
ATP + H2O ADP + Pi G˚ = −30.5 kJ/mol (−7.3 kcal/mol)<br />
ATP + H2O AMP + PPi G˚ = −45.6 kJ/mol (−10.9 kcal/mol)<br />
at the standard conditions,<br />
under typical cellular conditions, G is approximately −57 kJ/mol
Homeostasis and Adaptation<br />
Homeostasis (from Greek: standing still similar) is the property of a system, either<br />
open or closed, that regulates its internal environment and tends to maintain a<br />
stable, constant condition.<br />
All homeostatic control mechanisms have at least three interdependent<br />
components for the variable being regulated: The receptor is the sensing component<br />
that monitors and responds to changes in the environment. When the receptor senses<br />
a stimulus, it sends information to a control center, the component that sets the<br />
range at which a variable is maintained. The control center determines an appropriate<br />
response to the stimulus. In most homeostatic mechanisms the control center is the<br />
brain. The control center then sends signals to an effector, which can be muscles,<br />
organs or other structures that receive signals from the control center. After receiving<br />
the signal, a change occurs to correct the deviation by either enhancing it with<br />
positive feedback (e.g. blood platelet accumulation) or depressing it with negative<br />
feedback (regulation of blood pressure by vasoconstriction or vasodilatation).<br />
Homeostasis
Homeostasis and Adaptation<br />
Adaptation is the evolutionary process whereby a population becomes better suited<br />
to its habitat.<br />
May be structural, behavioral or physiological. Structural adaptations are<br />
physical features of an organism (shape, body covering, defensive or offensive<br />
armament); and also the internal organization). Behavioural adaptations are<br />
composed of inherited behaviour chains and/or the ability to learn: behaviours may<br />
be inherited in detail (instincts), or a tendency for learning may be inherited. E.g.:<br />
searching for food, mating, vocalizations. Physiological adaptations permit the<br />
organism to perform special functions (for instance making venom, secreting slime,<br />
phototropism); but also more general functions such as growth and development,<br />
temperature regulation, ionic balance and other aspects of homeostasis. Adaptation,<br />
then, affects all aspects of the life of an organism.
BIOLOGICAL SIGNAL<br />
is a summarizing term for all kinds of signals that can be (continually) measured<br />
and monitored from biological beings. The term biosignal is often used to mean<br />
bio-electrical signal but in fact, biosignal refers to both electrical and non-electrical<br />
signals.<br />
Electrical biosignals are usually taken to be (changes in) electric currents<br />
produced by the sum of electrical potential differences across a specialized tissue,<br />
organ or cell system like the nervous system.<br />
Information in biosignals is often depreciated by a disturbance or noise. Therefore<br />
the biosignals have to be properly processed – using a transformation or filtration<br />
to extract required information.<br />
There are a lots of methods and<br />
algorithms for biosignal processing, 1-<br />
or 2-dimensional, in time or in<br />
frequency distribution.
Classification of Biosignals<br />
may be classified in many ways<br />
according to:<br />
• to their source or physical nature, where the classification respects the basic<br />
physical characteristics of the considered process.<br />
• to biomedical application. The biomedical signal is acquired and processed<br />
with some diagnostic, monitoring, or other goal in mind. Classification may be<br />
constructed according to the field of application, e.g., cardiology or neurology.<br />
Such classification may be of interest when the goal is, for example, the study of<br />
physiologic systems.<br />
• to signal characteristics. From point of view of signal analysis, this is the<br />
most relevant classification method. When the main goal is processing, it is not<br />
relevant what is the source of the signal or to which biomedical system it belongs;<br />
what matters are the signal characteristics.
We recognize two broad classes of signals:<br />
- continuous signals<br />
- discrete signals.<br />
Continuous signals are described by a continuous function s (t) which provides<br />
information about the signal at any given time. Discrete signals are described by a<br />
sequence s (m) which provides information at a given discrete point on the time<br />
axis.<br />
Continuous<br />
Discrete<br />
value<br />
value<br />
time<br />
time<br />
Most of the biomedical signals are continuous. Since current technology<br />
provides powerful tools for discrete signal processing, we most often transform a<br />
continuous signal into a discrete one by a process known as sampling.
