Maxillomandibular Advancement Surgery in a Site-Specific ...
Maxillomandibular Advancement Surgery in a Site-Specific ...
Maxillomandibular Advancement Surgery in a Site-Specific ...
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
<strong>Maxillomandibular</strong> <strong>Advancement</strong><br />
<strong>Surgery</strong> <strong>in</strong> a <strong>Site</strong>-<strong>Specific</strong> Treatment<br />
Approach for Obstructive Sleep Apnea<br />
<strong>in</strong> 50 Consecutive Patients*<br />
Jeffrey R. Pr<strong>in</strong>sell, DMD, MD<br />
Objective: To report the efficacy of maxillomandibular advancement (MMA) surgery, with a<br />
description of several <strong>in</strong>novations, as a site-specific treatment of obstructive sleep apnea<br />
syndrome (OSAS) <strong>in</strong> selected cases with disproportionate velo-orohypopharyngeal anatomy.<br />
Design: Cl<strong>in</strong>ical series of 50 consecutive cases.<br />
Sett<strong>in</strong>g: <strong>Surgery</strong> was performed <strong>in</strong> a hospital operat<strong>in</strong>g room, and perioperative management was<br />
provided <strong>in</strong> an <strong>in</strong>tensive care environment. Except for polysomnography (PSG), which was<br />
performed and <strong>in</strong>terpreted by <strong>in</strong>dependent sleep facilities/physicians, all pre- and postoperative<br />
evaluations were accomplished <strong>in</strong> a solo office private practice sett<strong>in</strong>g.<br />
Patients: Patients were referred for MMA evaluation when applicable conservative therapies such<br />
as nasal cont<strong>in</strong>uous positive airway pressure (nCPAP) were not tolerated, refused, or unsuccessful.<br />
Case selection was based primarily on the sites of disproportionate upper airway anatomy.<br />
Interventions: MMA consisted of a Lefort I osteotomy, bilateral sagittal split ramus osteotomies, and<br />
a new modified procedure called an anterior <strong>in</strong>ferior mandibular osteotomy with <strong>in</strong>direct hyoid<br />
suspension. Some patients also received concomitant adjunctive nonpharyngeal procedures.<br />
Measurements and results: Obta<strong>in</strong>ed at a mean of 5.2 months postoperatively, revealed significant<br />
improvement <strong>in</strong> all cases. Mean BPs (n 50) were lowered, subjective symptoms were ameliorated,<br />
and mean body mass <strong>in</strong>dex (n 50) was reduced. Cephalometric analysis (n 50), with several new<br />
modifications <strong>in</strong>clud<strong>in</strong>g standardization for phases of respiration, quantified structural changes <strong>in</strong><br />
soft-tissue and bony landmarks. Postoperative PSG results (n 50) showed dramatic improvement<br />
over preoperative data (n 50), with therapeutic values similar to nCPAP (n 42). Mean values<br />
improved from preoperative to postoperative vs nCPAP for apnea <strong>in</strong>dex (34.5 to 1.0 vs 2.0,<br />
respectively), apnea-hypopnea <strong>in</strong>dex (59.2 to 4.7 vs 5.4, respectively), lowest arterial oxyhemoglob<strong>in</strong><br />
desaturations (72.7% to 88.6% vs 88.6%, respectively), and number of desaturations < 90% (118.8 to<br />
6.6 vs 2.4, respectively). The success rate was 100%.<br />
Conclusion: MMA is highly successful and safe and may be a def<strong>in</strong>itive primary s<strong>in</strong>gle-staged surgical<br />
treatment of selected OSAS cases with diffusely complex or multiple sites of disproportionate<br />
velo-orohypopharyngeal anatomy. (CHEST 1999; 116:1519–1529)<br />
Key words: cephalometric; maxillomandibular advancement; obstructive sleep apnea; polysomnography; site-specific surgery<br />
Abbreviations: AHI apnea-hypopnea <strong>in</strong>dex; AI apnea <strong>in</strong>dex; AIMO anterior <strong>in</strong>ferior mandibular osteotomy;<br />
BMI body mass <strong>in</strong>dex; BSSRO bilateral sagittal split ramus osteotomies; EDS excessive daytime sleep<strong>in</strong>ess;<br />
ETT endotracheal tube; ETV end-tidal volume; GO-POG gonion to pogonion; LF Lefort I osteotomy;<br />
LSAT lowest arterial oxyhemoglob<strong>in</strong> desaturation; MM modified Müller maneuver; MMA maxillomandibular advancement;<br />
MMO maxillomandibular osteotomies; MP-H mandibular plane to hyoid; nCPAP nasal cont<strong>in</strong>uous<br />
positive airway pressure; OSA obstructive sleep apnea; OSAS obstructive sleep apnea syndrome; PAS posterior airway<br />
space; PNS-P length of soft palate from posterior nasal sp<strong>in</strong>e to uvula tip; PSG polysomnography; SNA sella nasion<br />
po<strong>in</strong>t A angle; SNB sella nasion po<strong>in</strong>t B angle; T/A tonsillectomy and/or adenoidectomy; UA upper airway;<br />
UPPP uvulopalatopharyngoplasty<br />
Obstructive sleep apnea syndrome (OSAS) 1 is a<br />
potentially life-threaten<strong>in</strong>g medical disorder2–4 with a projected prevalence of up to 18 million<br />
*From Jeffrey R. Pr<strong>in</strong>sell, DMD, MD, 1950 Spectrum Circle,<br />
Suite B-300, Marietta, GA.<br />
Manuscript received December 14, 1998; revision accepted June<br />
23, 1999.<br />
Correspondence to: Jeffrey R. Pr<strong>in</strong>sell, DMD, MD, 1950 Spectrum<br />
Circle, Suite B-300 Marietta, GA 30067; e-mail: drpr<strong>in</strong>sell@<br />
m<strong>in</strong>dspr<strong>in</strong>g.com<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013<br />
people <strong>in</strong> the U.S. population alone. 5 OSAS results<br />
from repetitive collapse of the soft tissues that form<br />
or lie <strong>in</strong>to or adjacent to the lumen of the supraglot-<br />
For editorial comment see page 1503<br />
tic or upper airway (UA), while asleep. These pharyngeal<br />
soft tissues are suspended and supported by<br />
the cartilag<strong>in</strong>ous and bony skeletal structures of the<br />
CHEST / 116 /6/DECEMBER, 1999 1519
lower face and upper neck. UA patency dur<strong>in</strong>g sleep<br />
is dependent on a complex <strong>in</strong>terplay of anatomic and<br />
physiologic factors. The balance of constrict<strong>in</strong>g<br />
forces, eg, negative <strong>in</strong>spiratory <strong>in</strong>tralum<strong>in</strong>al suction<br />
generated by the diaphragm, and dilat<strong>in</strong>g forces of<br />
the pharyngeal musculature 6,7 is dysfunctional <strong>in</strong><br />
obstructive sleep apnea (OSA). 8 Reduction <strong>in</strong> activity<br />
of the tensor palat<strong>in</strong>i 9 and genioglossus 8,10 muscles<br />
may contribute to flopp<strong>in</strong>ess and collapsibility of an<br />
elongated soft palate <strong>in</strong> the velopharynx and a bulky<br />
retropositioned tongue base <strong>in</strong> the orohypopharynx,<br />
respectively. Efforts to enhance neuromuscular control<br />
of the abnormal pharyngeal dilator muscles with<br />
medications 11,12 and nerve stimulators 13,14 have been<br />
largely unsuccessful. More conventional OSA therapies<br />
seek to improve or correct abnormalities of the<br />
pharyngeal anatomic structure or physiologic function.<br />
15<br />
Comprehensive evaluation and treatment plann<strong>in</strong>g<br />
of OSAS cases requires a multidiscipl<strong>in</strong>ary team<br />
approach. The universal convenience of nasal cont<strong>in</strong>uous<br />
positive airway pressure (nCPAP) is that it<br />
pneumatically spl<strong>in</strong>ts open the entire UA with a high<br />
degree of therapeutic efficacy, 16,17 elim<strong>in</strong>at<strong>in</strong>g the<br />
need to identify specific site(s) of obstruction. However,<br />
not all OSAS patients are compliant with its<br />
required lifetime of nightly use, caused primarily by<br />
<strong>in</strong>tolerance. 18–23 Other devices, eg, oral appliances, 24,25<br />
are therapeutic only if selected appropriately for the<br />
specific site(s) of UA obstruction, which may vary<br />
among different <strong>in</strong>dividuals 26,27 ; and also may have<br />
compliance problems with habitual use while asleep.<br />
Although it is known that weight reduction may<br />
lessen OSA, 28 it is unknown what degree of weight<br />
loss is required. OSAS also occurs <strong>in</strong> nonobese<br />
patients. 29 Noncompliance is a common problem <strong>in</strong><br />
that many patients have difficulty los<strong>in</strong>g weight or<br />
ma<strong>in</strong>ta<strong>in</strong><strong>in</strong>g weight loss. 30,31<br />
It is generally accepted that surgery is <strong>in</strong>dicated<br />
when applicable conservative therapies are unsuccessful<br />
or not tolerated, and for patients with an underly<strong>in</strong>g<br />
specific surgically correctable abnormality that is caus<strong>in</strong>g<br />
the OSAS. 32 <strong>Surgery</strong> can provide def<strong>in</strong>itive treatment<br />
and, thus, elim<strong>in</strong>ate issues of patient compliance,<br />
but only if performed competently, both <strong>in</strong> terms of<br />
technical skill, as well as on the “correct” area(s) of UA<br />
obstruction. Although many surgical procedures and<br />
protocols are reported, 33 maxillomandibular advancement<br />
(MMA), which “pulls forward” the anterior pharyngeal<br />
tissues attached to the maxilla, mandible, and<br />
hyoid to enlarge the entire velo-orohypopharynx 34 with<br />
