Invasive breast carcinoma - IARC
Invasive breast carcinoma - IARC
Invasive breast carcinoma - IARC
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
Macroscopy<br />
Fisher et al. reported that invasive papillary<br />
<strong>carcinoma</strong> is grossly circumscribed<br />
in two-thirds of cases {879}. Other invasive<br />
papillary <strong>carcinoma</strong>s are gro s s l y<br />
indistinguishable from invasive bre a s t<br />
cancers of no special type.<br />
Histopathology<br />
Of the 1,603 <strong>breast</strong> cancers reviewed in<br />
the NSABP-B04 study, 38 had papillary<br />
f e a t u res, and all but 3 of these were<br />
" p u re," without an admixture of other histologic<br />
types {879}. Micro s c o p i c a l l y,<br />
expansile invasive papillary carc i n o m a s<br />
a re characteristically circ u m s c r i b e d ,<br />
show delicate or blunt papillae, and show<br />
focal solid areas of tumour growth. The<br />
cells typically show amphophillic cytoplasm,<br />
but may have apocrine feature s ,<br />
and also may exhibit apical "snouting" of<br />
cytoplasm similar to tubular carc i n o m a .<br />
The nuclei of tumour cells are typically<br />
i n t e rmediate grade, and most tumours<br />
a re histologic grade 2 {879}. Tumour stroma<br />
is not abundant in most cases, and<br />
occasional cases show prominent extracellular<br />
mucin production. Calcifications,<br />
although not usually evident mammog<br />
r a p h i c a l l y, are commonly seen histologi<br />
c a l l y, but usually are present in associated<br />
DCIS. DCIS is present in more than<br />
75% of cases, and usually, but not exclus<br />
i v e l y, has a papillary pattern. In rare<br />
lesions in which both the invasive and in<br />
situ components have papillary feature s ,<br />
it may be difficult to determine the re l a t i v e<br />
p ro p o rtion of each. Lymphatic vessel<br />
invasion has been noted in one third of<br />
cases. Microscopic involvement of skin or<br />
nipple was present in 8 of 35 cases<br />
(23%), but Paget disease of the nipple<br />
was not observed {879}.<br />
E s t rogen receptor positivity was observed<br />
in all 5 cases of invasive papillary<br />
c a rcinoma examined in one study, and<br />
p ro g e s t e rone receptor positivity in 4 of 5<br />
(80%) {2351}. In a review of cytogenetic<br />
findings in 5 examples of invasive papill<br />
a ry <strong>carcinoma</strong>, 60% exhibited re l a t i v e l y<br />
simple cytogenetic abnormalities {40}. In<br />
addition, none of the 4 examples of papi<br />
l l a ry <strong>carcinoma</strong>s examined in two re c e n t<br />
re p o rts were associated with either TP53<br />
p rotein accumulation or ERBB2 oncoprotein<br />
overe x p ression {2440,2750}.<br />
Clinical course and prognosis<br />
T h e re are only limited data on the pro g-<br />
nostic significance of invasive papillary<br />
A<br />
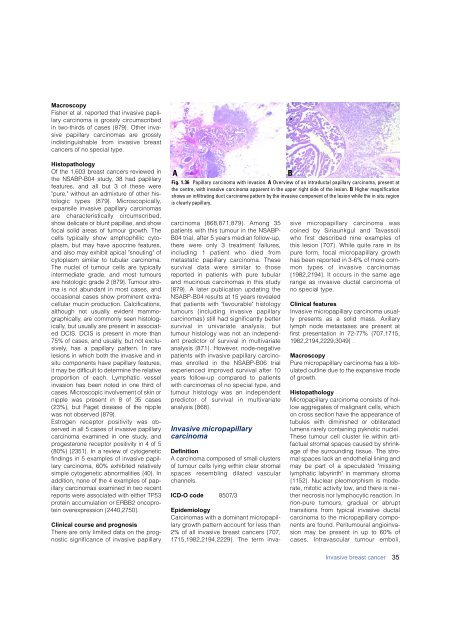
Fig. 1.36 Papillary <strong>carcinoma</strong> with invasion. A Overview of an intraductal papillary <strong>carcinoma</strong>, present at<br />
the centre, with invasive <strong>carcinoma</strong> apparent in the upper right side of the lesion. B Higher magnification<br />
shows an infiltrating duct <strong>carcinoma</strong> pattern by the invasive component of the lesion while the in situ region<br />
is clearly papillary.<br />
c a rcinoma {868,871,879}. Among 35<br />
patients with this tumour in the NSABP-<br />
B04 trial, after 5 years median follow-up,<br />