We divide signals into two main groups:<br />
- deterministic<br />
- stochastic signals.<br />
Deterministic signals are signals that can be exactly described mathematically or<br />
graphically. Real-world signals are never deterministic. There is always some<br />
unknown and unpredictable noise added, some unpredictable change in the<br />
parameters. It is very often convenient to approximate or model the signal by<br />
means of a deterministic function(s).<br />
An important family of deterministic signals is the periodic family. A periodic<br />
signal is a deterministic signal that may be expressed by<br />
s(t )= s(t + nT)<br />
where n is an integer, and T is the period.<br />
Under some conditions, the blood pressure<br />
signal may be modeled by a complex periodic<br />
signal, with the heart rate as its period and the<br />
blood pressure wave shape as its basic wave<br />
shape.
Most deterministic functions are nonperiodic. It is sometimes worthwhile to consider<br />
an “almost periodic” type of signal. The ECG signal can sometimes be considered<br />
“almost periodic.” The ECG’s RR interval is never constant; in addition, the PQRST<br />
complex of one heartbeat is never exactly the same as that of another beat.<br />
The most important class of signals is the stochastic class. Stochastic signals<br />
cannot be expressed exactly; they can be described only in terms of probabilities.<br />
Stationary stochastic processes are processes whose statistics do not<br />
change in time. The expectation and the variance (as with any other statistical<br />
mean) of a stationary process will be time-independent. Unfortunately, almost all<br />
signals are nonstationary (e.g. sleep EEG signal)<br />
the 3. and/or the 4.<br />
stage of the nonREM<br />
sleep phase
Types of biosignals<br />
according to the origin<br />
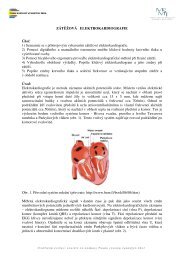
a) Bioelectric signals. They are generated by nerve<br />
cells and muscle cells. Its source is the membrane potential,<br />
which under certain conditions may be excited to generate an<br />
action potential. In single cell measurements, where specific<br />
microelectrodes are used as sensors, the action potential<br />
itself is the biomedical signal. In more gross measurements,<br />
where, for example, surface electrodes are used as sensors,<br />
the electric field generated by the action of many cells,<br />
distributed in the electrode’s vicinity, constitutes the bioelectric<br />
signal. The electric field propagates through the biologic<br />
medium, and thus the potential may be acquired at relatively<br />
convenient locations on the surface, eliminating the need to<br />
invade the system. The bioelectric signal requires a relatively<br />
simple transducer for its acquisition. E.g.: ECG, EEG, EMG<br />
and others.
) Bioimpedance signals. The impedance of the tissue contains important<br />
information concerning its composition, blood volume, blood distribution, endocrine<br />
activity, automatic nervous system activity, and more. The bioimpedance signal is<br />
usually generated by injecting (or superficially) into the tissue under test sinusoidal<br />
currents (frequency range of 50 kHz to 1 MHz, with low current densities of the<br />
order of 20 A to 2 mA). The frequency range is chosen to minimize electrode<br />
polarization problems, and the low current densities are chosen to avoid tissue<br />
damage mainly due to heating effects. Bioimpedance measurements are usually<br />
performed with 4 electrodes. Two source electrodes are connected to a current<br />
source and are used to inject the current into the tissue. The two measurement<br />
electrodes are placed on the tissue under investigation and are used to measure the<br />
voltage drop generated by the current and the tissue impedance. E.g.: impedance<br />
plethysmography or rheography.
c) Biomagnetic signals. Various organs, such as the brain, heart, and lungs,<br />
produce extremely weak magnetic fields (10 −9 T to 10 −6 T). The measurements<br />
of these fields provides information not included in other biosignals (such as<br />
bioelectric signals). Due to the low level of the magnetic fields to be measured,<br />
biomagnetic signals are usually of very low signal-to-noise ratio. Extreme caution<br />
must be taken in designing the acquisition system of these signals.
