Percutaneous cholecystoscopy and internal rendezvous for ... - IJP
Percutaneous cholecystoscopy and internal rendezvous for ... - IJP
Percutaneous cholecystoscopy and internal rendezvous for ... - IJP
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
BRIEF REPORTS<br />
<strong>Percutaneous</strong> <strong>cholecystoscopy</strong> <strong>and</strong> <strong>internal</strong> <strong>rendezvous</strong> <strong>for</strong> removal of<br />
gallstones <strong>and</strong> common bile duct stones (with video)<br />
Eduardo A. Bonin, MD, MSc, Tercio L. Lopes, MD, Todd H. Baron, MD, FASGE<br />
Rochester, Minnesota, USA<br />
Acute cholecystitis may be successfully managed by<br />
cholecystostomy, either temporarily or permanently. 1,2<br />
Concomitant common bile duct (CBD) stones are present<br />
in 14% to 21% of patients. 3,4 We describe a case of cholecystolithiasis<br />
with concomitant choledocholithiasis successfully<br />
treated by percutaneous endoscopic cholelithotomy<br />
<strong>and</strong> <strong>internal</strong> <strong>rendezvous</strong> to allow ERCP <strong>and</strong> CBD<br />
stone removal.<br />
CASE REPORT<br />
A 67-year-old man initially presented with acute calculous<br />
cholecystitis <strong>and</strong> was deemed a nonsurgical c<strong>and</strong>idate<br />
because of severe coronary artery disease with<br />
left main coronary artery stent, ischemic cardiomyopathy,<br />
ventricular tachycardia with implantable cardiodefibrillator,<br />
hypertension, diabetes mellitus, <strong>and</strong> chronic<br />
kidney disease. He was managed with US-guided percutaneous<br />
gallbladder drainage. After clinical improvement,<br />
gallstones were removed percutaneously, although impacted<br />
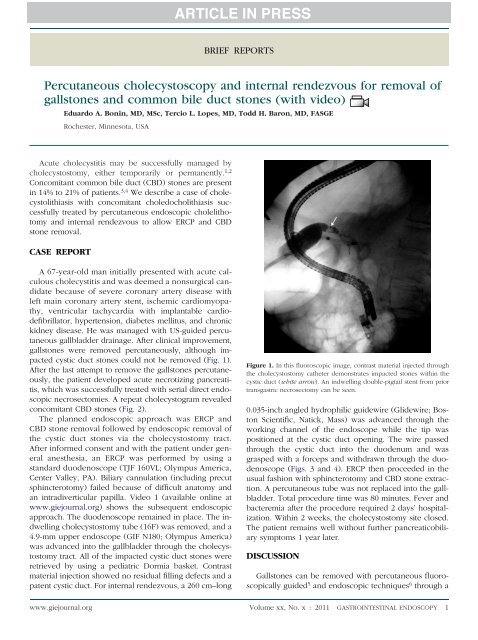
cystic duct stones could not be removed (Fig. 1).<br />
After the last attempt to remove the gallstones percutaneously,<br />
the patient developed acute necrotizing pancreatitis,<br />
which was successfully treated with serial direct endoscopic<br />
necrosectomies. A repeat cholecystogram revealed<br />
concomitant CBD stones (Fig. 2).<br />
The planned endoscopic approach was ERCP <strong>and</strong><br />
CBD stone removal followed by endoscopic removal of<br />
the cystic duct stones via the cholecystostomy tract.<br />
After in<strong>for</strong>med consent <strong>and</strong> with the patient under general<br />
anesthesia, an ERCP was per<strong>for</strong>med by using a<br />
st<strong>and</strong>ard duodenoscope (TJF 160VL; Olympus America,<br />
Center Valley, PA). Biliary cannulation (including precut<br />
sphincterotomy) failed because of difficult anatomy <strong>and</strong><br />
an intradiverticular papilla. Video 1 (available online at<br />
www.giejournal.org) shows the subsequent endoscopic<br />
approach. The duodenoscope remained in place. The indwelling<br />
cholecystostomy tube (16F) was removed, <strong>and</strong> a<br />
4.9-mm upper endoscope (GIF N180; Olympus America)<br />
was advanced into the gallbladder through the cholecystostomy<br />
tract. All of the impacted cystic duct stones were<br />
retrieved by using a pediatric Dormia basket. Contrast<br />
material injection showed no residual filling defects <strong>and</strong> a<br />
patent cystic duct. For <strong>internal</strong> <strong>rendezvous</strong>, a 260 cm–long<br />
Figure 1. In this fluoroscopic image, contrast material injected through<br />
the cholecystostomy catheter demonstrates impacted stones within the<br />
cystic duct (white arrow). An indwelling double-pigtail stent from prior<br />
transgastric necrosectomy can be seen.<br />
0.035-inch angled hydrophilic guidewire (Glidewire; Boston<br />
Scientific, Natick, Mass) was advanced through the<br />
working channel of the endoscope while the tip was<br />
positioned at the cystic duct opening. The wire passed<br />
through the cystic duct into the duodenum <strong>and</strong> was<br />
grasped with a <strong>for</strong>ceps <strong>and</strong> withdrawn through the duodenoscope<br />
(Figs. 3 <strong>and</strong> 4). ERCP then proceeded in the<br />
usual fashion with sphincterotomy <strong>and</strong> CBD stone extraction.<br />
A percutaneous tube was not replaced into the gallbladder.<br />
