choice of drugs for use in syringe drivers - Palliative Care Resources
choice of drugs for use in syringe drivers - Palliative Care Resources
choice of drugs for use in syringe drivers - Palliative Care Resources
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
LIVERPOOL CARE PATHWAY FOR THE DYING PATIENT<br />
PRINCIPLES OF MANAGEMENT<br />
The pr<strong>in</strong>ciples are applicable to the care <strong>of</strong> patients dy<strong>in</strong>g from cancer and non-malignant disease.<br />
RECOGNISE THAT DEATH IS APPROACHING<br />
Studies have found that dy<strong>in</strong>g patients will manifest some or all <strong>of</strong> the follow<strong>in</strong>g:<br />
• Pr<strong>of</strong>ound weakness - usually bedbound<br />
• Drowsy or reduced cognition - semi-comatose<br />
• Dim<strong>in</strong>ished <strong>in</strong>take <strong>of</strong> food and fluids - only able to take sips <strong>of</strong> fluid<br />
• Difficulty <strong>in</strong> swallow<strong>in</strong>g medication - no longer able to take tablets<br />
TREATMENT OF SYMPTOMS<br />
The prime aim <strong>of</strong> all treatment at this stage is the control <strong>of</strong> symptoms current and potential.<br />
• Discont<strong>in</strong>ue any medication which is not essential<br />
• Prescribe medication necessary to control current distress<strong>in</strong>g symptoms<br />
• All patients who are dy<strong>in</strong>g would benefit from hav<strong>in</strong>g subcutaneous medication prescribed<br />
IN CASE distress<strong>in</strong>g symptoms develop<br />
• All medication needs should be reviewed every 24 hours<br />
• If two or more doses <strong>of</strong> prn medication have been required, then consider the <strong>use</strong> <strong>of</strong> a<br />
syr<strong>in</strong>ge driver <strong>for</strong> cont<strong>in</strong>uous subcutaneous <strong>in</strong>fusion (CSCI)<br />
The most frequently reported symptoms are:-<br />
• Pa<strong>in</strong><br />
• Na<strong>use</strong>a / Vomit<strong>in</strong>g<br />
• Excessive secretions / Noisy breath<strong>in</strong>g<br />
• Agitation / Restlessness<br />
• Dyspnoea<br />
OPIOID CHOICE AND SYRINGE DRIVERS<br />
Morph<strong>in</strong>e sulphate is the <strong>in</strong>jectable opioid <strong>of</strong> <strong>choice</strong> <strong>in</strong> the majority <strong>of</strong> patients.<br />
Alternative opioids (when morph<strong>in</strong>e is not tolerated or <strong>in</strong> patients with severe renal failure e.g GFR <<br />
30mL /m<strong>in</strong>) <strong>in</strong>clude oxycodone or alfentanil.<br />
Morph<strong>in</strong>e sulphate and oxycodone are both compatible with all the medications that are<br />
recommended <strong>in</strong> the follow<strong>in</strong>g guidel<strong>in</strong>es (cycliz<strong>in</strong>e, haloperidol, levomepromaz<strong>in</strong>e, hyosc<strong>in</strong>e<br />
butylbromide, glycopyrronium, metoclopramide and midazolam).<br />
Alfentanil is also compatible with all the above medications that are recommended, with the<br />
exception <strong>of</strong> cycliz<strong>in</strong>e.<br />
Use either water <strong>for</strong> <strong>in</strong>jection or sodium chloride 0.9 % as the diluent, unless mix<strong>in</strong>g with cycliz<strong>in</strong>e,<br />
when water <strong>for</strong> <strong>in</strong>jection must be <strong>use</strong>d.<br />
Although 10mL syr<strong>in</strong>ges are the standard size usually <strong>use</strong>d <strong>in</strong> the syr<strong>in</strong>ge driver, if volumes are<br />
larger it may be necessary to <strong>use</strong> a 20mL or 30mL syr<strong>in</strong>ge <strong>in</strong>stead.<br />