Superconducting quantum interference devices (SQUID) are very sensitive<br />
magnetometers used to measure extremely weak magnetic fields, based on<br />
superconducting loops containing Josephson junctions. They are sensitive enough<br />
to measure fields as low as 5×10 −18 T. The strength of the field at the Earth's<br />
surface ranges from less than 3x10 -5 T in an area including most of South America<br />
and South Africa to over 6x10 -5 T around the magnetic poles in northern Canada<br />
and south of Australia, and in part of Siberia. ( A typical refrigerator magnet<br />
produces 10 −2 T.
d) Bioacoustic signals. Many biomedical phenomena create acoustic noise. The<br />
flow of blood in the heart, through the heart’s valves, or through blood vessels<br />
generates typical acoustic noise. The flow of air through the upper and lower<br />
airways and in the lungs creates acoustic sounds. These sounds, known as<br />
coughs, snores, and chest and lung sounds, are used extensively in medicine.<br />
Sounds are also generated in the digestive tract and in the joints. It also has been<br />
observed that the contracting muscle produces an acoustic noise (muscle noise).<br />
Since the acoustic energy propagates through the biologic medium, the<br />
bioacoustic signal may be conveniently acquired on the surface, using acoustic<br />
transducers (microphones or accelerometers).<br />
e) Biochemical signals. Biochemical signals are the result of chemical<br />
measurements from the living tissue or from samples analyzed in the clinical<br />
laboratory. Measuring the concentration of various ions inside and in the vicinity of<br />
a cell by means of specific ion electrodes is an example of such a signal. Partial<br />
pressures of oxygen (pO 2<br />
) and of carbon dioxide (pCO 2<br />
) in the blood or respiratory<br />
system are other examples or blood pH. Biochemical signals are most often very<br />
low frequency signals. Most biochemical signals are actually dc signals.
f) Biomechanical signals. The term biomechanical signals includes all signals used<br />
in the biomedicine fields that originate from some mechanical function of the biologic<br />
system. These signals include motion and displacement signals, pressure and<br />
tension and flow signals, and others. The measurement of biomechanical signals<br />
requires a variety of transducers, not always simple and inexpensive.<br />
The mechanical phenomenon does not propagate, as do the electric, magnetic, and<br />
acoustic fields. The measurement therefore usually has to be performed at the exact<br />
site. This very often complicates the measurement and forces it to be an invasive<br />
one. E.g. blood pressure, non-directly – phonocardiography, Carotidography.<br />
g) Biooptical signals. Biooptical signals are the result of optical functions of the<br />
biologic system, occurring naturally or induced by the measurement. Blood<br />
oxygenation may be estimated by measuring the transmitted and backscattered<br />
light from a tissue (in vivo and in vitro) in several wavelengths (oximetry). Important<br />
information about the fetus may be acquired by measuring fluorescence<br />
characteristics of the amniotic fluid. Estimation of the heart output may be<br />
performed by the dye dilution method, which requires the monitoring of the<br />
appearance of recirculated dye in the bloodstream. The development of fiberoptic<br />
technology has opened vast applications of biooptical signals.
h) Thermal biosignals – continuous or discrete carry information about the<br />
temperature of the body core or temperature distribution on the surface. The<br />
temperature measurement reflects physical and biochemical processes proceeded<br />
in organism. The measurement is usually performed by a contact method using a<br />
variety of thermometers. In special cases it is used 2D thermographic camera.<br />
i) Radiological biosignals. These biosignals are formed by<br />
interaction of ionizing interaction with biological structures.<br />
They carry information about inner anatomical structures.<br />
They play a significant role in diagnostics and therapy.<br />
j) Ultrasonic biosignals. They are formed by interaction<br />
with organism tissues. They carry information about<br />
acoustic impedances of biological structures and their<br />
anatomical changes. They are acquired by probes<br />
containing piezoelectric transducer.
