Slides - University of Utah - School of Medicine
Slides - University of Utah - School of Medicine
Slides - University of Utah - School of Medicine
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
WHAT ABOUT THE<br />
PATIENT-CENTERED<br />
MEDICAL HOME AND<br />
YOUR PRACTICE IN<br />
2013?<br />
Leslie Lenert MD<br />
Associate Chair for Quality and Innovation<br />
Department <strong>of</strong> <strong>Medicine</strong><br />
<strong>University</strong> <strong>of</strong> <strong>Utah</strong> Health Care System<br />
What can we<br />
do to get ready<br />
for Medical<br />
Homes and<br />
Accountable<br />
Care<br />
Organizations?
THE PROBLEM WITH PRIMARY<br />
CARE<br />
Time for chronic disease<br />
care for an average<br />
patient panel:<br />
- 10 hours per day<br />
Time for preventative<br />
care an average panel:<br />
- 7.4 hours per day<br />
Proportion <strong>of</strong><br />
recommended care<br />
received by patients:<br />
-! 55%
THE ARCHETYPE FOR PRIMARY CARE<br />
REMAINS IN THE ROCKWELL ERA<br />
We like it this way and people are willing to pay<br />
for this type <strong>of</strong> personal attention<br />
(e.g., Concierge or Retainer <strong>Medicine</strong>)
PARADIGM SHIFT:<br />
PRIMARY CARE AS A SYSTEM<br />
!"#$%&'(')$*+',-'./012345+'*26256'5)$5'(')$*+'57'$88719:26)';+723>'57'69+3C'1%'C$%'5=%23>'57'1$#+'1%'9$3+:'7)'7='A)7')$*+3J5')$C'$'<br />
)+17>:7;23'I.8'23'5)+'9$65'%+$=&'E+'$=+'>723>'57'8735$85'5)+6+'9+79:+&'E+'$=+'>723>'<br />
57';=23>'5)+1'23'$=C'<br />
57'5)+2='8)=7328'C26+$6+D'5)+%J=+'>723>'57'1++5'A25)'$'34=6+'A)7')$6'$'9)%6282$30<br />
A=2K+3'9=75787:'$6'57')7A'57'238=+$6+'5)+2='1+C28$F736'57'>+5'5)+2='64>$=6';$8#'<br />
43C+='8735=7:&?'<br />
Thomas Bodenheimer<br />
4
MEDICAL HOME MODEL<br />
Payment Reform<br />
(pay for episode <strong>of</strong><br />
care, for<br />
coordination <strong>of</strong> care)<br />
Enhanced Access<br />
(email, extend<br />
hours, decision aids)<br />
Personal<br />
Physician<br />
Quality and Safety<br />
(evidence based medicine<br />
perspective, use <strong>of</strong> IT to<br />
facilitate quality and<br />
assessment <strong>of</strong> quality)<br />
Physician Directed Care<br />
(practice team led by physician)<br />
Whole Person<br />
Orientation<br />
Integration<br />
(bring together all<br />
services needed to<br />
address a medical<br />
issue)<br />
5
MEDICAL HOME DESIDERATA<br />
!! Personal physician.<br />
!! Each patient has an ongoing relationship with a personal physician who is trained<br />
to provide first contact, continuous and comprehensive care.<br />
!! Physician-directed medical practice.<br />
!! The personal physician leads a team <strong>of</strong> individuals at the practice level who<br />
collectively take responsibility for ongoing patient care.<br />
!! Whole-person orientation.<br />
!! The personal physician is responsible for providing all <strong>of</strong> the patient’s health care<br />
needs or for arranging care with other qualified pr<strong>of</strong>essionals.<br />
!! Care is coordinated and integrated<br />
!! across all elements <strong>of</strong> the complex health care system and the patient’s<br />
community.<br />
!! Quality and safety are hallmarks<br />
!! Enhanced access to care<br />
!! Open scheduling, expanded hours and other innovative options for communication<br />
between patients, their personal physician and practice staff.<br />
!! Payment recognizes the added value<br />
!! Practices that achieve NCQA’s PCMH Recognition are positioned to take<br />
advantage <strong>of</strong> financial incentives
PCMH is a high level<br />
strategy to change<br />
the structure <strong>of</strong> primary care<br />
Cost neutral<br />
(Reductions in<br />
ED and<br />
Hospitalization)<br />
Only feasible with cooperation<br />
payers and health delivery systems<br />
Raise income<br />
levels and<br />
supply <strong>of</strong><br />
primary care<br />
providers<br />
Continue to<br />
reimburse for<br />
services<br />
Viable<br />
primary<br />
care<br />
Add<br />
reimbursement for<br />
episodes <strong>of</strong> care<br />
and pay for<br />
performance<br />
Add<br />
reimbursement for<br />
coordination <strong>of</strong><br />
care<br />
7
WHY FOCUS ON THE MEDICAL HOME<br />