For more <strong>in</strong><strong>for</strong>mation on the usual doses <strong>of</strong> <strong>drugs</strong> <strong>use</strong>d <strong>in</strong> a syr<strong>in</strong>ge driver see page 41<br />
For guidance on convert<strong>in</strong>g between opioids see the back page.<br />
Contacts <strong>for</strong> cl<strong>in</strong>ical advice are on page 3<br />
For advice on compatibility contact Pharmacy Medic<strong>in</strong>es In<strong>for</strong>mation ext 5960<br />
The algorithms will support you <strong>in</strong> your management <strong>of</strong> the most frequently reported symptoms.<br />
1
PAIN CONTROL<br />
(Non renal pathway – see next page <strong>for</strong> patients with renal failure)<br />
Strong opioid Conversion to s/c morph<strong>in</strong>e over 24 hours Example<br />
Zomorph/ MST Divide total oral morph<strong>in</strong>e dose by 2 Zomorph 30mg bd = 30mg Morph<strong>in</strong>e s/c <strong>in</strong> 24 hours<br />
Fentanyl patch Standard practice is to leave fentanyl patch on<br />
patient and change every 3 days.<br />
Top up with s/c doses <strong>of</strong> morph<strong>in</strong>e and review.<br />
Fentanyl patch 75 microgram changed every 72 hours<br />
is approximately equivalent to<br />
morph<strong>in</strong>e 270mg oral or 140mg s/c over 24 hours<br />
To calculate prn s/c morph<strong>in</strong>e dose to supplement<br />
patch<br />
a) Work out equivalent 24 hour oral morph<strong>in</strong>e dose <strong>for</strong><br />
a given patch<br />
b) Divide by 2 to get s/c 24 hour morph<strong>in</strong>e dose<br />
c) Divide by 6 to get s/c morph<strong>in</strong>e prn dose<br />
The prn dose can be given every 4 hours up to a<br />
maximum <strong>of</strong> 6 prn doses <strong>in</strong> 24 hours<br />
A syr<strong>in</strong>ge driver may be required if 2 or more prn doses<br />
are <strong>use</strong>d.<br />
Subsequent breakthrough dose should be calculated<br />
from the dose <strong>of</strong> morph<strong>in</strong>e <strong>in</strong> the syr<strong>in</strong>ge driver and the<br />
equivalent given by patch<br />
2<br />
Leave patch on and calculate <strong>in</strong>itial prn dose as 1/6 th<br />
<strong>of</strong> 140mg morph<strong>in</strong>e s/c over 24 hours = 25mg<br />
A syr<strong>in</strong>ge driver may be required if 2 or more doses<br />
<strong>use</strong>d <strong>in</strong> the past 24 hours.<br />
E.g. If 2 prn doses are <strong>use</strong>d (2 x 25mg) the syr<strong>in</strong>ge<br />
driver would be set up with 50mg morph<strong>in</strong>e s/c over 24<br />
hour<br />
Calculate subsequent prn morph<strong>in</strong>e s/c doses<br />
Add morph<strong>in</strong>e syr<strong>in</strong>ge driver dose i.e 50mg s/c with<br />
equivalence <strong>in</strong> patch i.e 140mg morph<strong>in</strong>e s/c.<br />
Total equivalent s/c morph<strong>in</strong>e dose <strong>in</strong> 24 hour = 50mg<br />
+ 140mg =190mg<br />
New prn doses would be 1/6 th <strong>of</strong> 190mg = 32mg<br />
(prescribe 30mg <strong>for</strong> convenience).<br />
Consult opioid conversion chart on back page<br />
Remember to <strong>in</strong>clude prn doses <strong>in</strong> your calculations
PAIN CONTROL<br />
(Patients with severe renal failure ie GFR < 30mL/m<strong>in</strong>)<br />
Strong opioid Conversion to s/c alfentanil over 24 hours Example<br />
MST/ Zomorph Divide total oral morph<strong>in</strong>e dose by 30 Zomorph 30mg bd = 2mg alfentanil s/c over 24 hours<br />
OxyCodone Divide total oral oxycodone by 15 OxyCont<strong>in</strong>15mg bd =2mg alfentanil s/c over 24 hours<br />
Fentanyl patch<br />
microgram/hour<br />
Standard practice is to leave fentanyl patch on<br />
patient and change every 3 days.<br />