Electronic devices in Medicine<br />
Block diagram of a diagnostic device<br />
sensor<br />
amplifier<br />
A/D<br />
converter<br />
calibration<br />
control<br />
unit<br />
signal<br />
processing<br />
data<br />
storage<br />
source<br />
signal<br />
display<br />
data<br />
transfer
Electronic devices in Medicine<br />
Diagnostic systems<br />
Electric signals are detected by sensors (mainly electrodes), while nonelectric<br />
magnitudes are first converted by transducers into electric signals that can be<br />
easily treated, transmitted, and stored. The output signals from electrodes or<br />
sensors of the most monitored quantities are analog. For their processing, storage<br />
and transport is necessary to do their amplification, filtration and digitalization<br />
using A/D converter.<br />
Different types of microprocessors are used to process biosignals (PC serves as a<br />
control unit).<br />
The control unit of modern electrocardiographs
Signal display usually respects user requirements. They are displays with<br />
numerical or graphical information (light emitting diodes LED, LCD, monitors).<br />
Data storage (e.g. Holter long-term (24- 48hrs) monitoring ECG, blood<br />
pressure or pH of stomach).<br />
Data transmission locally inside of the clinic or via hospital information system<br />
(HIS), but also to other places by phone, internet or telemetrically.
Block diagram of a therapeutic device<br />
source<br />
life<br />
functions<br />
monitoring<br />
signal<br />
display<br />
dose<br />
monitoring<br />
applicator<br />
generator<br />
control<br />
unit<br />
therapeutical<br />
watch<br />
Applicators are stimulation electrodes, tips, cavity resonators, ultrasound heads,<br />
coils, optical fibers and others, that directly act on specified area of the tissue,<br />
organ.
Signal digitalization<br />
The A/D conversion ideally can be divided in two steps, the sampling process,<br />
which converts the continuous signal in a discrete-time series and whose elements<br />
are named samples, and a quantization procedure, which assigns the amplitude<br />
value of each sample within a set of determined discrete values. Both processes<br />
can modify the characteristics of the signal. A continuous time signal can be<br />
completely recovered from its samples if, and only if, the sampling rate is greater<br />
than twice the signal bandwidth (Shanon-Kotelnikov theorem).
Sensors of biosignals<br />
different types of electrodes and sensors<br />
Biomedical sensors<br />
take signals representing biomedical variables and convert them into what is<br />
usually an electrical signal. As such, the biomedical sensor serves as the interface<br />
between a biologic and an electronic system.<br />
It is possible to categorize all sensors as being either physical or chemical.<br />
In the case of physical sensors, quantities such as geometric, mechanical, thermal,<br />
and hydraulic variables are measured. In biomedical applications these can include<br />
things such as muscle displacement, blood pressure, core body temperature, blood<br />
flow, cerebrospinal fluid pressure, and bone growth.<br />
The second major classification of sensing devices is chemical sensors. In this<br />
case the sensors are concerned with measuring chemical quantities such as<br />
identifying the presence of particular chemical compounds, detecting the<br />
concentrations of various chemical species, and monitoring chemical activities<br />
in the body for diagnostic and therapeutic applications.
Measurement of biological signals (physical quantities)<br />
Some important biosignals do not have the character of the electrical potential or<br />
voltage. The monitoring can be carried out only with the sensors transforming that<br />
signal as a physical quantity to some form of the electrical signal.<br />
Displacement sensors<br />
Inductance sensors of a displacement use inductance changes of a coil at the<br />
change of ferromagnetic slug position. The inductance is given by the formula:<br />
where µ 0<br />
is permeability of vacuum, µ r<br />
is relative permeability of the ferromagnetic<br />
slug, G is constant and characterizes the coil shape, N is the number of turns.
Capacitive Sensors for displacement monitoring use the changes of the capacitance<br />
of the plate condenser based on the following formula:<br />
S<br />
where ε 0<br />
is permittivity of vacuum, ε r<br />
relative permittivity of dielectric (air), S is plate<br />
area, d is plate distance.<br />
If for example if one plate is fixed then the capacitance will vary<br />
inversely with respect to the plate separation. This will result in a<br />
hyperbolic capacitance-displacement characteristic. These<br />
sensors can be used for monitoring of patient movement in bed,<br />
but also can be applied for respiration measurements, gas or<br />
liquid pressure.<br />
Sensors of the blood velocities and flows<br />
For the non-invasive measurement of the blood speeds or<br />
flows there are used piezoelectric transducers in ultrasound<br />
Dopller instruments. They are usually ceramic piezoelectric<br />
transducers working on frequencies from 4 to 10 MHz in<br />
continuous or pulse mode. The piezoelectric transducers can<br />
be also used for blood pressure measurement or for<br />
observation of heart valves movement in phonocardiography.<br />
Sensor of the intraocular pressure
Sensors of the air flow<br />
mesh<br />
warming<br />
Fleish’s pneumotachometer<br />
measure flow rate by means of a transducer through which the patient breathes.<br />
The air passes through a fine mesh which offers a small resistance to flow, with<br />
the result that there will be a pressure drop across the mesh in proportion to the<br />
flow rate. The instrument also calculates volume by integrating the flow signal.<br />
The tube cone shaped ends provide laminar air flow around the pressure<br />
transducer. The mesh warming facilitates water evaporation.