t h e re were only 3 treatment failure s ,<br />
including 1 patient who died fro m<br />
metastatic papillary <strong>carcinoma</strong>. These<br />
survival data were similar to those<br />
re p o rted in patients with pure tubular<br />
and mucinous <strong>carcinoma</strong>s in this study<br />
{879}. A later publication updating the<br />
NSABP-B04 results at 15 years re v e a l e d<br />
that patients with "favourable" histology<br />
tumours (including invasive papillary<br />
c a rcinomas) still had significantly better<br />
survival in univariate analysis, but<br />
tumour histology was not an independent<br />
predictor of survival in multivariate<br />
analysis {871}. However, node-negative<br />
patients with invasive papillary carc i n o-<br />
mas enrolled in the NSABP-B06 trial<br />
experienced improved survival after 10<br />
years follow-up compared to patients<br />
with <strong>carcinoma</strong>s of no special type, and<br />
tumour histology was an independent<br />
p redictor of survival in multivariate<br />
analysis {868}.<br />
<strong>Invasive</strong> micropapillary<br />
<strong>carcinoma</strong><br />
Definition<br />
A <strong>carcinoma</strong> composed of small clusters<br />
of tumour cells lying within clear stromal<br />
spaces resembling dilated vascular<br />
channels.<br />
ICD-O code 8507/3<br />
B<br />
Epidemiology<br />
C a rcinomas with a dominant micro p a p i l-<br />
l a ry growth pattern account for less than<br />
2% of all invasive <strong>breast</strong> cancers {707,<br />
1715,1982,2194,2229}. The term invasive<br />
micro p a p i l l a ry <strong>carcinoma</strong> was<br />
coined by Siriaunkgul and Ta v a s s o l i<br />
who first described nine examples of<br />
this lesion {707}. While quite rare in its<br />
p u re form, focal micro p a p i l l a ry gro w t h<br />
has been re p o rted in 3-6% of more common<br />
types of invasive carc i n o m a s<br />
{1982,2194}. It occurs in the same age<br />
range as invasive ductal <strong>carcinoma</strong> of<br />
no special type.<br />
Clinical features<br />
<strong>Invasive</strong> micropapillary <strong>carcinoma</strong> usually<br />
presents as a solid mass. Axillary<br />
lymph node metastases are present at<br />
first presentation in 72-77% {707,1715,<br />
1982,2194,2229,3049} .<br />
Macroscopy<br />
Pure micropapillary <strong>carcinoma</strong> has a lobulated<br />
outline due to the expansive mode<br />
of growth.<br />
Histopathology<br />
Micropapillary <strong>carcinoma</strong> consists of hollow<br />
aggregates of malignant cells, which<br />
on cross section have the appearance of<br />
tubules with diminished or obliterated<br />
lumens rarely containing pyknotic nuclei.<br />
These tumour cell cluster lie within artifactual<br />
stromal spaces caused by shrinkage<br />
of the surrounding tissue. The stromal<br />
spaces lack an endothelial lining and<br />
may be part of a speculated "missing<br />
lymphatic labyrinth" in mammary stroma<br />
{1152}. Nuclear pleomorphism is moderate,<br />
mitotic activity low, and there is neither<br />
necrosis nor lymphocytic reaction. In<br />
n o n - p u re tumours, gradual or abrupt<br />
transitions from typical invasive ductal<br />
<strong>carcinoma</strong> to the micropapillary components<br />
are found. Peritumoural angioinvasion<br />
may be present in up to 60% of<br />
cases. Intravascular tumour emboli,<br />
<strong>Invasive</strong> <strong>breast</strong> cancer<br />
35