MODEL<br />
!! Improve patient experience<br />
!! Improve quality <strong>of</strong> care<br />
!! Reduce costs <strong>of</strong> care<br />
!! Address issues with lack <strong>of</strong> satisfaction with practice, viability<br />
<strong>of</strong> primary care as a specialty<br />
!! Address income gap between specialists and primary care<br />
physicians
HEALTHCARE IS A COMPLEX<br />
ADAPTIVE SYSTEM
WHAT THIS MIGHT (EVENTUALLY)<br />
MEAN FOR PHYSICIANS…<br />
!! Team leadership role may predominate over personal<br />
physician role<br />
!! Larger panel sizes in some models (more team<br />
leadership);<br />
!! Smaller panel sizes in other models (more personal care<br />
at a cost)<br />
!! High severity <strong>of</strong> illness practices<br />
!! Retainer practices<br />
!! Empowerment for responsibility for patient outcomes<br />
•! Payment for population health management and care<br />
coordination services<br />
•! At risk payment (Accountable Care Organizations)
OVERLAP BETWEEN PCMH AND ACO’S<br />
!! Accountable Care Organizations (ACO) are provider-based<br />
organizations that take responsibility for meeting the health<br />
care needs <strong>of</strong> a defined population, with the goal <strong>of</strong><br />
simultaneously improving health, improving patient<br />
experience and reducing per capita costs.<br />
!! ! Determine and update care coordination needs<br />
!! ! Create a a plan <strong>of</strong> care<br />
!! ! Communicate<br />
!! ! between health pr<strong>of</strong>essionals and family<br />
! !! within teams teams <strong>of</strong> health pr<strong>of</strong>essionals<br />
! !! Across health care settings<br />
! !! Facilitate transitions<br />
ACO<br />
! !! Connect with community resources<br />
! !! Align resources to population needs<br />
PCMH
EFFECT ON QUALITY/OUTCOMES/COSTS<br />
!! Wide evidence that PCMH improves quality metrics<br />
Benefits <strong>of</strong> Implementing the Primary Care Patient- Centered Medical Home. Patient Centered Primary Care Collaborative<br />
!! Early evidence that it improves outcomes<br />
!! Geisinger: PCMH participation reduced patients risk <strong>of</strong> amputation<br />
and renal failure. American Journal <strong>of</strong> Medical Quality 2012 27: 210<br />
!! Some evidence it reduces costs<br />
!! UMPC: -$15 PMPM HEALTH AFFAIRS 31, NO. 11 (2012): 2423–2431<br />
!! Geisinger: -4% costs <strong>of</strong> care, ROI = ~1 Am J Manag Care. 2012;18(3):149-155)<br />
!! Group Health: - $10 PMPM HEALTH AFFAIRS 29, NO. 5 (2010): 835-843
PCMH EFFECTS: OTHER VARIABLES<br />
!! Operational costs increased by PMCH<br />
!! $2 per PMPM cost for 10% gain in PCMH features JAMA. 2012;308(1):60-66<br />
!! $6 PMPM total for UPMC pilot HEALTH AFFAIRS 31, NO. 11 (2012): 2423–2431<br />
!! Total PCMH score not associated with patient satisfaction<br />
Health Services Research DOI: 10.1111/j.1475-6773.2012.01429.x<br />
!! Total PCMH score in Safety-Net clinics associated with<br />
!! Improved provider and staff morale<br />
!! Improved clinic staff job satisfaction<br />
!! Less risk <strong>of</strong> burn out symptoms in providers<br />
Arch Intern Med 2012;172(1):23-31
COMMON PROBLEMS WITH PCMH AS<br />
SEEN BY PHYSICIANS ADOPTING IT<br />
The Policy Context <strong>of</strong> Patient Centered Medical Homes:<br />
Perspectives <strong>of</strong> Primary Care Providers<br />
J Gen Intern Med DOI: 10.1007/s11606-012-2135-0
NCQA MEDICAL HOME CERTIFICATION<br />
!! PPC-1: Written standards for<br />
patient access and communication<br />
!! PPC-1b: Use <strong>of</strong> data to show<br />
standards for patient access and<br />
communication are met<br />
!! PCC-2D: Use <strong>of</strong> paper or electronic<br />
tools to organize clinical<br />
information<br />
!! PPC-2E: Use <strong>of</strong> data to identify<br />
important diagnoses and conditions<br />
in practice.<br />
!! PPC-3A: Adoption and<br />
implementation <strong>of</strong> evidence-based<br />
guidelines for three conditions.<br />
Level 1: 50% <strong>of</strong> items<br />
Level 2 or 3: 100% <strong>of</strong> items<br />
!! PPC-4B: Active support <strong>of</strong> patient<br />
self management<br />
!! PPC-6A: System tracking <strong>of</strong> tests<br />