Top up with s/c prn doses <strong>of</strong> alfentanil and review<br />
To calculate prn s/c alfentanil dose to<br />
supplement patch<br />
a)Either divide fentanyl patch strength by 50 to get<br />
prn s/c alfentanil dose ( <strong>in</strong> mg). This is an<br />
approximation and may slightly under estimate<br />
requirements. OR<br />
b)1/6 th <strong>of</strong> equivalent 24 hour alfentanil s/c dose<br />
The prn dose can be given every 2 to 4 hours up to<br />
a maximum <strong>of</strong> 6 prn doses <strong>in</strong> 24 hours<br />
A syr<strong>in</strong>ge driver may be required if 2 or more prn<br />
doses are <strong>use</strong>d.<br />
Subsequent breakthrough dose should be<br />
calculated from the dose <strong>of</strong> alfentanil <strong>in</strong> the syr<strong>in</strong>ge<br />
driver and the equivalent given by patch.<br />
3<br />
Fentanyl patch 75 microgram changed every 72 hours<br />
is approximately equivalent to 9mg alfentanil s/c over 24<br />
hours<br />
Leave patch on and calculate <strong>in</strong>itial prn dose as<br />
a)1/50 th patch strength = 1.5mg OR<br />
b)1/6 th <strong>of</strong> equiv 24 hour alfentanil sc dose 9mg =1.5mg<br />
A syr<strong>in</strong>ge driver may be required if 2 or more doses <strong>use</strong>d<br />
<strong>in</strong> the past 24 hours.<br />
E.g. If 2 prn doses are <strong>use</strong>d (2 x 1.5mg) the syr<strong>in</strong>ge driver<br />
would be set up with 3mg alfentanil over 24 hours<br />
Calculate subsequent prn alfentanil s/c doses<br />
Add alfentanil syr<strong>in</strong>ge driver dose i.e 3mg s/c with<br />
equivalence <strong>of</strong> alfentanil <strong>in</strong> patch i.e 9mg s/c.<br />
Total equivalent 24 hour s/c alfentanil dose = 3mg + 9mg<br />
=12mg<br />
New prn dose would be 1/6 th <strong>of</strong> 12 mg = 2mg<br />
Prn doses will need <strong>in</strong>creas<strong>in</strong>g as syr<strong>in</strong>ge driver<br />
requirements <strong>in</strong>crease<br />
Consult opioid conversion chart on back page<br />
Remember to <strong>in</strong>clude prn doses <strong>in</strong> your calculations
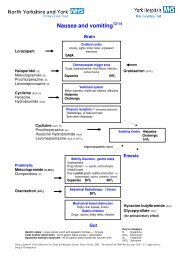
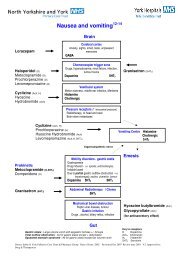
NAUSEA AND VOMITING<br />
4
RESPIRATORY TRACT SECRETIONS<br />
(Remember you cannot clear exist<strong>in</strong>g secretions, but you can help<br />
stop further production)<br />
HYOSCINE BUTYL BROMIDE (BUSCOPAN) occasionally can precipitate when mixed with<br />
CYCLIZINE. If problems discuss with pharmacy.<br />
GLYCOPYRRONIUM may be <strong>use</strong>d as an alternative if Hyosc<strong>in</strong>e Butylbromide not effective (reduced<br />
doses <strong>in</strong> renal failure) See page 41<br />
HYOSCINE HYDROBROMIDE is not recommended <strong>in</strong> patients with renal failure beca<strong>use</strong> <strong>of</strong><br />
excessive drows<strong>in</strong>ess or paradoxical agitation<br />
5
AGITATION / TERMINAL RESTLESSNESS<br />
Yes<br />
Is agitation/ term<strong>in</strong>al<br />
restlessness present <br />
No<br />
Prescribe and adm<strong>in</strong>ster<br />
MIDAZOLAM<br />
2.5 to 5mg s/c every 4 hours<br />
prn<br />
Prescribe<br />
MIDAZOLAM<br />
2.5 to 5mg s/c<br />
every 4 hours prn<br />
(to be adm<strong>in</strong>istered only if the<br />
patient develops symptoms)<br />
Review<br />
every 24 hours<br />
Have more than<br />
2 prn doses been given<br />
<strong>in</strong> 24 hours<br />
No<br />
Yes<br />
Convert to a<br />
syr<strong>in</strong>ge driver<br />
Calculate<br />
amount <strong>of</strong> MIDAZOLAM adm<strong>in</strong>istered<br />
over the last 24 hours and set up a<br />
syr<strong>in</strong>ge driver with this dose<br />
and<br />
