Ankle and Foot 47 - Department of Radiology - University of ...
Ankle and Foot 47 - Department of Radiology - University of ...
Ankle and Foot 47 - Department of Radiology - University of ...
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
2208 VII Imaging <strong>of</strong> the Musculoskeletal System<br />
over, displaying the talar <strong>and</strong> calcaneal articular surfaces <strong>of</strong><br />
the posterior, middle, <strong>and</strong> anterior facets <strong>of</strong> the subtalar<br />
joint in red, blue, <strong>and</strong> green, respectively.<br />
The posterior facet is the largest <strong>and</strong> is the primary<br />
weight-bearing portion <strong>of</strong> the subtalar joint. At the anterolateral<br />
corner <strong>of</strong> the posterior facet, the talus comes to an<br />
acutely angled corner, the lateral process <strong>of</strong> the talus. When<br />
the subtalar joint experiences an extreme axial load, such<br />
as when a person falls from a height or undergoes a deceleration<br />
injury in a motor vehicle collision, the pointy<br />
lateral process <strong>of</strong> the talus acts like a wedge, splitting<br />
<strong>and</strong> fracturing the calcaneus. 13 Calcaneal fractures tend to<br />
extend into the posterior facet, <strong>and</strong> when imaging calcaneal<br />
fractures we obliquely angle our coronally reformatted<br />
CT slices to be perpendicular to the posterior facet.<br />
The middle facet is defined by the sustentaculum tali,<br />
a shelflike projection from the anteromedial portion <strong>of</strong> the<br />
calcaneus that supports the middle <strong>of</strong> the talus. Sustentaculum<br />
in Latin means “a supporting structure.” The flexor<br />
hallucis longus tendon passes under the sustentaculum<br />
tali. The middle facet <strong>of</strong> the subtalar joint is a completely<br />
separate articulation from the posterior facet. When injecting<br />
contrast (<strong>of</strong>ten mixed with anesthetic) into the posterior<br />
facet <strong>of</strong> the subtalar joint, we do not expect it to<br />
communicate with the middle facet. Across the middle<br />
facet <strong>of</strong> the subtalar joint is one <strong>of</strong> the two most common<br />
locations for tarsal coalitions to occur, the other being<br />
between the anterior process <strong>of</strong> the calcaneus <strong>and</strong> the<br />
lateral pole <strong>of</strong> the navicular.<br />
Unlike the posterior <strong>and</strong> middle facets, the anterior<br />
facet is not well defined <strong>and</strong> may even be absent. When<br />
present, the anterior facet is a smooth continuation <strong>of</strong> the<br />
middle facet, extending under the head <strong>of</strong> the talus. Directly<br />
lateral to the anterior <strong>and</strong> middle facet is the sinus tarsi, an<br />
area devoid <strong>of</strong> bone <strong>and</strong> filled primarily with fat.<br />
• Anatomic Divisions<br />
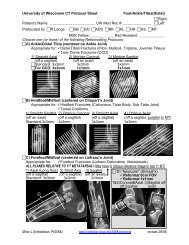
Figure <strong>47</strong>-5 is a three-dimensionally reformatted CT image<br />
showing the anatomic divisions between the tarsals <strong>and</strong><br />
metatarsals. The hindfoot consists <strong>of</strong> the talus <strong>and</strong> the calcaneus<br />
<strong>and</strong> is separated from the midfoot by the Chopart*<br />
joint, a smooth continuation between the talonavicular<br />
<strong>and</strong> calcaneocuboid joints. The midfoot consists <strong>of</strong> the<br />
other five tarsal bones, the navicular, the cuboid, <strong>and</strong> the<br />
three cuneiforms. The forefoot consists <strong>of</strong> the metatarsals<br />
<strong>and</strong> phalanges <strong>and</strong> is separated from the midfoot by the<br />
tarsometatarsal joint, also known as the Lisfranc † joint. Along<br />
Figure <strong>47</strong>-1. Gross anatomy <strong>of</strong> the tarsals <strong>and</strong> surrounding bones.<br />
Ti, tibia; Fi; fibula; Ta, talus; Ca, calcaneus; ST, sustentaculum tali;<br />
N, navicular; Cu, cuboid; 1, 2, <strong>and</strong> 3, refer respectively to the first,<br />
second, <strong>and</strong> third cuneiforms (sometimes referred to as the medial,<br />
intermediate, <strong>and</strong> lateral cuneiforms, respectively); I, II, III, IV, <strong>and</strong> V<br />
refer to the first through fifth metatarsals, respectively.<br />
*François Chopart (1743-1795), a pioneer in urology, was known for the particular<br />
attention he gave to recording his numerous clinical observations. Thus, it<br />
is somewhat surprising that he never wrote about the midtarsal amputation that<br />
bears his name almost three centuries later. He performed this surgery only once,<br />
on August 21, 1791, to resect a presumed liposarcoma <strong>of</strong> the foot. The approach<br />
was based on Chopart’s knowledge <strong>of</strong> the anatomy <strong>of</strong> the midfoot <strong>and</strong> was published<br />
by his student, Laffiteau, in 1792.<br />
† Jacques Lisfranc (1790-18<strong>47</strong>) was a very aggressive surgeon who wrote<br />
extensively <strong>and</strong> described many new procedures, including disarticulation <strong>of</strong> the<br />
shoulder, excision <strong>of</strong> the rectum, <strong>and</strong> amputation <strong>of</strong> the cervix. At age 23 he joined<br />
Napoleon’s army as a battlefront surgeon, a setting where amputations were the<br />
norm. Military surgeons (<strong>of</strong> the period) were not given the calm <strong>and</strong> unhurried<br />
atmosphere necessary for the task <strong>of</strong> laboriously picking out bone splinters <strong>and</strong><br />
bits <strong>of</strong> clothing from gaping wounds. Locating the open ends <strong>of</strong> severed arteries<br />
<strong>and</strong> tying them <strong>of</strong>f in the smoke <strong>of</strong> battle or by flickering c<strong>and</strong>lelight was an enormous<br />
problem. Although some wounds did not themselves dictate amputation, it<br />
<strong>of</strong>ten had to be done because the patient could not otherwise survive the rigors<br />
<strong>of</strong> transport to the rear. The mind did not have time to reason. Experience <strong>and</strong><br />
cold-bloodedness counted for more than talent. Everything had to be done with<br />
prompt <strong>and</strong> decisive action. In 1815, the final year <strong>of</strong> the war, Lisfranc wrote a 50-<br />
page paper describing his technique for performing a partial amputation <strong>of</strong> the<br />
foot at the tarsometatarsal joint, with the sole being preserved to make the flap.<br />
The technique was used to treat forefoot gangrene from frostbite. Lisfranc was<br />
widely known for his ability to amputate a foot in less than a minute, an important<br />
skill in that preanesthesia era.<br />
Ch0<strong>47</strong>-A05375.indd 2208<br />
9/9/2008 5:33:08 PM