Sensors of temperature<br />
There are many different sensors of temperature, but three find particularly wide<br />
application to biomedical problems - metallic resistance thermometers,<br />
thermistors, and thermocouples.<br />
Metallic Resistance Thermometers<br />
The electric resistance of a piece of metal or wire generally increases as the<br />
temperature of that electric conductor increases. A linear approximation to this<br />
relationship is given by<br />
R = R 0<br />
[ 1+α (T −T 0<br />
)]<br />
where R 0<br />
is the resistance at temperature T 0<br />
, is the temperature coefficient of<br />
resistance, and T is the temperature at which the resistance is being measured.
Most metals have temperature coefficients of resistance of the order of 0.1– 0.4%/°C.<br />
The noble metals are preferred for resistance thermometers, since they do not<br />
corrode easily.<br />
Metal resistance thermometers are often fabricated from fine-gauge insulated wire<br />
that is wound into a small coil.
Thermistors<br />
Unlike metals, semiconductor materials have an inverse relationship between<br />
resistance and temperature. Their resistance as a function of temperature is given<br />
by<br />
where R 0<br />
marks thermistor resistance at the reference temperature T 0<br />
(298,15 K=25<br />
°C), β is a constant determined by the materials that make up the thermistor, the<br />
temperature constants for current materials are between 1500 and 7000 K.<br />
Thermistors are usually made of a mixture of metal oxides such as FeO, NiO, MnO,<br />
TiO, CoO.
Thermocouples<br />
When different regions of an electric conductor or semiconductor are at different<br />
temperatures, there is an electric potential between these regions that is directly<br />
related to the temperature differences. This phenomenon, known as the Seebeck<br />
effect, can be used to produce a temperature sensor known as a thermocouple<br />
by taking a wire of metal or alloy A and another wire of metal or alloy B and<br />
connecting them.<br />
When these junctions are at different temperatures, a voltage proportional to the<br />
temperature difference will be seen at the voltmeter<br />
V = S AB<br />
(Ts–Tr)<br />
where S AB<br />
is the Seebeck coefficient for the thermocouple made up of metals A<br />
and B
Infrared thermometers<br />
measure temperature by measuring infrared radiation emitted from objects. The<br />
object's temperature can be determined if you know the amount of infrared energy<br />
emitted by the object and its emissivity.<br />
The Stefan–Boltzmann law, also known as Stefan's law, states that the total<br />
energy radiated per unit surface area of a black body in unit time (known variously<br />
as the black-body irradiance, energy flux density, radiant flux, or the emissive<br />
power), H, is directly proportional to the fourth power of the black body's<br />
thermodynamic temperature T:<br />
H = ε . σ . T 4
Oximetry measures the degree of oxygen saturation in blood<br />
The oxygen is under normal physiological conditions transported from lungs to<br />
tissues in 2 different forms. Approximately 2 % of the total blood O 2<br />
is dissolved in<br />
plasma – it is linearly proportional to the p0 2<br />
in blood. The rest (98 %) is carried on<br />
erythrocytes, rather is reversible bound to hemoglobin producing oxyhemoglobin<br />
HbO 2<br />
. Based on this facts, there are 2 approaches to measure the blood<br />
oxygenation: application of p0 2<br />
sensor or measurement O 2<br />
saturation (relative<br />
content of HbO 2<br />
in blood) with an oximeter.<br />
Oximetry is based on the light absorption by blood (the color of fully oxygenated<br />
blood is bright red)<br />
A, B are coefficients dependent on specific<br />
absorption of Hb and HbO 2 , H(λ1), H(λ2) are<br />
optical densities of blood λ1 and λ2, resp.<br />
Pulse oximeter facilitates non-invasive in vivo measurement of oxygen saturation in<br />
blood. The sensor is formed by 2 light emitting diodes LED working on 2 different<br />
wavelengths :<br />
- λ 1<br />
where is significant difference between light absorption of Hb and HbO 2<br />
(red color<br />
660 nm ),<br />
- λ 2<br />
where light absorption is independent on oxygen saturation in blood (the<br />
absorbance of Hb is slightly lower than for HbO 2<br />
(IR 960 nm ).