m<strong>in</strong>imal risks of edema-<strong>in</strong>duced UA embarrassment or<br />
pharyngeal dysfunction, is the most effective, exclud<strong>in</strong>g<br />
tracheostomy, acceptable surgical treatment of OSAS,<br />
with success rates of 95%, 34 96%, 35 and 98%. 36<br />
Nevertheless, the <strong>in</strong>dications for MMA rema<strong>in</strong><br />
unsettled, eg, it is often limited to severe cases of<br />
OSAS when other surgeries have failed, partly because<br />
of exist<strong>in</strong>g diagnostic dilemmas such as identify<strong>in</strong>g<br />
and rank<strong>in</strong>g, <strong>in</strong> terms of severity, the often<br />
multiple sites of obstruction, and know<strong>in</strong>g when and<br />
how to prioritize and comb<strong>in</strong>e surgical procedures <strong>in</strong><br />
one or more stages, 33,36,37 which may be <strong>in</strong>fluenced<br />
and perhaps biased by the surgeon’s education,<br />
tra<strong>in</strong><strong>in</strong>g, and experience. The primary purpose of<br />
this case series is to report the efficacy of MMA,<br />
often with concomitant adjunctive nonpharyngeal<br />
procedures, as a treatment of OSAS <strong>in</strong> a site-specific<br />
approach: the methodology for the selection of specific<br />
surgical procedures was not specialty- or stagespecific,<br />
but rather, based on each <strong>in</strong>dividual patient’s<br />
sites of disproportionate UA anatomy.<br />
Materials and Methods<br />
Presurgical Evaluation and Treatment Plann<strong>in</strong>g<br />
Patients were evaluated for MMA only if (1) they exhibited<br />
OSAS diagnosed by <strong>in</strong>dependent nocturnal polysomnography<br />
(PSG) (<strong>in</strong>clusion criteria of an apnea-hypopnea <strong>in</strong>dex [AHI] 15<br />
or an apnea <strong>in</strong>dex [AI] 5 and a lowest arterial oxyhemoglob<strong>in</strong><br />
desaturation [LSAT] 90%) that was cl<strong>in</strong>ically significant (<strong>in</strong>clusion<br />
criteria of stated excessive daytime sleep<strong>in</strong>ess [EDS]); (2)<br />
all applicable conservative therapies (eg, nCPAP, weight loss,<br />
positional therapy, reduction of late even<strong>in</strong>g sedative-hypnotic<br />
medications or alcoholic beverages, oral appliances or other<br />
devices) or prior surgical procedures were unsuccessful, not<br />
tolerated, or refused, as determ<strong>in</strong>ed by the referr<strong>in</strong>g sleep<br />
physician(s); and (3) they were medically stable and will<strong>in</strong>g to<br />
proceed with surgery.<br />
Presurgical evaluations were performed by the author <strong>in</strong> a<br />
s<strong>in</strong>gle office. Detailed head and neck exam<strong>in</strong>ation was performed<br />
cl<strong>in</strong>ically and radiographically, us<strong>in</strong>g posterior-anterior panoramic<br />
and lateral cephalometric radiographs (described below).<br />
Cephalometric prediction trac<strong>in</strong>gs and photographic computer<br />
imag<strong>in</strong>g (Everex; United Digital Systems, Inc.; W<strong>in</strong>ston-Salem,<br />
NC) were used to illustrate proposed changes <strong>in</strong> UA size and<br />
facial appearance, respectively. Body weights were measured<br />
with a foot scale, and BP was recorded with the patients sitt<strong>in</strong>g<br />
us<strong>in</strong>g a digital BP monitor (Labron; Hauppauge, NY) with a<br />
full-sized arm cuff and with a paper pr<strong>in</strong>tout. Patients’ OSASrelated<br />
symptoms were recorded on a standard screen<strong>in</strong>g questionnaire<br />
form. Hospital medical staff credential<strong>in</strong>g for surgical<br />
privileges for all procedures performed (Table 1) and written<br />
<strong>in</strong>formed consent for all patients were obta<strong>in</strong>ed.<br />
Surgical treatment plann<strong>in</strong>g was “site-specific”: The selection<br />
of specific surgical procedures was <strong>in</strong>dividualized for each patient,<br />
based on their specific site(s) of disproportionate UA<br />
anatomy. The most severe sites were addressed first, with the<br />
hypopharynx as the area of most critical concern. MMA <strong>in</strong>clusion<br />
criterion was orohypopharyngeal narrow<strong>in</strong>g caused by macroglossia<br />
with a retropositioned tongue base—determ<strong>in</strong>ed by cl<strong>in</strong>ical<br />
exam<strong>in</strong>ation and measured by cephalometric analysis (posterior<br />
airway space [PAS] 9 mm at end-tidal volume [ETV]), described<br />
below. Macroglossia was def<strong>in</strong>ed cl<strong>in</strong>ically as an enlarged<br />
tongue base that, at rest, extended above the horizontal plane of<br />
the mandibular dentition. Velopharyngeal narrow<strong>in</strong>g, by cepha-<br />
1520 Cl<strong>in</strong>ical Investigations<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013
Table 1—Surgical Procedures<br />
Procedure<br />
lometry, 34 was also treated with MMA, but only if coexistent with<br />
orohypopharyngeal narrow<strong>in</strong>g. Nonpharyngeal sites coexistent<br />
with velo-orohypopharyngeal narrow<strong>in</strong>g were treated with adjunctive<br />
procedures (described <strong>in</strong> “Surgical Techniques”) performed<br />
concomitantly with MMA. Patients with sites <strong>in</strong> the<br />
absence of orohypopharyngeal narrow<strong>in</strong>g did not receive MMA,<br />
but rather received other procedures and, therefore, were excluded<br />
from this cl<strong>in</strong>ical series. Pharyngeal soft-tissue surgery<br />
(discussed <strong>in</strong> “Surgical Pr<strong>in</strong>ciples and Rationale”) was not performed<br />
concomitantly with MMA.<br />
All MMA patients <strong>in</strong>cluded <strong>in</strong> this series had diffusely complex<br />
or multiple sites of disproportionate UA anatomy that <strong>in</strong>cluded<br />
orohypopharyngeal narrow<strong>in</strong>g, characterized by macroglossia<br />
with a retropositioned tongue base and constricted PAS. Although<br />
certa<strong>in</strong> congenital craniofacial skeletal deformities, eg,<br />
retrognathia, may <strong>in</strong>fluence or predispose to OSA, 38,39 some<br />
MMA patients exhibited normal craniofacial skeletal morphology.<br />
Some had septal deviation, turb<strong>in</strong>ate hypertrophy, anterior mandibular<br />
l<strong>in</strong>gual tori, and/or thick necks with cervicofacial lipomatosis.<br />
Many also displayed encroachment of the lateral pharyngeal<br />
walls because of medially displaced tonsillar pillars associated<br />
with dysmorphic soft palates and, less commonly, tonsillar hypertrophy.<br />
Tonsillectomy and/or adenoidectomy (T/A) had been<br />
performed earlier, usually as a child, <strong>in</strong> 26 patients, and uvulopalatopharyngoplasty<br />
(UPPP) had been performed before MMA<br />
<strong>in</strong> 10 patients. For those patients who had failed prior surgery<br />
(Table 1), the basel<strong>in</strong>e data described above, <strong>in</strong>clud<strong>in</strong>g diagnostic<br />
PSG, were obta<strong>in</strong>ed after prior surgery before proceed<strong>in</strong>g with<br />
MMA.<br />
Lateral Cephalometric Analysis<br />
Prior to<br />
MMA*<br />
Concomitant<br />
With MMA<br />
MMA<br />
LF 0 50<br />
BSSRO 0 50<br />
AIMO 0 50<br />
Septoplasty 9 28<br />
Turb<strong>in</strong>ate reduction 5 26<br />
Cervicofacial lipectomy 1 26<br />
Maxillary s<strong>in</strong>us surgery 0 13<br />
Mandibular l<strong>in</strong>gual tori removal 0 1<br />
T/A 26 0<br />
UPPP 10 0<br />
Tracheostomy 2 0<br />
*Basel<strong>in</strong>e (pre-MMA) diagnostic data (PSG, BP, weight, symptoms, and<br />
cephalometry) were obta<strong>in</strong>ed after these prior surgical procedures.<br />
Lateral cephalometric radiographs were obta<strong>in</strong>ed us<strong>in</strong>g an<br />
Oralix Pan DC III (model PT-11 P/C; Orion Corporation,<br />
Soredex, Hels<strong>in</strong>ki, F<strong>in</strong>land for Philips Medical Systems, Inc.<br />
Shelton, CT) with wedge filter screens for tissue enhancement<br />
and clarity. To m<strong>in</strong>imize variances <strong>in</strong> magnification, head position,<br />
and neck flexion, all films were obta<strong>in</strong>ed at a 5-ft x-ray<br />
source distance with the awake patients stand<strong>in</strong>g with head<br />
secured <strong>in</strong> a cephalostat and look<strong>in</strong>g straight ahead with a<br />
radiopaque level taped to the temporal region. Volumetric<br />
lum<strong>in</strong>al pharyngeal changes associated with different phases of<br />
respiration were standardized by obta<strong>in</strong><strong>in</strong>g two films: the first at<br />
ETV and the second dur<strong>in</strong>g a modified Müller maneuver (MM).<br />
Acetate trac<strong>in</strong>gs with measurements of soft and bony tissue<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013<br />
landmarks of all preoperative and postoperative cephalographs were<br />
made. Figure 1 illustrates a cephalometric trac<strong>in</strong>g with several new<br />
modifications of measurements described previously by others.<br />
33,36,40–44 PAS was measured as the shortest horizontal l<strong>in</strong>e<br />
drawn perpendicular to the anterior and posterior pharyngeal walls<br />