2.5 to 5mg s/c every 4 hours prn<br />
Cont<strong>in</strong>ue with<br />
MIDAZOLAM<br />
2.5 to 5mg s/c<br />
every 4 hours prn<br />
Yes<br />
Is the patient’s<br />
agitation controlled<br />
No<br />
Review<br />
every 24 hours<br />
Cont<strong>in</strong>ue with<br />
current<br />
prescription<br />
Increase dose <strong>of</strong><br />
MIDAZOLAM <strong>in</strong> syr<strong>in</strong>ge driver to<br />
maximum <strong>of</strong> 60mg<br />
(30mg <strong>in</strong> renal failure) <strong>in</strong> 24 hours<br />
and<br />
2.5 to 5mg s/c every 4 hours prn<br />
Maximum dose <strong>in</strong> 24 hours is 60mg<br />
(30mg <strong>in</strong> renal failure) which <strong>in</strong>cludes<br />
both prn doses and syr<strong>in</strong>ge driver<br />
Seek advice if more required<br />
If patient still agitated levomepromaz<strong>in</strong>e may be required see page 41 or<br />
contact palliative care team <strong>for</strong> advice<br />
6
DYSPNOEA (BREATHLESSNESS)<br />
(Non renal pathway –see next page <strong>for</strong> patients with renal failure)<br />
Yes<br />
Is the patient<br />
breathless <br />
No<br />
Treat reversible ca<strong>use</strong>s<br />
appropriately and consider<br />
non pharmacological<br />
management such as<br />
position<strong>in</strong>g, cool air,<br />
reassurance<br />
Is the patient already<br />
tak<strong>in</strong>g an opioid (oral or<br />
patch)<br />
No<br />
Prescribe<br />
MORPHINE 3 to 5mg s/c every 4 hours prn<br />
(to be adm<strong>in</strong>istered only if the patient<br />
develops breathlessness)<br />
(If concurrent anxiety consider also prescrib<strong>in</strong>g<br />
MIDAZOLAM 2.5mg s/c every 4 hours prn)<br />
Yes<br />
NB if patient sensitive to morph<strong>in</strong>e <strong>use</strong> alternative –<br />
but note lack <strong>of</strong> evidence <strong>for</strong> other opioids<br />
Use prn doses <strong>for</strong> breathlessness even if not <strong>in</strong> pa<strong>in</strong><br />
Convert to MORPHINE (or alternative opioid)<br />
24 hour s/c <strong>in</strong>fusion us<strong>in</strong>g the opioid conversion table<br />
plus<br />
s/c dose every 4 hours prn<br />
If the patient is on a opioid patch<br />
Leave the patch on and <strong>in</strong>itially top up with prn morph<strong>in</strong>e<br />
or alternative opioid.<br />
If over the next 24 hours 2 or more prn doses are<br />
required set up a 24 hour s/c syr<strong>in</strong>ge driver with<br />
appropriate opioid.<br />
The prn dose <strong>of</strong> morph<strong>in</strong>e (or alternative opioid) <strong>use</strong>d<br />
should take account <strong>of</strong> both the patch and the syr<strong>in</strong>ge<br />
driver<br />
Yes<br />
Have more than<br />
2 prn doses been given<br />
<strong>in</strong> 24 hours<br />
No<br />
Cont<strong>in</strong>ue with<br />
MORPHINE<br />
3 to 5mg s/c every 4 hours prn<br />
+/- MIDAZOLAM<br />
If concurrent anxiety<br />
Consider also prescrib<strong>in</strong>g MIDAZOLAM 2.5mg s/c every 4<br />
hours prn.<br />
If more than 2 prn doses required <strong>in</strong><br />
24 hours put total dose given <strong>in</strong> 24 hours <strong>in</strong>to syr<strong>in</strong>ge<br />
driver<br />
Maximum MIDAZOLAM dose 60mg <strong>in</strong> 24 hours<br />
To calculate the prn dose <strong>of</strong> morph<strong>in</strong>e or<br />
alternative opioid<br />
Prescribe 1/6th <strong>of</strong> the 24 hour dose <strong>in</strong> the syr<strong>in</strong>ge<br />
driver<br />
e.g 20mg morph<strong>in</strong>e s/c via driver over 24 hours<br />
will require<br />
3 to 5mg s/c morph<strong>in</strong>e every 4 hourly prn<br />
7
DYSPNOEA<br />
(Patients with severe renal failure ie GFR < 30mL/m<strong>in</strong>)<br />