Biosignal processing<br />
The most of the biosignals are acquired in the time domain. On the other hand for<br />
their processing it is better to work with the frequency distribution (e.g. to<br />
remove a noise by a frequency dependent filter).<br />
The basic mathematical operation serves for biosignal transformation from the<br />
time domain to the frequency domain is Fourier transformation.<br />
For any periodic biosignal we can use Fourier series<br />
and so describe the signals by means of the amplitudes a n<br />
,b n<br />
and phases of the<br />
sine waves. ( = 2f is the angular frequency)
Electrical signals processing – 3 steps:<br />
1. sensing<br />
(electrical signals are collected as electrical voltages, with amplitude from 10 -6 V<br />
(EEG) to 10 -2 V (EMG), their frequency is also in a wide range from 10 -1 to 10 3<br />
Hz)<br />
2. amplification<br />
(2 types: direct current (voltage) amplifier and alternating amplifier, the both<br />
have to be frequency independent)<br />
3. recording
Biophysics of sensory perception<br />
Classification and characteristics of receptors<br />
Psychophysical laws
Our perception of the outside world depends on our five senses:<br />
Cutaneous sensation<br />
Gustation<br />
Olfaction<br />
Vision<br />
Audition<br />
Touch<br />
Taste<br />
Smell<br />
Sight<br />
Hearing<br />
The elements of the peripheral nervous system that respond directly to stimuli are<br />
called the sensory receptors.<br />
A receptor is a transducer that produces electrical energy, impulse, from a form of<br />
energy (mechanical, thermal, light).<br />
The internal receptors (interoceptors, viscoreceptors and proprioceptors) monitor<br />
position and function of the organs, muscles, joints, ligaments, etc.<br />
The elements located at or near to the surface of the body - exteroceptors.
The classification according to function depends on the transduction<br />
mechanism of the receptor.<br />
Mechanoreceptors transduce mechanical factors such as touch, pressure,<br />
vibration and strain into electrical activity.<br />
Thermoreceptors respond to temperature<br />
Photoreceptors to light<br />
Chemoreceptors respond to chemicals in solution<br />
Nociceptors are pain sensors, if the stimulus level is high enough<br />
Some receptors are designed specifically to respond to the level of a stimulus,<br />
whilst others are designed to respond to changes in the level. (e.g. some<br />
mechanoreceptors respond directly to pressure and some respond to vibration)
Mechanoreceptors<br />
associated with the sense of touch<br />
structurally relatively simple<br />
CUTANEOUS SENSATION<br />
The categorization of the simple receptors depends on the geometry of the dendritic<br />
endings<br />
Encapsulated dendritic endings are contained in a protective capsule of connective<br />
tissue. Some are designed to respond to light pressure, some to higher pressure,<br />
some to strain and some to vibration.<br />
-Pacinian corpuscles detect rapid vibrations, with large receptive fields<br />
-Meissner’s corpuscle (glabrous skin only) detect slow vibrations<br />
-Ruffini corpuscles (plus Merkel’s disks on glabrous skin) respond to<br />
indentation, with slow adaptation<br />
Free nerve endings around hairs detect movements of hairs<br />
Nociceptors (pain receptors) and thermoreceptors belong into this section because<br />
of their structural similarity
Mechanoreceptors respond to the stimulus of a mechanical load<br />
are designed to respond to the intensity of the load (slowly adapting (SA)<br />
receptors) and some are designed to respond to the rate of change of load (rapidly<br />
adapting (RA) receptors)<br />
The rate of generation of impulses is distinctly non-linear to the intensity of the<br />
stimulus, and furthermore there is a fatigue effect so that the rate is not constant<br />
even for constant stimulus.