at the most narrow level, rather than simply an extension of a straight<br />
l<strong>in</strong>e connect<strong>in</strong>g po<strong>in</strong>t B to gonion. Length of the soft palate from<br />
posterior nasal sp<strong>in</strong>e to the uvula tip (PNS-P) and hyoid position<br />
below the mandibular plane (MP-H), as well as PAS, were recorded<br />
at both ETV and MM. Gonion to pogonion (GO-POG) was used as<br />
a direct l<strong>in</strong>ear measurement of absolute mandibular length, <strong>in</strong><br />
addition to sella nasion po<strong>in</strong>t B angle (SNB), which is an angular<br />
measurement of anterior mandibular position <strong>in</strong> relation to the<br />
cranial base. Maxillary advancement was measured by sella nasion<br />
po<strong>in</strong>t A angle (SNA). Although only PAS at ETV was used as an<br />
MMA <strong>in</strong>clusion criterion, all of these cephalometric measurements<br />
were used to quantify the amount of: maxillary (SNA), mandibular<br />
(SNB), and genial (GO-POG) advancement; soft palatal (PNS-P)<br />
and hyoid (MP-H) suspension; as well as orohypopharyngeal enlargement<br />
(PAS).<br />
PSG<br />
Although there were several referr<strong>in</strong>g physicians associated<br />
with different facilities, each patient had both their pre- and<br />
postoperative PSG performed and <strong>in</strong>terpreted <strong>in</strong>dependently by<br />
the same respective facility. Although different types of <strong>in</strong>strumentation<br />
were used, all stated their PSG methods were <strong>in</strong><br />
accordance with conventional criteria, as described elsewhere. 45<br />
Obstructive apnea and hypopnea were def<strong>in</strong>ed as a cessation and<br />
dim<strong>in</strong>ishment, respectively, of airflow, despite respiratory effort,<br />
for 10 s.<br />
Surgical Pr<strong>in</strong>ciples and Rationale<br />
MMA (Figs 2 and 3) opens the velo-, oro-, and hypopharynx 34<br />
by “pull<strong>in</strong>g forward” the anterior pharyngeal soft-tissue compo-<br />
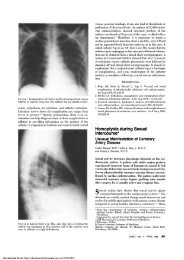
Figure 1. Lateral cephalometric analysis. Measurements obta<strong>in</strong>ed<br />
were SNA, 82 2°; SNB, 80 2°; PNS-P, 35 3 mm;<br />
PAS, 11 1 mm; MP-H, 15 2 mm; and GO-POG, 84 5 mm.<br />
CHEST / 116 /6/DECEMBER, 1999 1521
Figure 2. Lateral cephalometric prediction of MMA.<br />
nents, which are attached to the maxilla, mandible, and hyoid.<br />
Mandibular advancement pulls forward the tongue base and<br />
suprahyoid muscles attached to the genial tubercles and the<br />
anterior <strong>in</strong>ferior mandible to open the orohypopharynx. Maxillary<br />
advancement anterosuperiorly tightens the soft palate, which is<br />
suspended from the palat<strong>in</strong>e bone of the maxilla, to open the<br />
velopharynx and, thus, may obviate surgery of the soft palatal<br />
tissues.<br />
The soft palate is a tissue organ whose known primary function<br />
is to prevent reflux of air and liquids <strong>in</strong>to the nasopharynx dur<strong>in</strong>g<br />
speech and swallow<strong>in</strong>g, respectively. Also, its role <strong>in</strong> snor<strong>in</strong>g may<br />
Figure 3. MMA.<br />
be a warn<strong>in</strong>g sign or “bell” (to the bed partner) of partial or<br />
impend<strong>in</strong>g UA obstruction, which may progress to OSA. A<br />
dysmorphic or abnormal-look<strong>in</strong>g soft palate may be an anatomic<br />
variant of normal, which ensures compensatory function<strong>in</strong>g; and<br />
may not always be a cause of OSAS. Retropalatal narrow<strong>in</strong>g and<br />
collapse, often <strong>in</strong>duced by swallow<strong>in</strong>g, eg, dur<strong>in</strong>g nasopharyngolaryngoscopy,<br />
should be understood as normal velopharyngeal<br />
closure, rather than perhaps mis<strong>in</strong>terpreted as a site of obstruction<br />
dictat<strong>in</strong>g surgery. A long or bulky soft palate does not<br />
necessarily mandate a UPPP, 46 laser-assisted uvuloplasty, 47 palatopharyngoglossoplasty,<br />
48 uvulopalatopharyngoglossoplasty, 49<br />
somnoplasty (Somnus Medical Technologies Inc; Sunnyvale,<br />
CA), or radiofrequency volumetric tissue reduction. 50 Surgical<br />
ablation or distortion may produce dysfunction (eg., velopharyngeal<br />
<strong>in</strong>sufficiency, 51–53 nasopharyngeal stenosis, 51 voice changes,<br />
51 or dysphagia 52,53 ) and, <strong>in</strong> cases of snor<strong>in</strong>g amelioration, may<br />
produce silent apnea 47 —either of immediate or delayed onset<br />
with advanc<strong>in</strong>g age and/or weight ga<strong>in</strong>. Soft palatal surgery may<br />
also produce severe pa<strong>in</strong>, hemorrhage, 51–54 and UA obstruction<br />
<strong>in</strong> the immediate postoperative period because of velopharyngeal<br />
edema that, particularly if compounded with coexist<strong>in</strong>g untreated<br />
hypopharyngeal narrow<strong>in</strong>g, can result <strong>in</strong> death. 51,52,54<br />
MMA not only preserves the functional <strong>in</strong>tegrity of the pharyngeal<br />
tissues but also m<strong>in</strong>imizes the risk of worsened OSA <strong>in</strong><br />
the immediate postoperative period because m<strong>in</strong>imal edema<br />
occurs with<strong>in</strong> the unoperated pharyngeal soft tissues. The edema<br />
result<strong>in</strong>g from the <strong>in</strong>traoral labial vestibular MMA <strong>in</strong>cisions is<br />
physiologically shielded from the UA by the underly<strong>in</strong>g bony<br />
structures and, thus, is conf<strong>in</strong>ed to the facial soft tissues. Although<br />
this extraosseous edema may produce pronounced facial<br />
swell<strong>in</strong>g, it does not extend to or compromise the UA, which is<br />
more patent at the moment of skeletal advancement, ie, like the<br />
immediate UA open<strong>in</strong>g produced by a cardiopulmonary resuscitation<br />
jaw-thrust maneuver. Furthermore, rigidly fixated MMA<br />
osteotomy segments, unlike pharyngeal soft tissues that are<br />
operated on, do not move and, therefore, are not pa<strong>in</strong>ful dur<strong>in</strong>g<br />
the normal functions of swallow<strong>in</strong>g, cough<strong>in</strong>g, and vocalization.<br />
Maxillary and mandibular branches of the trigem<strong>in</strong>al (sensory)<br />
nerve, encased with<strong>in</strong> bony canals, that <strong>in</strong>nervate the <strong>in</strong>traoral<br />
and lower facial tissues are typically surgically traumatized or<br />
stretched, result<strong>in</strong>g <strong>in</strong> numbness, rather than severe pa<strong>in</strong>.<br />
The primary functions of the maxilla and mandible, speech<br />
articulation and mastication, are determ<strong>in</strong>ed by their <strong>in</strong>terrela-<br />
1522 Cl<strong>in</strong>ical Investigations<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013
tionship and enhanced by a harmonious dental occlusion. Except<br />
for isolated mandibular horizontal deficiency 55 with severe class<br />
II malocclusion characterized by pronounced <strong>in</strong>cisal overjet<br />
(none seen <strong>in</strong> this series), mandibular advancement requires<br />
synchronous maxillary advancement to ma<strong>in</strong>ta<strong>in</strong> a functional<br />
occlusion. Orthodontic therapy was performed <strong>in</strong> four patients to<br />
decompensate severely recumbent maxillary <strong>in</strong>cisors to maximize<br />
mandibular advancement. However, <strong>in</strong> most patients with malocclusions<br />
who refused orthodontics, as well as <strong>in</strong> the patients<br />
with relatively normal occlusions, the maxilla and mandible were<br />
advanced the same amounts, ma<strong>in</strong>ta<strong>in</strong><strong>in</strong>g the same presurgical<br />
occlusal relationship.<br />
Adjunctive nonpharyngeal surgical procedures (described under<br />
“Surgical Techniques”) were performed concomitantly with<br />
MMA because these additional sites could be operated on safely<br />
with m<strong>in</strong>imal risk of postoperative edema-<strong>in</strong>duced airway embarrassment.<br />
T/A, UPPP, laser-assisted uvuloplasty, palatopharyngoglossoplasty,<br />
uvulopalatopharyngoglossoplasty, radiofrequency<br />
volumetric tissue reduction, laser midl<strong>in</strong>e glossectomy, 56 or l<strong>in</strong>gualplasty<br />
57 could conceivably be performed with MMA, but only<br />
if immediate tracheostomy, endotracheal tube (ETT) <strong>in</strong>tubation,<br />
or nCPAP or bilevel pressure ventilation were to be used for<br />
several days dur<strong>in</strong>g the resolution of postoperative pharyngeal<br />
edema. In this latter situation it would be difficult to know what<br />
pressures would be therapeutic—possibly requir<strong>in</strong>g a cont<strong>in</strong>uous<br />
titration, eg, auto-adjust<strong>in</strong>g cont<strong>in</strong>uous positive airway pressure—<br />
with <strong>in</strong>creased risk of hemorrhage 51–54,56,57 caused by barotrauma<br />
of the recently operated on pharyngeal tissues. Thus, pharyngeal<br />
soft-tissue surgery was not attempted simultaneously with MMA.<br />
Surgical Techniques<br />
The author, always assisted by another surgeon, operated on all<br />
