accp-seek board review question of the month
accp-seek board review question of the month
accp-seek board review question of the month
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
A 78-year-old<br />
<strong>accp</strong>-<strong>seek</strong> <strong>board</strong> <strong>review</strong> <strong>question</strong><br />
<strong>of</strong> <strong>the</strong> <strong>month</strong><br />
ICU Admission for Anterior Myocardial<br />
Infarction With Shortness <strong>of</strong> Breath*<br />
Steven M. Hollenberg, MD, FCCP<br />
(CHEST 2004; 125:1577–1578)<br />
woman is admitted to <strong>the</strong> ICU with<br />
an anterior myocardial infarction. She is treated<br />
with aspirin, thrombolytic <strong>the</strong>rapy, and nitrates. Her<br />
clinical course is uneventful until <strong>the</strong> third hospital<br />
day, when she has sudden onset <strong>of</strong> shortness <strong>of</strong><br />
breath. Her BP is 95/55 mm Hg, pulse rate is 124<br />
beats/min, and respiratory rate is 32 breaths/min.<br />
Cardiovascular examination reveals jugular venous<br />
*From <strong>the</strong> ACCP-SEEK program, reprinted with permission.<br />
Items are selected by Department Editors Richard S. Irwin, MD,<br />
FCCP, and John G. Weg, MD, FCCP. For additional information,<br />
phone 1-847-498-1400.<br />
Reproduction <strong>of</strong> this article is prohibited without written permission<br />
from <strong>the</strong> American College <strong>of</strong> Chest Physicians (e-mail:<br />
permissions@chestnet.org).<br />
Correspondence to: Steven M. Hollenberg, MD, FCCP, Cooper<br />
Hospital, Division <strong>of</strong> Cardiology, 366 Dorrance, One Cooper<br />
Plaza, Camden, NJ 08103; e-mail: hollenberg-steven@<br />
cooperhealth.edu<br />
distention, s<strong>of</strong>t heart sounds, and a pansystolic murmur.<br />
She has bibasilar crackles. A chest radiograph<br />
shows pulmonary edema. Her ECG shows sinus<br />
tachycardia and an evolving anterior myocardial infarction.<br />
A pulmonary artery ca<strong>the</strong>ter is inserted, and<br />
<strong>the</strong> following readings are obtained: right atrium<br />
pressure, 6 mm Hg (56% O 2 saturation); right<br />
ventricular pressure, 40/6 mm Hg (55% O 2 saturation);<br />
pulmonary artery pressure, 40/23 mm Hg<br />
(mean, 30 mm Hg; 57% O 2 saturation); pulmonary<br />
artery occlusion pressure, 24 mm Hg (v waves to 40);<br />
and cardiac output, 3.5 L/min. Which <strong>of</strong> <strong>the</strong> following<br />
is most appropriate at this time?<br />
A. Pericardiocentesis<br />
B. Mitral value surgery<br />
C. Repeat thrombolytic <strong>the</strong>rapy<br />
D. Cardiac ca<strong>the</strong>terization and angioplasty<br />
E. Surgical repair <strong>of</strong> <strong>the</strong> ventricular septum<br />
www.chestjournal.org CHEST / 125 /4/APRIL, 2004 1577
Answer: B. Mitral value surgery<br />
Acute mitral regurgitation after myocardial infarction<br />
presents with pulmonary edema and cardiogenic<br />
shock. The presence <strong>of</strong> a new holosystolic murmur,<br />
along with a large v wave on <strong>the</strong> pulmonary artery<br />
occlusion tracing, is diagnostic <strong>of</strong> this complication.<br />
Ischemic mitral regurgitation is more commonly associated<br />
with inferior myocardial infarction and ischemia<br />
or infarction <strong>of</strong> <strong>the</strong> posterior papillary muscle, but can<br />
occur with anterior infarction, particularly in patients<br />
with multivessel disease. In <strong>the</strong> presence <strong>of</strong> cardiogenic<br />