Yes<br />
Is the patient<br />
breathless <br />
No<br />
Treat reversible ca<strong>use</strong>s<br />
appropriately and consider<br />
non pharmacological<br />
management such as<br />
position<strong>in</strong>g, cool air,<br />
reassurance<br />
Is the patient already<br />
tak<strong>in</strong>g an opioid (oral or<br />
patch)<br />
No<br />
Prescribe<br />
ALFENTANIL 250 micrograms s/c every 2 to<br />
4 hours prn<br />
(up to a maximum <strong>of</strong> 6 prn doses <strong>in</strong> 24 hours)<br />
(to be adm<strong>in</strong>istered only if the patient<br />
develops breathlessness)<br />
(If concurrent anxiety consider also<br />
prescrib<strong>in</strong>g MIDAZOLAM 2.5mg s/c every 4<br />
hours prn)<br />
Yes<br />
Use prn doses <strong>for</strong> breathlessness even if not <strong>in</strong> pa<strong>in</strong><br />
If patient is already tak<strong>in</strong>g and tolerat<strong>in</strong>g oral<br />
OXYCODONE convert to 24 hour s/c syr<strong>in</strong>ge driver plus<br />
s/c dose every 4 hours prn<br />
Yes<br />
Convert to<br />
syr<strong>in</strong>ge driver<br />
Have more than<br />
2 prn doses been given<br />
<strong>in</strong> 24 hours<br />
OTHERWISE<br />
Convert to ALFENTANIL<br />
24 hour s/c <strong>in</strong>fusion us<strong>in</strong>g the opioid conversion table<br />
plus<br />
s/c dose every 2 to 4 hours prn (up to a maximum <strong>of</strong> 6<br />
prn doses <strong>in</strong> 24 hours)<br />
If the patient is on a opioid patch<br />
Leave the patch on and <strong>in</strong>itially top up with prn alfentanil.<br />
If over the next 24 hours 2 or more prn doses are<br />
required set up a 24 hour s/c syr<strong>in</strong>ge driver with alfentanil<br />
The prn dose <strong>of</strong> alfentanil <strong>use</strong>d should take account <strong>of</strong><br />
both the patch and the syr<strong>in</strong>ge driver<br />
If concurrent anxiety<br />
Consider also prescrib<strong>in</strong>g MIDAZOLAM 2.5mg<br />
s/c every 4 hours prn.<br />
If more than 2 prn doses required <strong>in</strong><br />
24 hours put total dose given <strong>in</strong> 24 hours <strong>in</strong>to syr<strong>in</strong>ge<br />
driver<br />
Maximum MIDAZOLAM dose 30mg <strong>in</strong> 24 hours<br />
No<br />
Cont<strong>in</strong>ue with<br />
ALFENTANIL 250 micrograms s/c<br />
every 2 to 4 hours prn<br />
(up to a maximum <strong>of</strong> 6 prn doses <strong>in</strong> 24 hours)<br />
+/- MIDAZOLAM<br />
To calculate the prn dose <strong>of</strong> alfentanil<br />
Prescribe 1/6th <strong>of</strong> the 24 hour dose<br />
<strong>in</strong> the syr<strong>in</strong>ge driver<br />
e.g 3mg alfentanil s/c via syr<strong>in</strong>ge driver over<br />
24 hours will require<br />
500 micrograms s/c alfentanil<br />
every 2 to 4 hours prn<br />
(up to a maximum <strong>of</strong> 6 prn doses <strong>in</strong> 24 hours)<br />
If symptoms cont<strong>in</strong>ue contact the specialist palliative care<br />
team<br />
Note : Morph<strong>in</strong>e would normally be <strong>use</strong>d <strong>for</strong> breathlessness as this is the opioid which has the best<br />
evidence base <strong>for</strong> treatment <strong>of</strong> breathlessness. In renal impairment however morph<strong>in</strong>e accumulates and<br />
alfentanil or oxycodone is preferred <strong>for</strong> this reason.<br />
8
CHOICE OF DRUGS FOR USE IN SYRINGE DRIVERS<br />
(USUAL DOSE RANGES QUOTED)<br />
If your patient has renal failure look at the cautions <strong>in</strong> red<br />
Drug Use Stat Dose<br />
S/C<br />
Anti emetic<br />
CYCLIZINE<br />
50mg <strong>in</strong> 1ml<br />
HALOPERIDOL<br />
5mg <strong>in</strong> 1ml<br />