patients with hypotensive general anesthesia <strong>in</strong> a hospital operat<strong>in</strong>g<br />
room. A Lefort I osteotomy (LF) with allogeneic bone graft<br />
and rigid <strong>in</strong>ternal fixation us<strong>in</strong>g custom-bent bone plates was<br />
performed for maxillary advancement with anterosuperior tighten<strong>in</strong>g<br />
of the soft palate and to enlarge the velopharynx. Bilateral<br />
sagittal split ramus osteotomies (BSSRO) with rigid <strong>in</strong>ternal<br />
and/or maxillomandibular fixation was performed for mandibular<br />
advancement. An anterior <strong>in</strong>ferior mandibular osteotomy<br />
(AIMO) was performed for additional advancement of the genial<br />
tubercles with attached tongue-related (eg, genioglossus) and<br />
suprahyoid muscles for additional advancement of the tongue<br />
base and an <strong>in</strong>direct hyoid suspension. The AIMO is a separate<br />
and dist<strong>in</strong>ct osteotomy, performed via <strong>in</strong>cisions not connected<br />
with the BSSRO. Nevertheless, BSSRO and AIMO together are<br />
additive <strong>in</strong> terms of “doubl<strong>in</strong>g” the anterior <strong>in</strong>ferior mandibular<br />
with genial tubercle advancement for orohypopharyngeal enlargement.<br />
The AIMO used as an <strong>in</strong>tegral component of MMA is a<br />
modification of previously reported similar osteotomies.<br />
33,35,36,42,43,58 This new trapezoid-shaped osteotomy, which<br />
preserves ch<strong>in</strong> contour and muscle attachments, is made with one<br />
cont<strong>in</strong>uous bony cut and no sharp angles so as to m<strong>in</strong>imize risk of<br />
anterior mandibular fracture. 43 The cut is directed superiorly<br />
toward the l<strong>in</strong>gual cortex to ensure capture of the entire genial<br />
tubercles, but yet stay<strong>in</strong>g <strong>in</strong>ferior labially to avoid cutt<strong>in</strong>g teeth<br />
apices. 43 Physiologic (<strong>in</strong>direct) hyoid suspension via anterosuperior<br />
tension on the <strong>in</strong>tact suprahyoid musculature obviates additional<br />
hyoid surgery, (eg, hyoid myotomy for suspension with<br />
fascia lata 36,43 or hyoid fixation to the thyroid cartilage.) 59 The<br />
distal segment is advanced maximally the full thickness of the<br />
bicortical region and secured with <strong>in</strong>terosseous wire fixation with<br />
a resultant protrusive ch<strong>in</strong> and m<strong>in</strong>imal bony contact that<br />
warrants concomitant (1) allogeneic cancellous bone graft<strong>in</strong>g to<br />
prevent soft-tissue <strong>in</strong>growth between the osteotomy segments<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013<br />
and to promote a complete bony union; and (2) reduction<br />
osteoplasty of the distal segment’s labial cortex for a tension-free<br />
soft-tissue closure to prevent wound dehiscence and <strong>in</strong>fection.<br />
In addition to LF, BSSRO, and AIMO, which were performed<br />
<strong>in</strong> all 50 cases, several adjunctive nonpharyngeal procedures were<br />
performed concomitantly, when <strong>in</strong>dicated (Table 1). Septoplasty<br />
and turb<strong>in</strong>ate reduction were performed <strong>in</strong> 28 and 26 patients<br />
with septal deviation and turb<strong>in</strong>ate hypertrophy, respectively.<br />
Enlargement of the piriform rims for additional relief of nasal<br />
obstruction, as well as removal of polypoid antral tissues (for<br />
biopsy) <strong>in</strong> 13 patients with chronic s<strong>in</strong>us problems were also<br />
performed with the maxilla down-fractured. Cervicofacial subcutaneous<br />
lipectomy was performed <strong>in</strong> 26 cases via a syr<strong>in</strong>geaspiration<br />
technique. Because weight loss may reduce OSA by a<br />
proportionate reduction of adipose tissue affect<strong>in</strong>g the airway,<br />
selective removal of bulky adipose tissue from the cervicofacial<br />
area might reduce the weight of these tissues aga<strong>in</strong>st the<br />
underly<strong>in</strong>g tongue-related muscles, which are <strong>in</strong> a state of flaccid<br />
paralysis dur<strong>in</strong>g sleep and, thus, might reduce the extralum<strong>in</strong>al<br />
soft-tissue forces of collapse aga<strong>in</strong>st the posterior pharyngeal<br />
walls, particularly when sup<strong>in</strong>e. In one patient, bilateral anterior<br />
mandibular l<strong>in</strong>gual tori were removed to <strong>in</strong>crease tongue space <strong>in</strong><br />
the mouth floor.<br />
Postsurgical Management and Evaluation<br />
Because the UAs were immediately more patent after MMA<br />
and to m<strong>in</strong>imize potential ETT-<strong>in</strong>duced glottic edema, early ETT<br />
extubation was accomplished, even <strong>in</strong> the sett<strong>in</strong>g of maxillomandibular<br />
fixation, usually <strong>in</strong> the operat<strong>in</strong>g room before patient<br />
transport to the recovery area. A long-act<strong>in</strong>g local anesthetic,<br />
0.5% bupivaca<strong>in</strong>e with 1:200,000 ep<strong>in</strong>ephr<strong>in</strong>e was <strong>in</strong>jected <strong>in</strong>traorally<br />
postsurgically for wound hemostasis and to m<strong>in</strong>imize the<br />
need for centrally-act<strong>in</strong>g opiate or opioid narcotics, which can<br />
cause respiratory depression. Patients were carefully monitored,<br />
<strong>in</strong>clud<strong>in</strong>g cont<strong>in</strong>uous pulse oximetry with paper pr<strong>in</strong>tout record<strong>in</strong>gs,<br />
<strong>in</strong> an ICU environment while wean<strong>in</strong>g off supplemental<br />
oxygen onto room air. Nurses and respiratory therapists were<br />
<strong>in</strong>structed to allow m<strong>in</strong>or desaturations of 90% on room air<br />
and without nCPAP, provided the lower limit established for<br />
each <strong>in</strong>dividual patient was significantly higher than preoperative<br />
diagnostic PSG LSAT, to determ<strong>in</strong>e the early postoperative OSA<br />
status to be expected <strong>in</strong> the patient’s home the follow<strong>in</strong>g nights.<br />
Patients were followed up with weekly visits at the author’s<br />
office for 3 months. Nutritional counsel<strong>in</strong>g was provided for<br />
liquids the first 2 weeks, followed by a strict nonchew<strong>in</strong>g diet for<br />
2 months. Controlled weight reduction was encouraged and often<br />
expedited by maxillomandibular fixation <strong>in</strong> the morbidly obese<br />
patients. Overnight PSG was performed by the referr<strong>in</strong>g sleep<br />
facility at approximately 7 weeks postoperatively. Additional PSG<br />
at 6 months postoperatively and annually thereafter was encouraged.<br />
BP, weight, cl<strong>in</strong>ical exam<strong>in</strong>ation, panoramic and cephalo-<br />
Table 2—Demographics, Orthodontics, and<br />
Hospital Stay*<br />
Characteristics Values<br />
Age, yr<br />
Gender<br />
42.7 (9.3) (19–66)<br />
Male 44<br />
Female 6<br />
Orthodontic therapy cases 4<br />
Hospital stay, No. of nights<br />
*Values given as No. or mean (SD) (range).<br />
1.65 (0.5) (1–2)<br />
CHEST / 116 /6/DECEMBER, 1999 1523
metric radiographs, and the patient’s symptoms were recorded by<br />
the same methods described above (<strong>in</strong> the presurgical evaluation)<br />
dur<strong>in</strong>g the office visit closest to (usually the day after) each PSG<br />
obta<strong>in</strong>ed. Statistical analysis was performed us<strong>in</strong>g the paired<br />
Student’s t test. A p value 0.05 determ<strong>in</strong>ed statistical significance.<br />
Mean values are presented with SD.<br />
Results<br />
Demographic data of the 50 MMA patients are<br />
summarized <strong>in</strong> Table 2. Forty-four patients were<br />
male and six were female. The mean age was 42.7<br />
years, with a range of 19 to 66 years. The postoperative<br />
data presented <strong>in</strong> Tables 3 –6 were obta<strong>in</strong>ed at<br />
the longest complete follow-up evaluation. The<br />
mean length of follow-up was 5.2 months, with the<br />
longest at 4 years 3 months postoperatively. PSG<br />
results are summarized <strong>in</strong> Table 3 and illustrated <strong>in</strong><br />
Figures 4 and 5. Postoperative results (n 50) show<br />
significant improvement <strong>in</strong> all variables of AI, AHI,<br />
LSAT, number of desaturations, and percent (%)<br />
stage3&4sleep, percent rapid eye movement sleep,<br />
and percent sleep efficiency as compared with preoperative<br />
data (n 50), with success similar to that<br />
of nCPAP (n 42). All 50 patients were successful<br />
responders to MMA based on the criteria of an<br />
LSAT 80%, an AHI 15, and AI 5ora 60%<br />
reduction <strong>in</strong> AHI and AI, with all patients hav<strong>in</strong>g an<br />
AI 10, for a success rate of 100%.<br />
OSAS-related symptoms, as subjectively reported<br />
by these patients, are shown <strong>in</strong> Table 4. Patients with<br />
preoperative EDS (n 50), memory loss (n 34),<br />
and impaired concentration (n 28) all reported<br />