and follow up <strong>of</strong> test results<br />
!! PPC-7A: System tracking <strong>of</strong> critical<br />
referrals<br />
!! PPC-8A: Measurement <strong>of</strong> clinical<br />
and/or service performance<br />
!! PPC-8C: Performance reporting by<br />
physicians across the practice
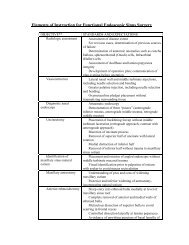
Medical-Home<br />
Capacities<br />
Improved access and<br />
communication<br />
Use <strong>of</strong> data systems to<br />
enhance safety and<br />
reliability<br />
Care management and<br />
coordination<br />
Support for patient selfcare<br />
Performance reporting<br />
and improvement<br />
How Capacities Are Measured in NCQA Certification<br />
Program<br />
Have written standards for key components <strong>of</strong> access and<br />
communication (4 points) and use data to document how standards<br />
are met (5). Assess language preference and communication<br />
barriers (2). (Total: 11 points)<br />
Use data system for nonclinical (2) and clinical (6) information to<br />
track patients’ diagnoses (4) and clinical status (6) and to generate<br />
reminders (3). Track referrals (4) and laboratory results<br />
systematically (7). Use electronic system to order, retrieve, and flag<br />
tests (6); write prescriptions (3) and check their safety (3) and cost<br />
(2); and improve safety and communication (4). (Total: 50 points)<br />
Adopt and implement evidence-based guidelines (3) and use<br />
reminders for preventive services (4). Coordinate care with other<br />
providers (5) and use non physician staff to manage patient care (3).<br />
(Total: 15 points)<br />
Develop individualized patient care plans, which assess progress<br />
and address barriers to achieving plan goals (5). Actively support<br />
patient self-care (4). (Total: 9 points)<br />
Measure (3) and report performance to physicians in the practice (3)<br />
using standardized measures (2). Report performance externally (1).<br />
Survey patients about their experience (3). Set goals and take action
WHAT CAN WE DO TO MOVE TOWARD THE<br />
MEDICAL HOME MODEL TODAY?<br />
!! Micro level efforts (you and your patient)<br />
!! Develop patient oriented goals and care plans<br />
!! Activate patients and measure activation<br />
!! Learn how to lead health care teams<br />
!! Meso level efforts (organization <strong>of</strong> your clinic)<br />
!! Written clinic policy development for medical home certification<br />
!! Practice guidelines <strong>of</strong> conditions (pathways), tracking diagnostic test<br />
orders as well as results<br />
!! Panel management efforts<br />
!! Macro level (fitting into the health system)<br />
!! Retainer medicine practices<br />
!! ACO development
Initial<br />
<strong>of</strong>fice<br />
visit<br />
Time<br />
Lab<br />
visit<br />
Lab<br />
check<br />
EXAMPLE OF A CARE PLAN<br />
Pharmacy<br />
Rx Pick up<br />
Home<br />
BP monitoring<br />
Follow<br />
up call<br />
Lab<br />
visit<br />
Return<br />
visit<br />
“Plan: After checking a chemistry panel, we’ll start and ACE<br />
inhibitor for hypertension. The patient will check his blood pressure<br />
at home and we’ll call after two weeks to evaluate if he needs a dose<br />
change. In 6 weeks he will return for a follow visit with a fasting lipid panel”
Measure Patient Activation (PAM)<br />
Four stages <strong>of</strong> activation:<br />
1.! Believes active role is<br />
important<br />
2.! Confidence and<br />
knowledge to take action<br />
3.! Taking action<br />
4.! Staying the course<br />
under stress<br />
ED visits vs. activation<br />
•! Stage 1: 24.1<br />
•!<br />
•!<br />
Stage 2: 20.4<br />
Stage 3: 17.9<br />
P
LEARN HOW TO LEAD HEALTH CARE<br />
TEAMS<br />
Shared Values<br />
!! Honesty: Put a high value on open<br />
communication within the team, including<br />
transparency about aims, decisions,<br />
uncertainty, and mistakes.<br />
!! Discipline. Carry out roles and responsibilities<br />
even when inconvenient, and seek out and<br />
share information to improve even when it is<br />
uncomfortable.<br />
!! Creativity: Be excited by the possibility <strong>of</strong><br />
tackling new or emerging problems, seeing<br />
errors and unanticipated bad outcomes as<br />
potential opportunities to learn and improve.<br />