METOCLOPRAMIDE<br />
10mg <strong>in</strong> 2ml<br />
LEVOMEPROMAZINE<br />
25mg <strong>in</strong> 1ml<br />
Anti agitation<br />
MIDAZOLAM<br />
10mg <strong>in</strong> 2ml<br />
LEVOMEPROMAZINE<br />
25mg <strong>in</strong> 1ml<br />
Anti secretory<br />
HYOSCINE<br />
BUTYLBROMIDE<br />
20mg <strong>in</strong> 1ml<br />
GLYCOPYRRONIUM<br />
Centrally act<strong>in</strong>g on vomit<strong>in</strong>g<br />
centre.<br />
Good <strong>for</strong> na<strong>use</strong>a associated with<br />
bowel obstruction or <strong>in</strong>creased<br />
<strong>in</strong>tracranial pressure<br />
Dilute with water<br />
Note Dose reduction may be<br />
necessary <strong>in</strong> renal, cardiac or<br />
liver failure e.g. 25mg<br />
Good <strong>for</strong> chemically <strong>in</strong>duced<br />
na<strong>use</strong>a<br />
Antiemetic action<br />
1. Prok<strong>in</strong>etic (accelerates GI<br />
transit)<br />
2. Centrally act<strong>in</strong>g on chemoreceptor<br />
trigger zone (CTZ),<br />
block<strong>in</strong>g transmission to<br />
vomit<strong>in</strong>g centre<br />
Broad spectrum antiemetic, works<br />
on CTZ and vomit<strong>in</strong>g centre (at<br />
lower doses)<br />
Dilute with sodium chloride 0.9%<br />
when <strong>use</strong>d alone<br />
Sedative/anxiolytic (term<strong>in</strong>al<br />
agitation). Also anticonvulsant<br />
and muscle relaxant<br />
Antipsychotic <strong>use</strong>d <strong>for</strong> term<strong>in</strong>al<br />
agitation (2 nd l<strong>in</strong>e to midazolam)<br />
Antisecretory - <strong>use</strong>ful <strong>in</strong> reduc<strong>in</strong>g<br />
respiratory tract secretions.<br />
Has antispasmodic properties<br />
May precipitate when mixed with<br />
cycliz<strong>in</strong>e or haloperidol<br />
Less sedat<strong>in</strong>g than HYOSCINE<br />
HYDROBROMIDE as does not<br />
cross the blood bra<strong>in</strong> barrier<br />
Antisecretory - <strong>use</strong>ful <strong>in</strong> reduc<strong>in</strong>g<br />
respiratory tract secretions<br />
Also has antispasmodic<br />
properties<br />
9<br />
50mg<br />
(25mg <strong>in</strong> patients with<br />
renal/heart/ liver<br />
failure.)<br />
Do not <strong>use</strong> if patient<br />
has two or more <strong>of</strong><br />
above risk factors<br />
1.5mg<br />
May need lower dose <strong>in</strong><br />
elderly/renal failure<br />
0.5mg=500microgram<br />
10mg<br />
(5 to 10mg)<br />
24 hours S/C<br />
dose <strong>in</strong><br />
syr<strong>in</strong>ge driver<br />
(SD)<br />
100 to 150mg<br />
(75 to 100mg <strong>in</strong><br />
renal/heart/liver<br />
failure)<br />
Usual maxm<br />
dose <strong>in</strong><br />
24 hours<br />
(PRN + SD)<br />
150mg<br />
(75 to 100mg <strong>in</strong><br />
renal/heart/liver<br />
failure)<br />
1.5 to 3mg 5mg<br />
30 to 60mg<br />
(30mg <strong>in</strong><br />
renal failure)<br />
120mg<br />
(30mg <strong>in</strong><br />
renal failure)<br />
5 to 6.25mg 5 to 25mg 25mg<br />
2.5 to 5mg<br />
Always start low<br />
For major bleeds <strong>use</strong><br />
10mg<br />
6.25 to 12.5mg<br />
Start with lower dose &<br />
titrate<br />
5 to 60mg<br />
(30mg <strong>in</strong> renal<br />
failure)<br />
Start with lower<br />
dose & titrate<br />
6.25 to 50mg<br />
Seek help with<br />
higher doses<br />
60mg<br />
(30mg <strong>in</strong> renal<br />
failure)<br />
200mg<br />
(25mg to 50mg<br />
<strong>in</strong> renal failure)<br />
20mg 40 to 120mg 240mg<br />
200mcg<br />
(100microgram)<br />
400mcg to<br />
1200microgram<br />
(1.2mg)<br />
(200 to<br />
600microgram)<br />
1200<br />
micrograms<br />
(1.2mg)<br />
(600microgram<br />
<strong>in</strong> renal failure)