amelioration of these symptoms. Snor<strong>in</strong>g was elim<strong>in</strong>ated<br />
<strong>in</strong> 44 of 50; depression, mood<strong>in</strong>ess, and/or<br />
irritability was reduced <strong>in</strong> 36 of 39; and morn<strong>in</strong>g<br />
headaches were alleviated <strong>in</strong> 28 of 29 patients. BP<br />
and body mass <strong>in</strong>dex (BMI) data are stated <strong>in</strong> Table<br />
5. Both systolic and diastolic pressures improved<br />
significantly, lower<strong>in</strong>g 15.0 and 9.6 mm Hg (difference<br />
of mean values), respectively (n 50). BMI<br />
(n 50) also improved significantly.<br />
Table 3—PSG Results*<br />
Variable Preoperative nCPAP Postoperative† p Value‡ p Value§<br />
AI 34.5 (27.9) 2.0 (4.0) 1.0 (1.9) 0.001 0.078<br />
AHI 59.2 (28.4) 5.4 (6.8) 4.7 (5.9) 0.001 0.306<br />
LSAT, % 72.7 (13.6) 88.6 (6.3) 88.6 (3.9) 0.001 0.450<br />
No. of desaturation events 90% 118.8 (160.7) 2.4 (4.7) 6.6 (12.2) 0.001 0.022<br />
% Stage 3 4 6.2 (13.6) 10.1 (14.1) 9.0 (13.6) 0.037 0.210<br />
% REM 9.9 (7.7) 23.1 (19.5) 16.5 (7.4) 0.001 0.036<br />
Sleep efficiency, % 83.2 (11.9) 83.1 (16.7) 86.7 (9.9) 0.054 0.139<br />
*Values given as mean (SD), unless otherwise <strong>in</strong>dicated. REM rapid eye movement sleep.<br />
†Obta<strong>in</strong>ed at 5.2 months (mean) postoperatively.<br />
‡Postoperative vs preoperative.<br />
§Postoperative vs nCPAP.<br />
Cephalometric results (n 50) are summarized <strong>in</strong><br />
Table 6. The average amount (difference of mean<br />
values) of maxillary (via LF) and mandibular (via<br />
BSSRO solely, without AIMO) advancement, as<br />
measured by SNA and SNB, was 7.4° and 6.9°,<br />
respectively. GO-POG showed an average advancement<br />
of the genial region (via the additive affects of<br />
AIMO together with BSSRO) of 14.4 mm. PAS<br />
enlarged considerably postoperatively, both at ETV<br />
(6.5 mm) and dur<strong>in</strong>g the MM (4.9 mm). PAS was<br />
more narrow dur<strong>in</strong>g the MM, consistent with hypopharyngeal<br />
collapse <strong>in</strong>duced by negative <strong>in</strong>spiratory<br />
forces generated aga<strong>in</strong>st an occluded UA. PNS-P<br />
shortened slightly, both at ETV (1 mm) and dur<strong>in</strong>g<br />
the MM (1.3 mm), because of anterosuperior tighten<strong>in</strong>g<br />
of the soft palate (via LF). MP-H results show<br />
the hyoid moved superiorly postoperatively, consistent<br />
with anterosuperior tension on the suprahyoid<br />
strap muscles attached to the anterior <strong>in</strong>ferior mandible<br />
(via AIMO <strong>in</strong> comb<strong>in</strong>ation with BSSRO).<br />
Discussion<br />
A comprehensive review of the OSA surgery literature<br />
33 showed that UPPP has been one of the most<br />
commonly performed, yet one of the least effective,<br />
surgeries for OSAS. Us<strong>in</strong>g the criteria of postoperative<br />
AHI 20 or AI 10 or 50% reduction <strong>in</strong><br />
either value, 137 of 337 patients from 37 <strong>in</strong>depen-<br />
Table 4—Subjective Symptoms<br />
Symptom Preoperative Postoperative*<br />
Excessive daytime sleep<strong>in</strong>ess 50 0<br />
Snor<strong>in</strong>g 50 6<br />
Depression, mood<strong>in</strong>ess, irritability 39 3<br />
Memory loss 34 0<br />
Morn<strong>in</strong>g headaches 29 1<br />
Impaired concentration 28 0<br />
*Obta<strong>in</strong>ed at 5.2 months (mean) postoperatively.<br />
1524 Cl<strong>in</strong>ical Investigations<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013
Table 5—BP and BMI*<br />
Variable Preoperative Postoperative† p Value<br />
BP<br />
Systolic 138.9 (15.6) 123.9 (13.8) 0.001<br />
Diastolic 89.8 (12.3) 80.2 (11.1) 0.001<br />
BMI 30.7 (4.5) 28.6 (3.9) 0.001<br />
*Values given as mean (SD), unless otherwise <strong>in</strong>dicated.<br />
†Obta<strong>in</strong>ed at 5.2 months (mean) postoperatively.<br />
dent case series were successful responders, for a<br />
comb<strong>in</strong>ed success rate of only 41%. Furthermore,<br />
surgery directly on the pharyngeal tissues, eg, soft<br />
palate, may produce life-threaten<strong>in</strong>g postoperative<br />
UA edema and permanent disfigurement with functional<br />
impairment. 33,51,52,54 Tracheostomy bypasses<br />
the entire UA with all its potential sites of obstruction<br />
but has significant psychosocial and medical<br />
management problems and, thus, is no longer recognized<br />
as an ideal treatment of OSAS <strong>in</strong> relatively<br />
healthy ambulatory patients. Exclud<strong>in</strong>g tracheostomy,<br />
MMA, which opens the entire velo-orohypopharynx<br />
34 via an extrapharyngeal operation with m<strong>in</strong>imal<br />
risks of UA embarrassment or pharyngeal<br />
dysfunction, is the most effective surgical treatment<br />
of OSAS.<br />
Riley et al 36 reported the largest series of maxillomandibular<br />
osteotomies (MMO), <strong>in</strong> which 89 of 91<br />
OSAS patients were successfully treated, based on<br />
postoperative AHI 20 or 50% reduction <strong>in</strong> AHI,<br />
for a success rate of 98%. However, it is perhaps<br />
mislead<strong>in</strong>g that MMO was labeled a phase II procedure<br />
<strong>in</strong> that 67 of the 91 patients did not participate<br />
<strong>in</strong> phase I of their two-phase protocol. Waite et al 35<br />
reported improvement <strong>in</strong> 22 of 23 patients, based on<br />
a mean postoperative AHI of 15, for a success rate of<br />
96%, <strong>in</strong> which MMA was performed as a primary<br />
procedure, often <strong>in</strong> comb<strong>in</strong>ation with adjunctive<br />
Table 6—Lateral Cephalometric Analysis*<br />
Cephalometric Analysis Preoperative Postoperative† p Value<br />
SNA, degrees 79.0 (4.2) 86.4 (4.1) 0.001<br />
SNB, degrees 74.7 (4.1) 81.6 (4.1) 0.001<br />
GO-POG, mm<br />
PNS-P, mm<br />
72.1 (4.7) 86.5 (5.7) 0.001<br />
ETV 37.9 (6.7) 36.9 (6.0) 0.003<br />
MM<br />
MP-H, mm<br />
39.6 (6.8) 38.3 (6.4) 0.001<br />
ETV 24.3 (5.8) 22.4 (6.0) 0.002<br />
MM<br />
PAS, mm<br />
37.1 (10.6) 33.7 (9.0) 0.003<br />
ETV 5.1 (2.4) 11.6 (3.4) 0.001<br />
MM 0.8 (1.5) 5.7 (3.9) 0.001<br />
*Values given as mean (SD), unless otherwise <strong>in</strong>dicated.<br />
†Obta<strong>in</strong>ed at 5.2 months (mean) postoperatively.<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013<br />
Figure 4. PSG results, sleep-disordered breath<strong>in</strong>g variables.<br />
Error bars <strong>in</strong>dicate SD. CPAP cont<strong>in</strong>uous positive airway<br />
pressure; #Desats number of oxyhemoglob<strong>in</strong> desaturation<br />
events; Pre-op preoperative; Post-op postoperative.<br />
procedures. Hochban et al 34 reported a 95% success<br />
rate, based on relatively rigid criterion of postoperative<br />
AHI 10 <strong>in</strong> a series of 21 consecutive OSAS<br />
cases <strong>in</strong> which MMA was performed as a def<strong>in</strong>itive<br />
primary surgery, without any adjunctive procedures.<br />
In Hochban’s series of carefully selected cases,<br />
which <strong>in</strong>cluded only healthy nonobese patients with<br />
specific craniofacial skeletal deformities and pharyngeal<br />
narrow<strong>in</strong>g, a “stepwise” algorithm of staged<br />
surgical procedures was “not justified.” 34<br />
A difficult diagnostic dilemma is decid<strong>in</strong>g when<br />
and how to stage surgery <strong>in</strong> patients with diffusely<br />
Figure 5. PSG results, sleep-stag<strong>in</strong>g variables, shown as a<br />
percentage of total sleep time. Error bars <strong>in</strong>dicate SD.<br />
REM rapid eye movement.<br />
CHEST / 116 /6/DECEMBER, 1999 1525
complex or multiple sites of disproportionate UA<br />
anatomy. One approach is to perform certa<strong>in</strong> procedures<br />
<strong>in</strong> a stepwise 32 manner or particular order<br />
accord<strong>in</strong>g to a methodical protocol, eg, UPPP first,<br />
then if unsuccessful, a hyoid suspension, then if that<br />
fails, a mandibular advancement, and so on. However,<br />
this may result <strong>in</strong> unnecessary additional surgery,<br />
which may be pa<strong>in</strong>ful, dysfunctional, expensive,<br />
nontherapeutic, and, ultimately, a deterrent for patients<br />
to seek def<strong>in</strong>itive surgical treatment. Riley et<br />
al 36 reported an overall success rate of only 61% (145<br />
of 239 patients) for phase I surgery, which consisted<br />
of UPPP and/or genioglossus advancement with<br />
hyoid myotomy suspension. Furthermore, only 24 of<br />
the 94 patients who had failed phase I surgery<br />
elected to proceed with phase II of their protocol,<br />
even though MMO was known to be highly<br />
successful.<br />
In this series, the approach and methodology of<br />
surgical treatment plann<strong>in</strong>g was site-specific: the<br />
selection of specific surgical procedures was based<br />
primarily on each <strong>in</strong>dividual patient’s sites of disproportionate<br />
UA anatomy. MMA was performed first<br />
for diffusely complex or multiple sites of disproportionate<br />
UA anatomy to enlarge and stabilize the<br />
velo-orohypopharyngeal airway to either (1) def<strong>in</strong>itively<br />
treat the OSAS and, thus, elim<strong>in</strong>ate additional<br />