shock, <strong>the</strong> pansystolic murmur can be s<strong>of</strong>t or inaudible<br />
above <strong>the</strong> pulmonary edema, and may be limited to<br />
early systole because <strong>of</strong> rapid equalization <strong>of</strong> pressures<br />
in <strong>the</strong> left atrium and left ventricle.<br />
Rupture <strong>of</strong> <strong>the</strong> interventricular septum can be<br />
difficult to distinguish clinically from acute mitral<br />
regurgitation due to papillary muscle rupture; in<br />
both, patients have a systolic murmur, and large v<br />
waves in <strong>the</strong> pulmonary artery occlusion tracing may<br />
be seen with septal rupture due to high pulmonary<br />
flow. With septal rupture, however, <strong>the</strong>re is a step-up in<br />
oxygenation from <strong>the</strong> right atrium to <strong>the</strong> right ventricle<br />
<strong>of</strong> 5% due to left-to-right shunting. Because <strong>the</strong>re is<br />
no step-up in <strong>the</strong> patient described in this <strong>question</strong>,<br />
option E is incorrect. Pump failure due to reocclusion<br />
<strong>of</strong> <strong>the</strong> infarct artery is a possible cause <strong>of</strong> cardiogenic<br />
shock after myocardial infarction, but most cases <strong>of</strong><br />
shock due to pump failure develop in <strong>the</strong> first 24 h, and<br />
nei<strong>the</strong>r <strong>the</strong> v wave nor <strong>the</strong> murmur is characteristic.<br />
Thus, options C and D, measures to re-establish pa-<br />
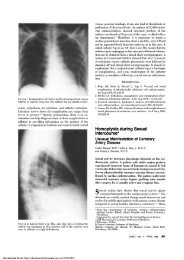
Figure 1. Echocardiographic image <strong>of</strong> a ruptured papillary muscle.<br />
tency <strong>of</strong> an occluded artery, are incorrect. Pericardial<br />
tamponade (option A) can result from rupture <strong>of</strong> <strong>the</strong><br />
left ventricular free wall and lead to shock after myocardial<br />
infarction, but <strong>the</strong> hemodynamic pr<strong>of</strong>ile is<br />
characterized by elevation and equalization <strong>of</strong> intracardiac<br />
pressure not seen in our patient.<br />
Echocardiography is <strong>of</strong>ten useful to diagnose<br />
acute mitral regurgitation after myocardial infarction,<br />
and can rule out o<strong>the</strong>r causes <strong>of</strong> acute decompensation<br />
such as free wall rupture, tamponade, and<br />
pump failure. An echocardiographic image <strong>of</strong> a<br />
ruptured papillary muscle is shown in <strong>the</strong> accompanying<br />
Figure 1 (arrow). Management includes afterload<br />
reduction with nitroprusside and intra-aortic<br />
balloon pumping as temporizing measures. Inotropic<br />
or vasopressor <strong>the</strong>rapy may be needed to support<br />
cardiac output and BP. Definitive <strong>the</strong>rapy, however,<br />
is surgical valve repair or replacement, which should<br />
be undertaken as soon as possible because clinical<br />
deterioration can be sudden.<br />
Selected Readings<br />
Bolooki H. Emergency cardiac procedures in patients in cardiogenic<br />
shock due to complications <strong>of</strong> coronary artery disease.<br />
Circulation 1989; 79: I-137–I-148<br />
Hollenberg SM, Kavinsky CJ, Parrillo JE. Cardiogenic shock.<br />
Ann Intern Med 1999; 131:47–59<br />
Khan SS, Gray RJ. Valvular emergencies. Cardiol Clin 1991;<br />
9:689–709<br />
Meister SG, Helfant RH. Rapid bedside differentiation <strong>of</strong> ruptured<br />
interventricular septum from acute mitral insufficiency.<br />
N Engl J Med 1972; 287:1024–1025<br />
1578 ACCP-SEEK Board Review Question <strong>of</strong> <strong>the</strong> Month