!! Humility: Recognize differences in training but<br />
do not believe that 1 type <strong>of</strong> training or<br />
perspective is uniformly superior; recognize<br />
that team members are human and will make<br />
mistakes.<br />
!! Curiosity: Delight in seeking out and reflecting<br />
on lessons learned and using those insights for<br />
continuous improvement.<br />
Principles<br />
!! Clear Roles: Have clear expectations for each<br />
member’s functions, responsibilities, and<br />
accountabilities.<br />
!! Mutual Trust: Earn each other’s trust,<br />
creating strong norms <strong>of</strong> reciprocity and<br />
greater opportunities for shared<br />
achievement.<br />
!! Effective Communication: Prioritize and<br />
continuously refine communication skills<br />
using consistent channels for candid and<br />
complete communication.<br />
!! Shared Goals: Work to establish shared goals<br />
that reflect patient and family priorities and<br />
that can be clearly articulated, understood,<br />
and supported by all members.<br />
!! Measurable Processes and Outcomes: Agree<br />
on and implement timely feedback on<br />
successes and failures in both the overall<br />
functioning <strong>of</strong> the team and achievement <strong>of</strong><br />
specific goals.
MESOSTRATEGIES FROM GROUP HEALTH<br />
COOPERATIVE<br />
!! Virtual medicine<br />
!! Secure email messaging and telephone<br />
encounters<br />
!! Chronic care management<br />
!! Use <strong>of</strong> electronic registries, health maintainece reminders, best<br />
practice alerts<br />
!! Collaborative care plans<br />
!! Self management resources, group visits, peer led workshops<br />
!! Visit preparation<br />
!! Patients contacted in advance <strong>of</strong> visits to clarify concerns and<br />
expectations<br />
!! Patient outreach<br />
!! Outreach and follow up for all discharges, ED visits and urgent care<br />
visits
PERSONNEL STRUCTURE OF A MEDICAL HOME<br />
PRACTICE<br />
Typical Medical<br />
Office Staff<br />
•!Medical Assistant<br />
•!Biller<br />
•!Scheduler<br />
•!Office manager<br />
•!Nurse call manager<br />
ICC2F73$:'65=4854=+'
!! Order sets<br />
for common conditions<br />
USING YOUR EHR<br />
!! Test and consult<br />
completion
CHANGE IS HARD<br />
•!Transformation to a PCMH “requires epic whole-practice reimagination<br />
and redesign. It is much more than a series <strong>of</strong><br />
incremental changes”<br />
•!Technology needed in a PCMH is not "plug and play.” The<br />
hodge-podge <strong>of</strong> information technology marketed to primary<br />
care practices resembles more a pile <strong>of</strong> jigsaw pieces than<br />
components <strong>of</strong> an integrated and interoperable system.
MEDICAL HOME ALTERNATIVES<br />
!! Retainer <strong>Medicine</strong><br />
!! Growing popularity<br />
!! Per member – Per month fee provides access to additional resources<br />
and limits panel sizes<br />
!! Fees vary from $50 per month to $200 to ???<br />
!! Panel size 600-1200<br />
!! Allows personal attention and care coordination<br />
!! Improves income or generates similar income with less effort<br />
!! May reduce other costs<br />
!! MDVIP members have 50% less utilization <strong>of</strong> hospital care<br />
!! Rarely readmitted for MI, CHF, CAP (90% less <strong>of</strong>ten)<br />
Personalized Preventive Care Leads to Significant Reductions in Hospital Utilization<br />
Am J Manag Care. 2012;18(12):e453-e460<br />
!! Difficult to fully adjust for effects <strong>of</strong> SES in this study
SUMMARY/CONCLUSIONS<br />
!! Patient Centered Medical Home in 2013<br />
!! New model for care<br />
!! Transformatory but change is hard<br />
!! Requires payer interest/participation<br />
!! Evidence is growing for effects on<br />
!! Quality <strong>of</strong> care ++++<br />
!! Costs <strong>of</strong> care ++<br />
!! Patient experience +/–<br />
!! Physician burnout ++<br />
!! Primary care salaries ?<br />
!! Cost <strong>of</strong> transformation<br />
!! $6-10 PMPM<br />
!! IT integration is critical<br />
!! Focus <strong>of</strong> the practice is on<br />
!! execution <strong>of</strong> plans (as opposed to orders)<br />
!! Behavioral change<br />
Is it for me?