unwarranted surgery or (2) reduce the risk of postoperative<br />
edema-<strong>in</strong>duced UA embarrassment caused<br />
by secondary pharyngeal procedures, if still necessary<br />
<strong>in</strong> the sett<strong>in</strong>g of cl<strong>in</strong>ically significant residual<br />
OSAS. Unlike other less successful procedures, 33<br />
which focus on particular anatomic structures or<br />
segmental areas by operat<strong>in</strong>g with<strong>in</strong> the UA, MMA<br />
addresses the entire velo-orohypopharynx by operat<strong>in</strong>g<br />
outside of the pharyngeal airway tissues. MMA<br />
was not conf<strong>in</strong>ed by a stag<strong>in</strong>g algorithm and reserved<br />
only for the most severe OSAS cases as a last resort<br />
when all other surgery had failed; nor was it restricted<br />
to a set of craniofacial skeletal characteristics.<br />
Rather, it was also performed <strong>in</strong> some patients<br />
with mild OSAS, as well as <strong>in</strong> some who did not<br />
exhibit craniofacial skeletal deformities such as retrognathia.<br />
The results show that MMA, often performed<br />
concomitantly with adjunctive nonpharyngeal procedures,<br />
was a safe and successful primary s<strong>in</strong>glestaged<br />
operation—even for those with morbid obesity<br />
and coexist<strong>in</strong>g lateral pharyngeal tonsillar<br />
hypertrophy and/or dysmorphic soft palates with<br />
medially displaced tonsillar pillars. T/A and/or UPPP<br />
were not required subsequently <strong>in</strong> any of the 24 or<br />
40 patients <strong>in</strong> whom T/A or UPPP, respectively, had<br />
not been performed before MMA (Table 1). Nevertheless,<br />
those patients were <strong>in</strong>formed that with advanc<strong>in</strong>g<br />
age and/or weight ga<strong>in</strong>, the UA could pro-<br />
gressively narrow to such a degree as to necessitate<br />
T/A and/or UPPP as second-stage surgery if applicable<br />
conservative therapies, eg, nCPAP, were not<br />
tolerated, refused, or unsuccessful. In the sett<strong>in</strong>g of<br />
variable complex UA heterogeneity of the OSAS<br />
population referred for MMA, particularly <strong>in</strong> those<br />
with scar distortion from prior, often dissimilar surgery<br />
<strong>in</strong> which anatomically similar cohorts are not<br />
readily discernible, it is unknown how each <strong>in</strong>dividual<br />
procedure contributed to the results <strong>in</strong> this, as<br />
well as other, uncontrolled cl<strong>in</strong>ical case series.<br />
The surgical pr<strong>in</strong>ciples and techniques <strong>in</strong>troduced<br />
<strong>in</strong> this series (eg, <strong>in</strong>corporation of the <strong>in</strong>novative<br />
AIMO with BSSRO and LF as an <strong>in</strong>tegral component<br />
of MMA, the understand<strong>in</strong>g of which and when<br />
nonpharyngeal adjunctive procedures can be performed<br />
safely with MMA vs staged operations, early<br />
ETT extubation, and avoidance of narcotic analgesics)<br />
may have served to hasten postoperative recovery<br />
and convalescence, with m<strong>in</strong>imal morbidity and<br />
no mortality. Waite et al 35 and Riley et al 36 reported<br />
mean hospital stays of 7.8 and 2.4 days, respectively.<br />
The results (Table 2) <strong>in</strong> this series show a mean<br />
hospital stay of 1.6 days: no patient required a<br />
hospital stay of 2 days; and 21 of the last 23<br />
patients were discharged home on the first postoperative<br />
day. There were no episodes of postoperative<br />
hemorrhage or edema-<strong>in</strong>duced UA embarrassment,<br />
and postoperative nCPAP was not used <strong>in</strong> any<br />
patient. Postoperative discomfort was typically m<strong>in</strong>imal.<br />
Those who experienced residual neurosensory<br />
deficits, the most common complication of MMA,<br />
reported significant resolution, which did not adversely<br />
affect their quality of life. MMA was not<br />
disfigur<strong>in</strong>g, eg, no facial scars because all <strong>in</strong>cisions<br />
were <strong>in</strong>traoral. On the contrary, all patients, especially<br />
those with preoperative craniofacial skeletal<br />
deformities such as retrognathia, accepted changes<br />
<strong>in</strong> facial appearances, predicted by preoperative<br />
computer imag<strong>in</strong>g, as aesthetically pleas<strong>in</strong>g. All resumed<br />
their normal lifestyles, usually return<strong>in</strong>g to<br />
work full-time with<strong>in</strong> 2 weeks postoperatively, with<br />
substantial improvement <strong>in</strong> their preoperative<br />
OSAS-related signs and symptoms.<br />
The results (Table 5) show that weight loss and a<br />
lower<strong>in</strong>g of systolic and diastolic BP occurred after<br />
MMA. Riley et al 40 reported that 7 of 13 MMO<br />
patients no longer required antihypertensive medic<strong>in</strong>es.<br />
Although OSAS can exacerbate and perhaps<br />
cause some cases of hypertension, these results<br />
suggest that resolution of OSAS after MMA may<br />
normalize hypertension <strong>in</strong> some cases. However, the<br />
hemodynamic significance of these data is unknown.<br />
Initial weight reduction, particularly <strong>in</strong> the morbidly<br />
obese, resulted primarily from controlled dietary<br />
restrictions, whereas weight loss ma<strong>in</strong>tenance after<br />
1526 Cl<strong>in</strong>ical Investigations<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013
estoration of normal masticatory function may have<br />
resulted, <strong>in</strong> part, from <strong>in</strong>creased metabolic rates<br />
associated with the resolution of OSAS-related EDS.<br />
It is unknown to what extent the weight loss contributed<br />
to the PSG results and whether those patients<br />
might eventually ga<strong>in</strong> or rega<strong>in</strong> weight and, therefore,<br />
experience progressive worsen<strong>in</strong>g of any residual<br />
OSAS. Furthermore, the relatively low mean<br />
BMI <strong>in</strong> this series may not represent the true general<br />
OSAS population. Other limitations of the results are<br />
that record<strong>in</strong>g the patients’ stated symptoms (Table<br />
4) was subjective and qualitative; and that potential<br />
variability <strong>in</strong> the methodology of data collection and<br />
<strong>in</strong>terpretation by different sleep facilities and physicians<br />
existed.<br />
The PSG results also support the use of cephalometry,<br />
although obta<strong>in</strong>ed <strong>in</strong> awake erect patients, as a<br />
reliable diagnostic adjunct to cl<strong>in</strong>ical exam<strong>in</strong>ation.<br />
Although only ETV PAS 9 mm was used as an<br />
MMA <strong>in</strong>clusion criterion, the cephalometric data<br />
(Table 6) show that the maxilla and mandible advanced,<br />
the hyoid elevated, the soft palate tightened,<br />
and, most important, the orohypopharynx enlarged<br />
postoperatively. In comparison with other reputable<br />
diagnostic modalities (eg, <strong>in</strong>vasive nasopharyngolaryngoscopy,<br />
<strong>in</strong>tralum<strong>in</strong>al pressure transducers,<br />
somnoflouroscopy, CT scans, and MRI), cephalometry<br />
is comfortably non<strong>in</strong>vasive, safe with m<strong>in</strong>imal<br />
radiation exposure, easy to perform <strong>in</strong> an outpatient<br />
sett<strong>in</strong>g, <strong>in</strong>expensive, and with results that are objective,<br />
standardized, and reproducible.<br />
Two cephalometric modifications have been <strong>in</strong>troduced.<br />
First, PAS was selected as the most critical<br />
measurement <strong>in</strong> that it quantitated (<strong>in</strong> a two-dimensional<br />
plane viewed laterally) the (velo)-orohypopharyngeal<br />
open<strong>in</strong>g and, thus, was measured at the most<br />
narrow level of orohypopharyngeal anteroposterior<br />
collapse, rather than at a level determ<strong>in</strong>ed by skeletal<br />
landmarks. Second, pharyngeal volumetric changes<br />
associated with different phases of respiration were<br />
standardized by obta<strong>in</strong><strong>in</strong>g two films—one at ETV<br />
and the other dur<strong>in</strong>g MM, to simulate pharyngeal<br />
soft-tissue collapse associated with negative <strong>in</strong>spiratory<br />
forces generated dur<strong>in</strong>g OSA events. The results<br />
show that PAS (1) enlarged significantly after MMA<br />
<strong>in</strong> all patients and (2) was always larger at ETV than<br />
dur<strong>in</strong>g an MM, which suggests that the measurement<br />
of PAS should be standardized for breath<strong>in</strong>g<br />
phases.<br />
The relatively short-term success of MMA <strong>in</strong> this<br />
series may equate with a def<strong>in</strong>itive cure. Progressive<br />
worsen<strong>in</strong>g of OSAS <strong>in</strong> adults may be caused, <strong>in</strong> part,<br />
by ag<strong>in</strong>g of anatomically disproportionate pharyngeal<br />
soft tissues, which gradually lose neuromuscular<br />
tone, lead<strong>in</strong>g to <strong>in</strong>creas<strong>in</strong>g flopp<strong>in</strong>ess and collapsibility.<br />