Structural Categories of Sensory Receptors<br />
Pain<br />
temperature<br />
Touch<br />
Pressure
The Pacinian corpuscle<br />
- the most abundant in the subcutaneous tissue under the skin, particularly in the<br />
fingers, the soles of the feet and the external genitalia<br />
- the largest of the receptors and the approximate shape of a rugby ball, typically<br />
about 1 mm, and up to 2 mm, long and about half as wide<br />
-resemble an onion in structure, with up to 60 layers of flattened cells surrounding a<br />
central core, the whole being enclosed in a sheath of connective tissue. At the<br />
centre is a single non-myelinated nerve fibre of up to 10 µm in diameter, which<br />
becomes myelinated as it leaves the corpuscle.<br />
- The Pacinian corpuscle serves most efficiently as a monitor of the rate of change<br />
of load rather than to the intensity of the load itself: serves as a vibration<br />
transducer.
The Pacinian corpuscle<br />
Load applied slowly<br />
Load applied rapidly<br />
The presented model suggests that the mechanical stimulus reaching the core will<br />
depend on the rate of loading.<br />
Consider the application of a pinching load to two concentric ovoids filled with an<br />
incompressible viscous fluid. If the load is applied very slowly then the fluid flows so<br />
that the elastic membrane of the outer ovoid stretches along the axis to maintain<br />
the enclosed volume of incompressible fluid.<br />
If the load is applied rapidly, there will be a local high pressure under the point of<br />
application of the load, and therefore some distortion of the circular section of the<br />
membrane. This must be accommodated by a stretching along the axis.
Density of mechanoreceptors in human skin<br />
Site<br />
Tip of tongue<br />
Tip of index finger<br />
Lips<br />
Edge of tongue<br />
Palm<br />
Forehead<br />
Back of hand<br />
Upper surface of foot<br />
Neck<br />
Back<br />
Spatial discrimination<br />
(cm)<br />
0.2<br />
0.5<br />
0.75<br />
1<br />
1.2<br />
2.5<br />
3.2<br />
4.0<br />
5.5<br />
6.8<br />
Spatial density<br />
(receptors per cm 2 )<br />
25<br />
4<br />
2<br />
1<br />
0.7<br />
0.16<br />
0.1<br />
0.06<br />
0.03<br />
0.02
Thermoreceptors<br />
free nerve endings, respond to the stimulus of heat energy<br />
there are few thermoreceptors in the human skin - of the order of 5 to 10 receptors<br />
per cm 2 .<br />
Some receptors are designed to monitor steady-state temperature, whilst others<br />
respond efficiently to rapid changes of temperature.<br />
Some of the steady-state receptors, the “hot detectors”, respond to high<br />
temperatures, and some, the “cold detectors”, respond to low temperatures.<br />
Warm receptors<br />
sensitive to temperatures above 30 o C<br />
unresponsive to temperature above 48 o C<br />
Cold receptors<br />
sensitive to temperature between<br />
10 o C and 35 o C<br />
Pain receptors<br />
respond to temperatures below<br />
10 o C<br />
and above 45 o C<br />
frequency AP/s<br />
cold receptors<br />
hot receptors<br />
temperature °C
Nociceptors<br />
free nerve endings networks<br />
signal pain when the intensity of stimulation exceeds a particular threshold -<br />
intense pressure, heat, acids, receptors that are sensitive to ATP level<br />
there are rapid pain receptors, transmitting through myelinated fibers, that let<br />
us know very quickly that something is wrong. The conduction velocity of these<br />
nerve fibers is up to 30 m s -1 .<br />
there are also persistent pain receptors, mostly non-myelinaled, that react<br />
more slowly but maintain the sensation of pain - conduction velocities down to 2 m<br />
s -1 and below.<br />
Myelination<br />
Most mammalian axons are myelinated.<br />
The myelin sheath is provided by oligodendrocytes and Schwann cells.<br />
Myelin is insulating, preventing passage of ions over the membrane.<br />
Saltatory Conduction<br />
Myelin<br />
sheath<br />
Node of<br />
Ranvier
The chemical senses<br />
gustation and olfaction, or taste and smell<br />
They are dependent on the chemical stimulation of special cells called<br />
chemoreceptors, which respond to chemicals in an aqueous solution.<br />
They are regarded as the most primitive of the special senses.<br />
Our perception of taste in particular is often a composite sense, in which we<br />
supplement true taste information with cues from our sense of smell.
