Mental Health Nursing
Mental Health Nursing
Mental Health Nursing
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
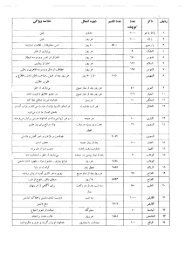
Table 8.1 Four levels of observation detailed in SNMAC practice<br />
guidance (reproduced with kind permission from the DoH)<br />
Four levels of observation<br />
Observation 171<br />
In order to facilitate communication, care planning and training, the following classification<br />
in the level of observation is recommended:<br />
Level I. General observation is the minimum acceptable level of observation for all<br />
in-patients. The location of all patients should be known to staff, but not all patients need to<br />
be kept within sight. At least once a shift a nurse should sit down and talk with each<br />
patient to assess their mental state. This interview should always include an evaluation<br />
of the patient’s mood and behaviours associated with risk and should be recorded in<br />
the notes.<br />
Level II. Intermittent observation means that the patient’s location must be checked every 15<br />
to 30 minutes (exact times to be specified in the notes). This level is appropriate when<br />
patients are potentially, but not immediately, at risk. Patients with depression, but no immediate<br />
plans to harm themselves or others, or patients who have previously been at risk of harm<br />
to self or others, but who are in a process of recovery, require intermittent observation.<br />
Level III. Within eyesight is required when the patient could, at any time, make an attempt<br />
to harm themselves or others. The patient should be kept within sight at all times, by day<br />
and night and any tools or instruments that could be used to harm self or others should be<br />
removed. It may be necessary to search the patients and their belongings whilst having<br />
due regard for patients’ legal rights.<br />
Level IV. Within arm’s length: patients at the highest levels of risk of harming themselves<br />
or others, may need to be nursed in close proximity. On rare occasions more than one<br />
nurse may be necessary. Issues of privacy, dignity and consideration of the gender in allocating<br />
staff, and the environmental dangers, need to be discussed and incorporated into<br />
the care plan.<br />
The four levels detailed by the SNMAC report are not based upon<br />
‘evidence’ as such, as they have not been evaluated. They are instead<br />
recommended as guidance to local services in England and Wales, intended<br />
to provide a template for local policies. However, local trusts and hospitals<br />
are not required in any legal sense to adopt these levels in their<br />
entirety, and therefore it is likely that there remains great variation in the<br />
terminology and detail of observation levels used in different places.<br />
Partly this may still be due to poor awareness of the report itself, or trusts<br />
only incorporating elements of the SNMAC guidance rather in its entirety.<br />
Second, organisations often need more than recommended guidance to<br />
change practice, which is embedded in the culture of individual wards and<br />
clinical teams.<br />
It is important to note the differences between the guidance issued for<br />
Scotland and the SNMAC guidance for England and Wales. In Scotland,<br />
the CRAG/SCOTMEG (1995) Good Practice Statement, which has been<br />
adopted in a number of Scottish trusts (Porter et al., 1998), has just three<br />
levels of observation: General Observation; Constant Observation; and