In addition to structural enlargement of the<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013<br />
pharyngeal lumen, MMA via tighten<strong>in</strong>g of the pharyngeal<br />
soft tissues attached to or suspended from<br />
the advanced skeletal structures may also enhance or<br />
rejuvenate neuromuscular tone of the anterior pharyngeal<br />
dilator musculature, such as the tensor palat<strong>in</strong>i<br />
and genioglossus, to both open and stabilize the<br />
entire velo-orohypopharyngeal airway. Although<br />
these rejuvenated tissues will cont<strong>in</strong>ue to lose neuromuscular<br />
tone with advanc<strong>in</strong>g age, advancement<br />
LF and BSSRO, which have been performed rout<strong>in</strong>ely<br />
and successfully for half a century (eg, as<br />
orthognathic surgery) do not relapse significantly, <strong>in</strong><br />
that osteotomies, once healed to a bony union, are<br />
relatively stable. Hence, the surgically improved or<br />
corrected UA may be sufficiently patent and stable<br />
as to simulate an anatomically and physiologically<br />
normal UA, which can withstand normal soft-tissue<br />
ag<strong>in</strong>g without redevelop<strong>in</strong>g OSAS.<br />
MMA as a potential def<strong>in</strong>itively successful primary<br />
s<strong>in</strong>gle-staged surgical treatment of OSAS, particularly<br />
when performed <strong>in</strong> a relatively young OSAS<br />
population, may result <strong>in</strong> a significant reduction <strong>in</strong><br />
OSAS-related health risks (eg, hypertension, cardiovascular<br />
dysrhythmias, stroke, and myocardial <strong>in</strong>farction,<br />
as well as EDS-<strong>in</strong>duced <strong>in</strong>juries such as motor<br />
vehicular accidents and neuropsychiatric disorders<br />
such as depression and cognitive dysfunction),<br />
which, when projected over a normal lifetime,<br />
should represent a considerable f<strong>in</strong>ancial sav<strong>in</strong>gs on<br />
the health-care system. 60,61 The one-time costs of<br />
early MMA is probably far less expensive than<br />
multiple less successful operations (with multiple<br />
hospitalizations), or even a lifetime of nCPAP with<br />
its associated costs of repeat sleep studies, eg, retitrations,<br />
equipment ma<strong>in</strong>tenance and replacement,<br />
technical support, and compliance counsel<strong>in</strong>g.<br />
Conclusion<br />
This cl<strong>in</strong>ical series of 50 consecutive OSAS patients<br />
reports a 100% success rate of MMA, often<br />
performed concomitantly with adjunctive nonpharyngeal<br />
procedures, as a safe primary s<strong>in</strong>gle-staged<br />
type of site-specific surgical treatment for selected<br />
patients with diffusely complex or multiple sites of<br />
disproportionate velo-orohypopharyngeal anatomy.<br />
Although there is variation <strong>in</strong> the OSAS literature as<br />
to what specific criteria determ<strong>in</strong>e success, these<br />
results support previously reported data that MMA is<br />
the best surgical alternative to tracheostomy, with a<br />
therapeutic efficacy equal to nCPAP. The long-term<br />
validity and significance of these results, as well as<br />
the <strong>in</strong>novative techniques and postulates presented,<br />
are unknown. Additional studies with larger numbers<br />
of patients and longer follow-up are warranted.<br />
CHEST / 116 /6/DECEMBER, 1999 1527
ACKNOWLEDGMENTS: The author thanks Manuel Davila,<br />
DMD, Robert Lazerson, DDS, and Roger Meyer, DDS, MD, for<br />
assistance dur<strong>in</strong>g surgery; the sleep facilities listed <strong>in</strong> the appendix<br />
and the follow<strong>in</strong>g sleep physicians, listed alphabetically, for<br />
patient referrals and PSG data (Hal Alpert, MD, Maher Astwani,<br />
MD, Robert Bashuk, MD, Francis Buda, MD, Ralph Ciccone,<br />
MD, David DeRuyter, MD, William Dowdell, MD, Dale Green,<br />
MD, Aris Iatridis, MD, Walter James, MD, George Kanes, MD,<br />
Scott Karl<strong>in</strong>, MD, John Lee, MD, David Lesch, MD, Mark<br />
Pollock, MD, Russell Rosenberg, PhD, Robert Schnapper, MD,<br />
Trammell Starr, MD, Jonne Walter, MD, James Wellman, MD,<br />
Charles Wells, Jr, MD, David Westerman, MD, and Kev<strong>in</strong> Ziffra,<br />
MD); Simon Peimer, MD, PhD, for statistical analysis of this<br />
data; and Karen Cary, Misty Gendron, and Shay Hammonds for<br />
clerical assistance <strong>in</strong> manuscript preparation.<br />
Appendix<br />
PSGs were performed and <strong>in</strong>terpreted at the follow<strong>in</strong>g facilities,<br />
which are listed alphabetically: Astwani Neurology, P.C.,<br />
Sleep Disorders Lab, Dubl<strong>in</strong>, GA; Athens Regional Medical<br />
Center, Neurodiagnostics and Sleep Lab, Athens, GA; Cape Fear<br />
Memorial Hospital, Inc., Sleep Disorders Center, Wilm<strong>in</strong>gton,<br />
NC; Cobb Hospital, Sleep Center, Austell, GA; Dekalb Medical<br />
Center, Sleep Disorders Center, Decatur, GA; Dunwoody Medical<br />
Center, Sleep/Wake Center, Atlanta, GA; Floyd Medical<br />
Sleep Disorders Center, Rome, GA; Georgia Baptist Medical<br />
Center, Atlanta Center for Sleep Disorders, Atlanta, GA; Kennestone<br />
Hospital, Sleep Disorders Center, Marietta, GA; National<br />
Sleep Dynamics, Woodstock, GA; Neurology Associates,<br />
Neurodiagnostic and Sleep Disorders Center, Macon, GA; N.<br />
Broward Medical Center, Sleep Disorders Center, Pompano<br />
Beach, FL; Northlake Regional Medical Center, Sleep Disorders<br />
Laboratory, Tucker, GA; Northside Hospital, Sleep Disorders<br />
Center, Atlanta, GA; Piedmont Hospital, Sleep Laboratory,<br />
Atlanta, GA; Redmond Regional Medical Center, Sleep Disorders<br />
Center, Rome, GA; Sleep Disorders Center of Georgia,<br />
Atlanta, GA; and Staten Island University Hospital, Sleep Disorders<br />
Center, Staten Island, NY.<br />
References<br />
1 Guillem<strong>in</strong>ault C, Part<strong>in</strong>en M, eds. Obstructive sleep apnea<br />
syndrome: cl<strong>in</strong>ical research and treatment. New York, NY:<br />
Raven Press, 1990; xv–xvii<br />
2 Guillem<strong>in</strong>ault C. Natural history, cardiac impact, and longterm<br />
follow-up of sleep apnea syndrome. In: Guillem<strong>in</strong>ault C,<br />
Lugaresi E, eds. Sleep/wake disorders: natural history, epidemiology,<br />
and long-term evolution. New York, NY: Raven<br />
Press, 1983; 107–125<br />
3 Part<strong>in</strong>en M, Jamieson A, Guillem<strong>in</strong>ault C. Long-term outcome<br />
for obstructive sleep apnea syndrome patients: mortality.<br />
Chest 1988; 94:1200–1204<br />
4 He J, Kryger M, Zorick F, et al. Mortality and apnea <strong>in</strong>dex <strong>in</strong><br />
obstructive sleep apnea: experience <strong>in</strong> 385 male patients.<br />
Chest 1988; 94:9–14<br />
5 National Commission on Sleep Disorders Research. A report<br />
of the National Commission on Sleep Disorders Research:<br />
wake up America; a national sleep alert. Wash<strong>in</strong>gton, DC: US<br />
Government Pr<strong>in</strong>t<strong>in</strong>g Office, 1995; 2:10<br />
6 Kuna ST, Sant’ Ambrogio G. Pathophysiology of upper airway<br />
closure dur<strong>in</strong>g sleep. JAMA 1991; 266:1384–1389<br />
7 Sullivan CE, Grunste<strong>in</strong> RR, Marrone O, et al. Sleep apneapathophysiology:<br />
upper airway and control of breath<strong>in</strong>g. In:<br />
Guillem<strong>in</strong>ault C, Part<strong>in</strong>en M, eds. Obstructive sleep apnea<br />
syndrome: cl<strong>in</strong>ical research and treatment. New York, NY:<br />
Raven Press, 1990; 49–69<br />
8 Remmers JE, DeGroot WJ, Sauerland EK, et al. Pathogenesis<br />
of upper airway occlusion dur<strong>in</strong>g sleep. J Appl Physiol 1978;<br />
44:931–938<br />
9 Tangel DJ, Mezzanotte WS, White DP. The <strong>in</strong>fluence of<br />
sleep on tensor palat<strong>in</strong>i EMG and upper airway resistance <strong>in</strong><br />
normal men. J Appl Physiol 1991; 70:2574–2581<br />
10 Sauerland EK, Harper RM. The human tongue dur<strong>in</strong>g sleep:<br />
electromyographic activity of the genioglossus muscle. Exp<br />
Neurol 1976; 51:160–170<br />
11 Hudgel DW. Pharmacologic treatment of obstructive sleep<br />
apnea. J Lab Cl<strong>in</strong> Med 1995; 126:13–18<br />
12 Davila DG, Hurt RD, Offord KP, et al. Acute effects of<br />
transdermal nicot<strong>in</strong>e on sleep architecture, snor<strong>in</strong>g, and<br />
sleep-disordered breath<strong>in</strong>g <strong>in</strong> non-smokers. Am J Respir Crit<br />
Care Med 1994; 150:469–474<br />
13 Edmonds LC, Daniels BK, Stanson AW, et al. The effects of<br />
transcutaneous electrical stimulation dur<strong>in</strong>g wakefulness and<br />
sleep <strong>in</strong> patients with obstructive sleep apnea. Am Rev Respir<br />
Dis 1992; 146:1030–1036<br />
14 Guillem<strong>in</strong>ault C, Powell NB, Bowman B, et al. The effect of<br />
electrical stimulation on obstructive sleep apnea syndrome.<br />
Chest 1995; 107:67–73<br />
15 Hoffste<strong>in</strong>, V. How and why should we stabilize the upper<br />
airway? Sleep 1996; 19:S57–S60<br />
16 Sullivan CE, Issa FG, Berthon-Jones M, et al. Reversal of<br />
obstructive sleep apnea by cont<strong>in</strong>uous positive airway pressure<br />