Gustation (taste)<br />
The chemoreceptors responsible for the sense of taste are called taste buds.<br />
We have about 10 000 of them, most of which are located on the tongue.<br />
They are shed and replaced about every 7-10 days.<br />
Different areas of the tongue react most effectively to particular tastes, suggesting<br />
that the taste buds have some degree of specificity. Every taste bud appears to be<br />
able to react to every taste, but the level of response varies. There is no obvious<br />
structural difference between the taste buds that respond best to different tastes.<br />
The task of transmission of the taste sensation to the brain is shared between two<br />
of the cranial nerves — the seventh (facial) and the ninth (glossopharyngeal).<br />
Epithelial cell receptors clustered<br />
in taste buds.<br />
Taste cells are not neurons, but<br />
depolarize upon stimulation and<br />
release chemical transmitters that<br />
stimulate sensory neurons.
Classification of tastes<br />
We normally classify tastes into four<br />
categories.<br />
In taste tests some compounds appear to fall<br />
into different categories depending on<br />
concentration. Even common salt, sodium<br />
chloride, tastes sweet at very low<br />
concentrations, close to the threshold of taste.<br />
Classification of tastes<br />
bitter<br />
sour<br />
sweet<br />
salt<br />
Location of taste sites<br />
on the human tongue<br />
Category<br />
General<br />
Specific<br />
Sweet<br />
Salt<br />
Sour<br />
Bitter<br />
Many organic<br />
compounds<br />
Many inorganic<br />
salts, metal ions<br />
Acids, hydrogen<br />
ion (H+)<br />
Many alkaloids<br />
Sugars, saccharin<br />
Sodium chloride,<br />
potassium chloride<br />
Acetic acid (vinegar),<br />
citric acid (lemon)<br />
Caffeine, nicotine,<br />
quinine, strychnine<br />
Salt:<br />
Na+ passes through channels<br />
and activates specific receptor<br />
cells, depolarizing the cells.<br />
Sour:<br />
Presence of H+.<br />
Sweet and bitter:<br />
Mediated by receptors coupled<br />
to G-protein (gustducin).
Olfaction (smell)<br />
The chemoreceptors responsible for the sense of smell, the olfactory receptors,<br />
are located in the epithelial lining of the roof of the nasal cavity.<br />
There are millions of these receptors. Man has a relatively poor sense of smell,<br />
and part of the reason for this is the geometrical design of the olfactory system.<br />
The olfactory receptors are situated in a side passage, off the main pathway of air<br />
into the lungs.<br />
Unlike the taste buds, which<br />
consist of epithelial cells, the<br />
olfactory receptors are actually<br />
neurones.<br />
They are unique in that they are<br />
the only neurones in the body<br />
that are replaced continually in<br />
adult life. They typically last for<br />
about 60 days.<br />
The task of transmission of the<br />
sensation of smell to the brain is<br />
performed by the first cranial<br />
nerve - the olfactory nerve.<br />
Molecules bind to<br />
receptors and act<br />
through G-proteins<br />
to increase cAMP.
Classification of smells<br />
There are several theories of olfaction, and no doubt each contains an element of<br />
the true. Many of the theories are underpinned by chemical models. One appealing<br />
and simple model suggests that there are seven basic odours: camphoric, musky,<br />
floral, pepperminty, ethereal, pungent and putrid. More complex models suggest 30<br />
or more primary odours, and more recent work suggests that there are a thousand<br />
or more separately identifiable odours.<br />
Thresholds of smell<br />
Our sense of smell is very sensitive - the threshold concentration for ethyl<br />
mercaptan as 4 x 10 8 molecules per cm 3 . Given that there are about 5 x 10 19<br />
molecules of nitrogen per cm 3 , this suggests that we can detect ethyl mercaptan in<br />
air at a concentration of about one molecule in 10 11 . We might consider this to be<br />
quite impressive, but the threshold of smell for a typical dog is about one thousand<br />
times lower.