Total procedure time was 80 minutes. Fever <strong>and</strong><br />
bacteremia after the procedure required 2 days’ hospitalization.<br />
Within 2 weeks, the cholecystostomy site closed.<br />
The patient remains well without further pancreaticobiliary<br />
symptoms 1 year later.<br />
DISCUSSION<br />
Gallstones can be removed with percutaneous fluoroscopically<br />
guided 5 <strong>and</strong> endoscopic techniques 6 through a<br />
www.giejournal.org Volume xx, No. x : 2011 GASTROINTESTINAL ENDOSCOPY 1
Brief Reports<br />
Figure 2. In this fluoroscopic image, contrast material injected through<br />
the cholecystostomy catheter demonstrates bile duct stones (white<br />
arrow).<br />
Figure 4. Schematic drawing depicting successful transcystic <strong>and</strong> transpapillary<br />
guidewire placement. This was achieved by advancing the guidewire into the<br />
cystic <strong>and</strong> bile ducts <strong>and</strong> finally into the duodenum, where it was then grasped<br />
<strong>and</strong> withdrawn through the working channel of the duodenoscope.<br />
DISCLOSURE<br />
T. Baron is a consultant <strong>for</strong> Olympus America. No other<br />
financial relationships relevant to this publication were<br />
disclosed.<br />
Abbreviation: CBD, common bile duct.<br />
REFERENCES<br />
Figure 3. For the <strong>internal</strong> <strong>rendezvous</strong> procedure, a 0.035-inch, hydrophilic<br />
biliary guidewire was advanced into the cystic duct. The guidewire<br />
was passed through the valves of Heister, into the bile duct, then finally<br />
into the duodenum.<br />
mature cholecystostomy tract with technical success rates<br />
of 94% to 96%. 5,6 We per<strong>for</strong>med percutaneous endoscopic<br />
cholecystolithotomy to remove difficult, impacted cystic<br />
duct stones with complete gallbladder clearance. Because<br />
retrograde cannulation was not possible even after precut<br />
papillotomy, an <strong>internal</strong> <strong>rendezvous</strong> through the gallbladder<br />
allowed successful ERCP with clearance of choledocholithiasis.<br />
We are unaware of prior reports of such an<br />
<strong>internal</strong> <strong>rendezvous</strong> technique, which can be useful <strong>for</strong><br />
endoscopically accessing the biliary tree to relieve biliary<br />
obstruction of any etiology <strong>and</strong>/or to treat biliary leaks in<br />
patients with indwelling, mature percutaneous cholecystostomy<br />
tubes.<br />
1. Bakkaloglu H, Yanar H, Guloglu R, et al. Ultrasound guided percutaneous<br />
cholecystostomy in high-risk patients <strong>for</strong> surgical intervention. World J<br />
Gastroenterol 2006;12:7179-82.<br />
2. Morse BC, Smith JB, Lawdahl RB, et al. Management of acute cholecystitis<br />
in critically ill patients: contemporary role <strong>for</strong> cholecystostomy <strong>and</strong> subsequent<br />
cholecystectomy. Am Surg 2010;76:708-12.<br />
3. Coelho JC, Buffara M, Pozzobon CE, et al. Incidence of common bile duct stones<br />
in patients with acute <strong>and</strong> chronic cholecystitis. Surg Gynecol Obstet 1984;158:<br />
76-80.<br />
4. Chiarugi M, Galatioto C, Lippolis PV, et al. Simultaneous laparoscopic<br />
treatment <strong>for</strong> common bile duct stones associated with acute cholecystitis:<br />
results of a prospective study [Italian]. Chir Ital 2006;58:709-16.<br />
5. Kim YH, Kim YJ, Shin TB. Fluoroscopy-guided percutaneous gallstone removal<br />
using a 12-fr sheath in high-risk surgical patients with acute cholecystitis.<br />
Korean J Radiol 2011;12:210-5.<br />
6. Ohashi S. <strong>Percutaneous</strong> transhepatic cholecystoscopic lithotomy in the managementofacutecholecystitiscausedbygallbladderstones.DiagnTherEndosc<br />
1998;5:19-29.<br />
Department of Medicine, Division of Gastroenterology & Hepatology, Mayo<br />
Clinic, Rochester, Minnesota, USA.<br />
Reprint requests: Todd H. Baron, MD, 200 First Street SW, Rochester, MN 55905.<br />
Copyright © 2011 by the American Society <strong>for</strong> Gastrointestinal Endoscopy<br />
0016-5107/$36.00<br />
doi:10.1016/j.gie.2011.07.074<br />
2 GASTROINTESTINAL ENDOSCOPY Volume xx, No. x : 2011 www.giejournal.org