applied through the nares. Lancet 1981; 1:862–865<br />
17 Sanders MH, Moore SE, Eveslage J. CPAP via nasal mask: a<br />
treatment for occlusive sleep apnea. Chest 1983; 83:144–145<br />
18 N<strong>in</strong>o-Murcia G, Crowe C, Bliwise D, et al. Nasal CPAP:<br />
follow-up of compliance and adverse effects. Sleep Res 1987;<br />
16:398 [abstract].<br />
19 N<strong>in</strong>o-Murcia G, Crowe C, Bliwise DL, et al. Compliance and<br />
side effects <strong>in</strong> sleep apnea patients treated with nasal cont<strong>in</strong>uous<br />
positive airway pressure. West J Med 1989; 150:165–169<br />
20 Waldhorn RE, Herrick TW, Nguyen MC, et al. Long-term<br />
compliance with nasal cont<strong>in</strong>uous positive airway pressure<br />
therapy of obstructive sleep apnea. Chest 1990; 97:33–38<br />
21 Kribbs NB, Redl<strong>in</strong>e S, Smith PL, et al. Objective monitor<strong>in</strong>g<br />
of nasal CPAP usage <strong>in</strong> OSAS patients. Sleep Res 1991;<br />
20:270–271<br />
22 Kribbs NB, Pack AI, Kl<strong>in</strong>e LR, et al. Objective measurement<br />
of patterns of nasal CPAP use by patients with obstructive<br />
sleep apnea. Am Rev Respir Dis 1993; 147:887–895<br />
23 Reeves-Hoche MK, Meck R, Zwillich CW. Nasal CPAP: an<br />
objective evaluation of patient compliance. Am J Respir Crit<br />
Care Med 1994; 149:149–154<br />
24 Schmidt-Nowara W, Lowe A, Wiegand L, et al. Oral appliances<br />
for the treatment of snor<strong>in</strong>g and obstructive sleep<br />
apnea: a review. Sleep 1995; 18:501–510<br />
25 American Sleep Disorders Association. Practice for the treatment<br />
of snor<strong>in</strong>g and obstructive sleep apnea with oral appliances.<br />
Sleep 1995; 18:511–513<br />
26 Shepard JW Jr, Gefter WB, Guillem<strong>in</strong>ault C, et al. Evaluation<br />
of the upper airway <strong>in</strong> patients with obstructive sleep apnea.<br />
Sleep 1991; 14:361–371<br />
27 Launois SH, Feroah TR, Campbell WN, et al. <strong>Site</strong> of<br />
pharyngeal narrow<strong>in</strong>g predicts outcome of surgery for obstructive<br />
sleep apnea. Am Rev Respir Dis 1993; 147:182–189<br />
28 Smith PL, Gold AR, Meyers DA, et al. Weight loss <strong>in</strong> mildly<br />
to moderately obese patients with obstructive sleep apnea.<br />
Ann Intern Med 1985; 103:850–855<br />
29 Rub<strong>in</strong>ste<strong>in</strong> I, Colap<strong>in</strong>to N, Rotste<strong>in</strong> LE, et al. Improvement<br />
<strong>in</strong> upper airway function after weight loss <strong>in</strong> patients with<br />
obstructive sleep apnea. Am Rev Respir Dis 1988; 138:1192–<br />
1195<br />
30 Johnson D, Drenick EJ. Therapeutic fast<strong>in</strong>g <strong>in</strong> morbid obe-<br />
1528 Cl<strong>in</strong>ical Investigations<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013
sity: long-term follow-up. Arch Intern Med 1977; 137:1381–<br />
1382<br />
31 Bennett W. Dietary treatments of obesity. Ann NY Acad Sci<br />
1987; 499:250–263<br />
32 American Sleep Disorders Association. Practice parameters<br />
for the treatment of obstructive sleep apnea <strong>in</strong> adults: the<br />
efficacy of surgical modifications of the upper airway. Sleep<br />
1996; 19:152–155<br />
33 Sher AE, Schechtman KB, Piccirillo JF. The efficacy of<br />
surgical modifications of the upper airway <strong>in</strong> adults with<br />
obstructive sleep apnea syndrome. Sleep 1996; 19:156–177<br />
34 Hochban W, Bradendurg U, Peter JH. Surgical treatment of<br />
obstructive sleep apnea by maxillomandibular advancement.<br />
Sleep 1994; 17:624–629<br />
35 Waite PD, Wooten V, Lachner J, et al. <strong>Maxillomandibular</strong><br />
advancement surgery <strong>in</strong> 23 patients with obstructive sleep<br />
apnea syndrome. J Oral Maxillofac Surg 1989; 47:1256–1261<br />
36 Riley RW, Powell NB, Guillem<strong>in</strong>ault C. Obstructive sleep<br />
apnea syndrome: a review of 306 consecutively treated surgical<br />
patients. Otolaryngol Head Neck Surg 1993; 108:117–<br />
125<br />
37 Riley RW, Powell NB, Guillem<strong>in</strong>ault C. Obstructive sleep<br />
apnea syndrome: a surgical protocol for dynamic upper airway<br />
reconstruction. J Oral Maxillofac Surg 1993; 51:742–747<br />
38 Jamieson A, Guillem<strong>in</strong>ault C, Part<strong>in</strong>en M, et al. Obstructive<br />
sleep apneic patients have craniomandibular abnormalities.<br />
Sleep 1986; 9:469–477<br />
39 Hochban W, Kunkel M, Bradenburg U. Functional anatomy<br />
of the upper respiratory tract: cephalometry and acoustic<br />
rh<strong>in</strong>ometry. Pneumologie 1993; 47:766–772<br />
40 Riley RW, Powell NB, Guillem<strong>in</strong>ault C. Maxillary, mandibular,<br />
and hyoid advancement for treatment of obstructive sleep<br />
apnea: a review of 40 patients. J Oral Maxillofac Surg 1990;<br />
48:20–26<br />
41 Riley R, Guillem<strong>in</strong>ault C, Herran J, et al. Cephalometric<br />
analysis and flow-volume loops <strong>in</strong> obstructive sleep apnea<br />
patients. Sleep 1983; 6:303–311<br />
42 Riley R, Powell N, Guillem<strong>in</strong>ault C. Current surgical concepts<br />
for treat<strong>in</strong>g obstructive sleep apnea syndrome. J Oral<br />
Maxillofac Surg 1987:149–157<br />
43 Riley R, Powell NB, Guillem<strong>in</strong>ault C. Inferior mandibular<br />
osteotomy and hyoid myotomy suspension for obstructive<br />
sleep apnea: a review of 55 patients. J Oral Maxillofac Surg<br />
1989; 47:159–164<br />
44 Lugaresi E, Cirignotta F, Coccagna G, et al. Cl<strong>in</strong>ical significance<br />
of snor<strong>in</strong>g. In Saunders NA, Sullivan CE, eds: Sleep<br />
and breath<strong>in</strong>g. New York, NY: Marcel Dekker, 1984:283–297<br />
45 Rechtschaffen A, Kales A. A manual of standardized term<strong>in</strong>ology,<br />
techniques and scor<strong>in</strong>g system for sleep stages of<br />
human subjects. Wash<strong>in</strong>gton, DC: Public Health Service, US<br />
Government Pr<strong>in</strong>t<strong>in</strong>g Office, 1968<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 03/21/2013<br />
46 Fujita S, Conway W, Zorick F, et al. Surgical correction of<br />
anatomic abnormalities <strong>in</strong> obstructive sleep apnea syndrome:<br />
uvulopalatopharyngoplasty. Otolaryngol Head Neck Surg<br />
1981; 89:923–934<br />
47 Practice parameters for the use of laser-assisted uvulopalatoplasty:<br />
Standards of Practice Committee of the American<br />
Sleep Disorders Association. Sleep 1994; 17:744–748<br />
48 Djupesland G, Schrader H, Lyberg T, et al. Palatopharyngoglossoplasty<br />
<strong>in</strong> the treatment of patients with obstructive<br />
sleep apnea syndrome. Acta Otolaryngol Suppl (Stockh) 1992;<br />
492:50–54<br />
49 Miljeteig H, Tv<strong>in</strong>nereim M. Uvulopalatopharygoglossoplasty<br />
(UPPGP) <strong>in</strong> the treatment of the obstructive sleep apnea<br />
syndrome. Acta Otolaryngol Suppl (Stockh) 1992; 492:86–89<br />
50 Powell NB, Riley RW, Troell RJ, et al. Radiofrequency<br />
volumetric tissue reduction of the palate <strong>in</strong> subjects with<br />
sleep-disordered breath<strong>in</strong>g. Chest 1998; 113:1163–1174<br />
51 Fairbanks DN. Uvulopalatopharyngoplasty complications and<br />
avoidance strategies. Otolaryngol Head Neck Surg 1990;<br />
102:239–245<br />
52 Haavisto L, Suonpaa J. Complications of uvulopalatopharyngoplasty.<br />
Cl<strong>in</strong> Otolaryngol 1994; 19:243–247<br />
53 Zohar Y, F<strong>in</strong>kelste<strong>in</strong> Y, Talmi YP, et al. Uvulopalatopharyngoplasty:<br />
evaluation of postoperative complications, sequelae<br />
and results. Laryngoscope 1991; 101:775–779<br />
54 Esclamado RM, Glenn MG, McCulloch TM, et al. Perioperative<br />
complications and risk factors <strong>in</strong> the surgical treatment<br />
of obstructive sleep apnea syndrome. Laryngoscope 1989;<br />
99:1125–1129<br />
55 Bear SE, Priest JH. Sleep apnea syndrome: correction with<br />
surgical advancement of the mandible. J Oral Surg 1980;<br />
38:543–549<br />
56 Fujita S, Woodson BT, Clark JL, et al. Laser midl<strong>in</strong>e<br />
glossectomy as a treatment for obstructive sleep apnea.<br />
Laryngoscope 1991; 101:805–809<br />
57 Woodson BT, Fujita S. Cl<strong>in</strong>ical experience with l<strong>in</strong>gualplasty<br />
as part of the treatment of severe obstructive sleep apnea.<br />
Otolaryngol Head Neck Surg 1992; 107:40–48<br />
58 Johnson NT, Ch<strong>in</strong>n J. Uvulopalatopharyngoplasty and <strong>in</strong>ferior<br />
sagittal mandibular osteotomy with genioglossus advancement<br />
for treatment of obstructive sleep apnea. Chest 1994;<br />
105:278–283<br />
59 Riley RW, Powell NB, Guillem<strong>in</strong>ault C. Obstructive sleep<br />
apnea and the hyoid: a revised surgical procedure. Otolaryngol<br />
Head Neck Surg 1994; 11:717–721<br />
60 Kryger MH, Roos L, Delaive K, et al. Utilization of health<br />
care services <strong>in</strong> patients with severe obstructive sleep apnea.<br />
Sleep 1996; 19:S111–S116<br />
61 Ronald J, Delaive K, Roos L, et al. Health care utilization <strong>in</strong><br />
the 10 years prior to diagnosis <strong>in</strong> obstructive sleep apnea<br />
syndrome patients. Sleep 1999; 22:225–229<br />
CHEST / 116 /6/DECEMBER, 1999 1529